- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 21 Minutes

What Is the Donor Area in Hair Transplant?
What does “donor area” actually mean in hair transplant?
When we talk about the donor area in hair transplant surgery, we mean the part of the scalp that provides the grafts we move into thinning or bald areas. In simple terms, it is the area we borrow hair from. In hair transplant patients, this refers to the back and sides of the scalp, because the hair there is usually more resistant to the genetic process of hair loss than the hair on the top of the head.
This is one of the most important concepts in hair transplantation. A hair transplant does not create new hair. It redistributes existing hair. So the donor area is the place that makes the surgery possible in the first place.
Why is the donor area so important?
The donor area is one of the most important parts of the entire surgery. Many patients naturally focus on the front hairline because that is the part they see in the mirror every day. That is understandable. But from a surgeon’s point of view, I can tell you that the donor area is at least as important as the recipient area, and sometimes even more important.
The reason is simple. The donor area is limited. It is not an unlimited source of hair. It is your reserve. It is your hair bank. It is what we use today, and, if necessary, what we may still need to rely on in the future. If the donor area is used carelessly, aggressively, or without long-term planning, the consequences can stay with the patient for years.
That is why I always think not only about how many grafts I can extract, but also how many grafts I should leave behind.
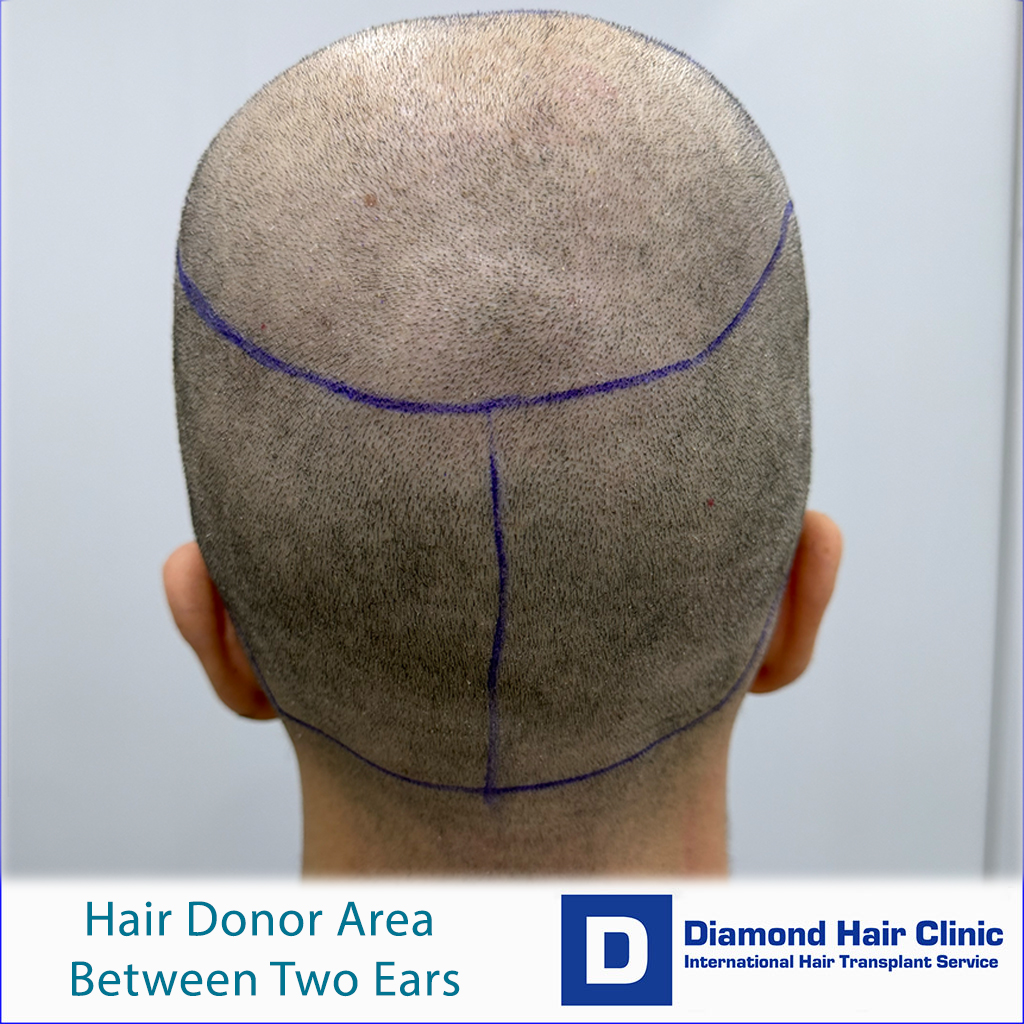
Where is the donor area located?
The donor area is mainly located in the back and sides of the scalp. However, that should not be misunderstood. Not every hair on the back and sides is equally safe or suitable for harvesting.
This is one detail patients often do not realize. Just because there is hair in a certain area does not mean all of it should automatically be used for transplantation. Some zones are more stable. Some are less stable. Some areas may look good today, but may not be the best long-term source if the patient’s hair loss continues to progress.
So when I evaluate a donor area, I am not just looking at whether there is hair there. I am looking at the quality of that hair, its density, caliber, future stability, and how safely it can be used without harming the donor’s overall appearance.
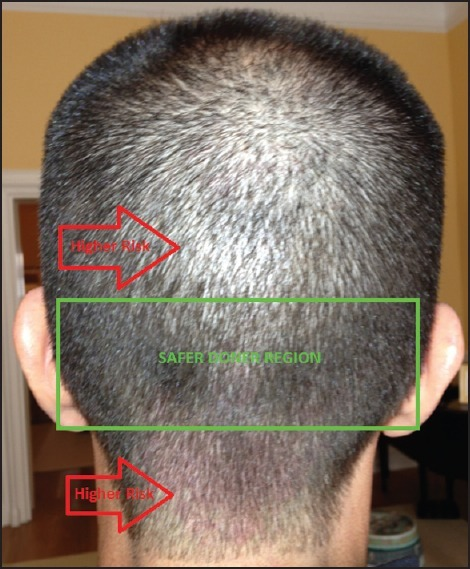
What is the safe donor area?
This is a very important question because many patients hear the term “donor area” and assume that the entire back and sides of the scalp are equally safe to harvest from. That is not really true.
The safer donor area is more limited than many patients think. In simple terms, it is the part of the donor zone that is more likely to remain stable over the years and less likely to be significantly affected by future hair loss. But even that safer area is not exactly the same for every patient. Some people have a broader, stronger safe donor zone, while others have a narrower, less reliable one.
This is why I never look at the donor as just “where there is hair.” The real question is whether that hair is likely to remain stable in the long term and whether it can be harvested without creating visible depletion later. One of the most common mistakes in poor hair transplant surgery is treating the broader back and sides as if all of it is equally safe. It is not.
Why are hairs taken from the donor area?
Donor hairs usually behave differently from the hairs in the balding area. In most men with androgenetic hair loss, the hairs on the top, front, and crown are more vulnerable to miniaturization and gradual loss. The hairs on the back and sides are usually more resistant.
That is why, when we move those hairs into the front or crown, they tend to keep much of their original behavior. This is the basic reason hair transplantation works.
So again, the surgery is not about creating something from nothing. It is about moving stronger follicles from a more stable area to a weaker one.
What exactly happens to the donor area in FUE?
In FUE, follicular units are extracted one by one from the donor area using very small punches. In modern practice, these punches are usually under 1 mm, and commonly around 0.8–1.0 mm for scalp harvesting. That detail matters because punch size affects both graft quality and donor appearance. A larger punch may reduce some technical difficulty, but creates more scar volume and more tissue trauma. A smaller punch may reduce scar size, but if it is used poorly, it can increase transection.
But in reality, good FUE is much more than just removing grafts one by one. The surgeon has to consider the angle of hair exit, the depth of punch penetration, the spacing between extractions, the density of the surrounding donor area, the thickness of the hair shafts, the skin characteristics, and the long-term preservation of donor reserve. If the extractions are too concentrated in one area, the donor can start to look patchy. If the harvesting is too aggressive overall, the donor can look thinned out or overharvested.
So in FUE, the donor area is not just the source of grafts. It is also the part that demands discipline, judgment, and restraint.
Does donor hair grow back after FUE?
No, the extracted follicles do not regrow in the same place after removal.
This is a very common misunderstanding. Patients sometimes hear people say that the donor heals, and they assume that means the extracted hairs return. That is not correct. What heals is the skin. The tiny wounds close. The area settles. The surrounding hairs help the donor blend visually. But the follicles that were removed from that exact spot are gone from that spot permanently.
This is exactly why donor management matters so much. A donor can heal beautifully and still look natural, but that happens because it was harvested properly, not because the extracted follicles magically regenerated.
Is FUE really scarless?
I do not like to call FUE scarless, because that is not medically accurate.
FUE does not leave the long linear scar associated with FUT, which is one reason many patients prefer it. But each extracted graft leaves a tiny wound, and every wound heals by forming a tiny scar. In a well-performed FUE procedure, these tiny scars are usually very small and difficult to notice, especially once healing is complete and the surrounding hair grows. But saying no scar is not correct.
I think patients deserve honesty in this area. FUE is minimally invasive compared to older methods, yes. But truly scarless, no.
What makes a donor area a good donor area?
A good donor area is not defined by a single factor. It is a combination of several factors. Density matters. Hair thickness matters. Hair-to-skin contrast matters. Curl can matter. The width and stability of the donor zone matter. The patient’s age matters. The likely future progression of hair loss matters.
A donor area may look full at first glance and still not actually be a strong donor. On the other hand, a donor area that does not look extraordinary can sometimes still be used very effectively if planned correctly.
This is why donor assessment should not be done carelessly or quickly. A proper assessment needs experience and long-term thinking.
How do I examine the donor area during a real consultation?
In real life, donor evaluation is much more than simply looking at the back of the head and saying whether it seems full. During consultation, I assess the donor from several angles and in good lighting. I assess density, hair shaft thickness, scalp-to-hair contrast, the presence or absence of miniaturization, the width of the safer donor zone, and whether the donor appears uniform or already shows signs of weakness. I also pay attention to how the patient normally wears the hair, because a donor that may look acceptable under longer hair might look much less forgiving if the patient prefers a short haircut.
I also think about the patient’s age, family history, current stage of hair loss, and likely future progression. These factors matter because a donor area should never be judged only for today. It has to be judged for tomorrow as well. Sometimes a donor looks decent at first glance, but closer evaluation shows that it is not as strong as the patient thinks. Sometimes the opposite is true. That is why donor assessment should be individualized, careful, and based on long-term planning rather than quick impressions.
How do I evaluate whether a donor area is strong or weak?
I do not judge a donor area only by whether it looks full from a distance. That would be far too superficial.
When I evaluate a donor, I look at donor density, hair shaft thickness, the contrast between scalp and hair color, the degree of miniaturization, the width of the safer donor zone, and the patient’s likely future hair-loss pattern. These details matter because two donors can look similar at first glance yet behave very differently in surgery and over the long term.
For example, a patient with thicker-caliber hair and lower scalp-to-hair contrast may achieve better visual coverage with fewer grafts than a patient with finer hair and stronger contrast. A donor that looks visually full may still be weak if there is significant miniaturization or if the stable donor zone is actually narrower than it appears. On the other hand, a donor that does not look extraordinary at first glance may still perform very well if the caliber and stability are good.
So a strong donor is not simply a donor that looks dense. It is a donor that can safely provide grafts while still remaining cosmetically natural afterward.
Can someone have hair at the back and still be a poor donor candidate?
Yes, absolutely.
A patient can have hair on the back and sides and still not be an ideal donor candidate. Sometimes the density is lower than it looks. Sometimes the hair is too fine. Sometimes the donor zone is not truly stable. Sometimes the patient has diffuse thinning. Sometimes the pattern of future loss is too advanced for the available donor reserve.
This is one of the reasons I do not like simplistic statements such as, “You have hair at the back, so you are a good candidate.” That is far too superficial. The real question is not whether there is hair there. The real question is whether that area can safely provide grafts while still preserving a natural donor appearance in the long term.
How many grafts can safely be taken from the donor area?
This is one of the most common questions in hair transplant consultation, and the honest answer is that there is no single number that fits every patient. A safe graft count depends on the strength of the donor area, the density, the hair caliber, the contrast between scalp and hair, the likely future progression of hair loss, and whether the patient may need another surgery later. That is why I do not like clinics that give the same high graft numbers to almost everyone as if donor capacity were standardized. It is not.
In some patients, the donor area is sufficient to allow a relatively generous extraction plan while preserving a natural appearance. In other patients, the donor must be used much more conservatively, even if the patient has a large bald area and wants a very aggressive result. The real question is not “What is the maximum number that can be extracted today?” The real question is “What is the safe number that can be extracted while still protecting the donor cosmetically and strategically for the future?” In my opinion, that is the number that truly matters.
Is the donor area the same in every patient?
No, not at all.
This is another area where patients are sometimes misled by oversimplified marketing. Donor areas are not identical from one patient to another. They differ in density, hair caliber, scalp characteristics, long-term stability, and the overall pattern of hair loss that may develop over time.
This is why I do not like standardized statements such as, “Everyone can get 4,000 or 5,000 grafts.” That is not how good surgery works. One patient’s donor area may tolerate a certain plan very well, while another patient’s donor area may require a much more conservative approach.
So the donor area should always be evaluated individually. One person’s donor cannot be compared too simply with another person’s.
Can the donor area also thin with age?
Yes, in some patients it can.
The donor area is usually more resistant to the common genetic process of hair loss, but that does not mean it is absolutely immune in every person forever. Some patients develop more diffuse thinning over time. Some show reverse thinning. Some have a donor zone that appears stable at one age but becomes less reliable later.
This is one of the reasons long-term planning matters so much. A surgeon should not think only about what looks safe today. He should also think about what is likely to remain safe in the future.
What is donor management in hair transplant?
Donor management is the part of hair transplant surgery that determines how the donor area will be used, how much can be safely harvested, from which zones grafts should be taken, how the extractions should be distributed, and how much donor reserve should be protected for the future.
In simple terms, donor management is not just about taking grafts out. It is about using a limited resource intelligently. The donor supply is finite, and every extraction has both short-term and long-term consequences.
Why is donor management so important?
Because a hair transplant can only be as good as the donor area allows. A patient may focus mainly on the front hairline, but from a surgeon’s perspective, one of the biggest responsibilities is to improve the front hairline without damaging the back and sides.
Poor donor management can lead to visible thinning, patchiness, a moth-eaten appearance, and fewer options for future procedures. Good donor management, on the other hand, helps the surgeon create a result that looks natural not only today, but also years later if the patient’s hair loss continues to progress.
What is the role of an experienced surgeon in donor management?
This is where the real difference between average surgery and proper surgery becomes obvious. Donor management is not a mechanical task. It is not simply a matter of removing as many grafts as possible until a target number is reached. An experienced surgeon has to decide not only how many grafts can technically be extracted, but how many should be extracted, from which exact zones they should be taken, how widely the extractions should be distributed, and how much donor reserve must be preserved for the future.
That decision is not based on a single factor. It depends on donor density, hair caliber, scalp-to-hair contrast, the width and long-term safety of the donor zone, the amount of miniaturization already present, the patient’s age, the likely future progression of hair loss, and the realistic possibility that the patient may need another surgery later. In some patients, the surgeon can safely be more generous. In others, the surgeon must be more conservative, even if the patient insists on a very large graft number. This is exactly why donor management requires judgment, restraint, and long-term thinking rather than short-term sales logic.
In my opinion, a truly experienced surgeon is always thinking in two directions at once. One direction is the immediate surgical goal: what can be achieved today in the recipient area? The other direction is donor preservation: what must still remain untouched and healthy for tomorrow? That second part is where many weak clinics fail. A surgeon who does not think carefully about the donor is not only risking the appearance of the back and sides of the scalp, but also risking the patient’s future repair options.
Why is the donor area one of the biggest risks in hair mill clinics?
In my opinion, the donor area is one of the clearest places where the difference between a proper one patient per day surgeon-led clinic and a hair mill becomes visible. Many patients see very cheap all-inclusive packages, often in the 3000–3500 Euro range, and convince themselves they are being clever. They assume that a hair transplant is basically the same surgery everywhere and that they are simply paying less for the same thing. But in reality, they are not buying the same surgery at all.
In hair mill clinics, there is no real surgeon creating a proper donor management plan in the way it should be done. These places may advertise themselves as doctor clinics, but once the patient enters the system, they are no-doctor clinics, just technician-driven mass-production lines. There may be no serious individualized planning of donor capacity, no thoughtful calculation of how much reserve to preserve, no careful mapping of safer versus less-safe donor zones, and no true surgeon-led control over the harvesting process. The donor area is often treated less as a limited biological reserve and more as raw material to be extracted quickly.
This problem is exacerbated by the extremely high daily patient turnover in many hair mills. Some of these clinics see 10–20 patients a day, sometimes more. Once a clinic starts operating at that kind of volume, speed inevitably begins to dominate quality. Donor extractions are more likely to be rushed. Punch angle and depth may be less carefully controlled. The spacing between extractions may be poorer. Too many grafts may be taken from the same limited zones. Harvesting may spread outside the safer donor area. The donor may be exposed to more unnecessary trauma and tissue injury than it should ever receive in a carefully performed surgery.
Another very important issue is graft transection. When donor harvesting is rushed, less precise, or performed by people who are working more like production staff than careful surgical operators, the transection rate of extracted grafts can increase. That means the clinic may injure or partially destroy more follicles during extraction. This is a double loss for the patient. The donor area still suffers the trauma of extraction, but the recipient area does not receive the full value of intact, high-quality grafts. In other words, the patient may spend part of his limited donor reserve while receiving a weaker graft quality at the same time. That is one of the worst combinations possible in hair transplant surgery.
This is why I always say that the donor area is where cheap surgery often reveals its true cost. On paper, the patient may feel proud of paying less. Later, the real price may appear in the mirror, a patchy donor, visible depletion, overharvesting, more noticeable scarring, reduced donor reserve, and fewer options for future repair work. In a proper one patient a day surgeon-led clinic, the donor area is managed as a limited and valuable reserve. In a hair mill, it is too often treated as a supply to be emptied into a high-speed system. And once a donor area is badly used, it cannot simply be reset.
What should a patient ask a clinic about the donor area before surgery?
This is a very important subject, because many patients ask detailed questions about the hairline and graft number, but not enough about the donor area. In my opinion, one of the smartest things a patient can do before surgery is to ask who will actually plan the donor extraction, who will perform it, how the clinic estimates safe donor capacity, how they try to avoid overharvesting, and how they plan for the possibility of future sessions if the patient’s hair loss continues.
Patients should also ask how many patients the clinic treats per day, how much direct surgeon involvement there is during donor harvesting, and whether the clinic prioritizes long-term donor preservation or only delivering a high graft count in a single session. These questions matter because the donor area is often where the quality difference between clinics becomes most obvious. A clinic that cannot clearly explain how it protects the donor is, in my opinion, not a clinic the patient should trust easily.
Can a good surgeon plan for two, and sometimes even three, hair transplant sessions?
Yes, in selected patients that is a very realistic part of long-term planning.
Not every patient should have multiple surgeries, but in some cases, especially younger patients, patients with progressive hair loss, or patients with extensive recipient demand, it is much wiser to think beyond a single session. Sometimes the best result is not to do everything in one operation. Sometimes the better decision is to perform a more conservative first surgery, allow the scalp to heal and the result to mature, then reassess both the donor reserve and the future needs.
That kind of planning is not a weakness. In my opinion, it is often a sign of better judgment and greater respect for the donor area.
Why are hair transplant sessions sometimes planned about a year apart?
Because both the scalp and the result need time. The recipient area needs time to grow and mature, the donor area needs time to settle, and the surgeon needs a clearer view of what was achieved before deciding what to do next.
In practical terms, spacing procedures apart allows better judgment of growth, better assessment of remaining donor capacity, and more thoughtful long-term planning rather than rushing into another extraction session too early.
How does donor capacity affect long-term planning?
Donor capacity is one of the most important limits in hair transplantation. Some patients have stronger donor density and thicker hair shafts, which gives more flexibility. Others have finer hair, lower density, or a broader future balding pattern, which means the surgeon has to be more conservative.
This is why good surgery is not only about designing a nice hairline. It is also about deciding how much of the donor should remain untouched for the future.
How is the donor area different in FUT?
In FUT, the donor area is still typically the back of the scalp, but the way grafts are obtained differs. Instead of removing follicular units one by one, a strip of scalp is taken from the donor area, and then the grafts are dissected from that strip.
So the donor concept is similar, but the harvesting method is different.
The biggest practical difference for patients is usually the scar pattern. FUT typically leaves a linear scar. FUE leaves many tiny scattered scars. That does not mean one method is always right and the other always wrong. It simply means the donor trade-offs are different.
In selected patients, FUT can still be useful. But when patients ask me about donor-area appearance, especially if they prefer shorter hairstyles, this difference matters a lot.
What about DHI? Is the donor area different in DHI?
This is an area where many patients get confused, because the marketing language can make it sound as if DHI is a completely different world. In reality, from the donor area’s perspective, the process of extracting grafts is exactly the same as FUE.
In DHI procedure, the grafts are still taken individually from the donor area, as in FUE. The main difference usually lies more in how the grafts are implanted into the recipient area than in the donor area itself.
That is why I usually tell patients not to get too distracted by labels alone. Whether a clinic says FUE or DHI, you still need to ask the same important donor questions. Where are the grafts coming from? How safely are they being harvested? How much donor reserve will remain afterward?
Can beard or body hair also be used as a donor area?
Sometimes yes, especially in selected cases.
The scalp donor area is usually the first and best source, but beard hair can also be useful in certain patients, especially when extra grafts are needed or when the scalp donor is limited. Body hair can sometimes be used as well, but that is usually much more case-specific.
I see beard and body hair as secondary donor sources, not as a replacement for proper scalp donor planning. They can be very helpful in the right hands and in the right case, but they should not become an excuse for poor management of the scalp donor.
Can donor hairs from different parts of the donor area be used for different purposes?
Yes, sometimes they can.
Not every hair in the donor area is exactly the same. Some regions may provide slightly thicker hairs, while others may provide relatively finer hairs. In practical terms, thicker grafts may be more useful when stronger visual density is desired, while finer grafts may sometimes be more suitable for softer and more delicate work in selected areas.
This is a more nuanced part of hair transplantation, but it is real. Good donor use is not only about how many grafts are taken. It is also about which grafts are used where.
Can the donor area be overharvested?
Yes, it can, and this is one of the most important risks of careless FUE.
If too many grafts are taken, or if they are taken too densely from certain zones, the donor area can appear visibly depleted. The patient may notice patchiness, thinning, irregular density, pinpoint scarring, lighter dots, or a moth-eaten appearance. In more severe cases, the donor can look cosmetically weak even after the hair has grown out.
This is why I always say that donor area management is where surgical discipline matters greatly. A surgeon should not chase numbers just because a patient wants an extremely high graft count, or because a clinic wants to advertise a large session. The donor has limits. Respecting those limits is part of good surgery.
Can the donor area be overharvested and repaired later?
Sometimes the appearance can be improved, yes, but prevention is always much better than repair.
In some overharvested donors, the situation can be improved by keeping the hair longer, using scalp micropigmentation, or, in selected cases, carefully placing grafts back into depleted areas. But these are secondary solutions. They are not a reason to be careless with the donor in the first place.
That is why I always prefer a conservative and intelligent use of the donor area rather than trying to fix a bad donor later.
What are the signs of a badly managed donor area?
A poorly managed donor area can manifest in several ways. One of the most obvious signs is visible patchiness that can still be seen under ordinary lighting and normal hair length, not only in extreme close-up photos. Some donors develop a moth-eaten appearance, in which the back and sides look uneven and visibly depleted. In other cases, the extractions may appear too concentrated in one zone, creating asymmetry or unnatural thinning. Sometimes the donor has been harvested too low or too high, outside the safer donor region, which may create even greater long-term problems.
Another sign is when the donor area looks cosmetically weak even after enough time has passed for healing and regrowth of the surrounding hair. Visible white dots, irregular density, poor blending, or a donor that cannot tolerate a normal haircut without looking depleted can all suggest poor donor management. In my opinion, a good donor should not only provide grafts. It should still look respectable afterward. If the front improves but the donor is left visibly damaged, that is not truly a good surgery.
Why do some donor areas look worse early on than they do later?
Because healing is a process.
After FUE, the donor area can look red, patchy, irritated, uneven, or visually thinner for a while. This can be especially dramatic in close-up photos, under harsh lighting, or when the hair is still very short. At that stage, patients often panic and think the donor has been permanently damaged.
But what they are seeing early is not always the final reality.
The donor area can look worse in the early weeks or months due to redness, temporary shock loss, scalp visibility, short hair length, and healing changes in the skin. In many cases, once the redness fades and the surrounding hair grows longer, the donor area blends much better and looks far more natural.
That is why I do not like very early judgments about the donor area. A donor area can look quite dramatic in the short term without becoming a bad long-term donor result.
Can the donor area look weak early after surgery even if it is not truly damaged?
Yes, absolutely.
This is something I see quite often in anxious post-operative patients. Early donor healing can create a visual impression that is worse than the long-term reality. Redness, short hair, temporary shock loss, and scalp visibility can all make the donor look weak, patchy, or uneven in the early period.
That does not automatically mean the donor has been permanently damaged or overharvested. Sometimes it simply means the donor is still healing. This is one reason why I always advise patience before making a final judgment about early donor appearance.
What is the difference between temporary donor healing and true donor damage?
This is one of the most misunderstood parts of post-operative donor assessment. Temporary donor healing can look much worse than the final reality, especially in the first weeks and months after FUE. Redness, short hair, temporary shock loss, scalp visibility, and early healing changes can all make the donor look weak, patchy, or uneven. That does not automatically mean the donor has been permanently damaged.
True donor damage is something different. It is not judged from a close-up photo taken too early. It is judged later, once healing has progressed, the surrounding hair has had time to grow, and the donor has had a fair chance to settle. If, after that point, the donor still looks visibly depleted, asymmetrical, overharvested, or cosmetically weak, then the concern becomes much more real. This distinction is very important, because many patients panic too early and confuse temporary healing changes with permanent donor damage. In my opinion, the donor should be judged with patience, context, and enough time for biology to do its work.
When do I allow patients to cut or shave the donor area after a hair transplant?
This is a question patients ask very often, and I know my own recommendation may sound more cautious than what some other clinics tell patients. In my own practice, I prefer that patients avoid haircuts on either the donor or recipient area for the first 6 months after surgery.
Why do I give that advice? Because even though the skin surface heals much earlier, the deeper biological recovery and the visual settling process take much longer. The donor area may still be going through redness, subtle inflammation, temporary shock loss, and gradual blending for months. The recipient area is also still in an early and fragile phase of growth, cycling, and cosmetic maturation. In my opinion, keeping both areas undisturbed during this period is simply the safer approach.
Another reason is that early haircuts, especially when clippers are used too closely or too aggressively, can cause unnecessary irritation, friction, and confusion during the healing process. Sometimes a patient gets a very short haircut too early, then starts staring at the donor area under bright light and panics because it suddenly looks more patchy or more visible than before. In reality, that does not always mean something has gone wrong. It may simply mean the donor was exposed too soon while it was still settling. I prefer to avoid that situation altogether.
I also believe that leaving the hair undisturbed for a longer period makes follow-up evaluation more reliable. It allows both the donor and recipient areas to mature more stably and reduces the risk that unnecessary grooming decisions will interfere with healing, appearance, or the patient’s perception of the result. So yes, I know six months may sound overcautious to some people, but as a surgeon, I believe it is a reasonable and protective recommendation.
Should medical treatment be considered before deciding on surgery?
Yes, in many patients it should.
In real practice, one of the most sensible approaches is to evaluate whether the patient’s hair loss should first be stabilized medically before committing to surgery. That is especially important when there is active progression, diffuse thinning, or uncertainty about how stable the donor and recipient areas really are.
Medical treatment before transplant is not just about improving hair. It is also about improving judgment and making better long-term surgical decisions.
Can medications make the donor area stronger before surgery?
Sometimes they can help stabilize and modestly improve the overall hair situation, especially when there is active miniaturization.
In practice, medications such as topical minoxidil, low-dose oral minoxidil, oral finasteride, and, in selected cases, oral dutasteride may help preserve existing native hair, slow progression, and improve the appearance of borderline areas. That can absolutely matter when planning a transplant. But they do not create a new donor supply out of nowhere. They may improve the condition of existing hair, but they do not turn a weak donor into an unlimited donor.
Can medications turn a patient who was previously not a good candidate into a good candidate?
Sometimes, yes, but only in certain borderline cases.
If the issue is ongoing miniaturization, unstable loss, or hair that needs medical stabilization before surgery, treatment may improve the situation enough that a previously borderline patient becomes a more reasonable candidate later.
But I would be careful not to overpromise this. Medication cannot create a new donor supply out of nowhere. It cannot turn a truly weak donor into a strong donor. It also does not solve every cause of hair loss. So the more accurate answer is this: medication can sometimes improve candidacy in borderline patients, but it cannot rescue every unsuitable case.
Can medications or supplements help the donor area recover after surgery?
They can sometimes help in the bigger picture, but they should not be presented as magic solutions.
Medications such as topical minoxidil 5%, topical minoxidil 2% in some patients, low-dose oral minoxidil in selected cases, and oral finasteride 1 mg/day for appropriate male patients can help support native hair, slow ongoing miniaturization, and improve the overall quality of the scalp hair over time. In selected male patients, oral dutasteride 0.5 mg/day may also be considered under proper medical supervision. These treatments can help stabilize the broader hair situation, which may indirectly benefit how the donor and surrounding scalp look over time, but they do not instantly repair the donor area or erase the visual effects of recent FUE extraction. They are supportive, longer-term treatments rather than quick fixes. Depending on the patient and the surgeon’s protocol, topical minoxidil is often restarted after the early healing phase rather than immediately.
As for supplements, I would keep the wording supportive but more selective. If a patient has poor nutrition, low ferritin or iron deficiency, low vitamin D, low zinc, or another documented deficiency, targeted supplementation may be reasonable and support overall hair health during recovery. Biotin is one of the most commonly marketed “hair vitamins,” but it should not be oversold, because it is mainly useful when there is an actual deficiency, and high biotin intake can interfere with certain blood tests. So I would describe supplements as supportive and individualized rather than transformative.
Can PRP or similar treatments help the donor area before or after hair transplant surgery?
PRP, which stands for platelet-rich plasma, is one of the most commonly discussed supportive treatments in hair transplantation. In my opinion, PRP should be understood as a possible adjunct rather than a miracle treatment. PRP may have real value in selected cases, but it is not a magical or perfectly standardized treatment.
Before surgery, PRP may be used in selected patients with miniaturization, weaker surrounding native hair, or a generally borderline scalp condition that might benefit from some degree of medical support. But I would still be careful with the wording. PRP does not create a new donor supply, does not turn a truly weak donor into a strong donor, and does not replace proper donor assessment or appropriate medical treatment, such as minoxidil, finasteride, or dutasteride, where appropriate. At most, it may help support the scalp’s biological environment in selected cases and may be part of a broader optimization strategy.
After surgery, PRP is often marketed as if it dramatically improves everything, but I think this topic should be discussed honestly. Some studies suggest PRP may help postoperative recovery and graft performance, but much of the attention is focused on the recipient area and early graft growth rather than on the donor area itself. For the donor area specifically, the evidence is much more limited than many clinics imply. So I would not present PRP as a proven solution that reliably makes the donor heal faster or better in every patient. I would present it more cautiously: it may possibly provide some supportive benefit in healing or inflammation control in selected cases, but it is not a substitute for careful extraction technique and proper donor management.
I also think it is important to explain that PRP is not the only treatment patients hear about. There are other add-on or “regenerative” treatments that are often marketed around donor recovery or scalp optimization. Low-level laser therapy, mesotherapy, exosomes, and other stem-cell-branded treatments are often discussed in this context. Some may have a limited supportive role in selected cases, but many are marketed far more aggressively than the evidence really justifies.
So my practical view is this: PRP and some other adjunctive treatments may have a supportive role in selected patients before or after surgery, but they should not be oversold. They do not replace good surgery. They do not replace a strong donor. And they do not correct poor donor management.
Why do many hair mill clinics push PRP, exosomes, and similar add-on treatments so aggressively?
In my opinion, this is something patients should understand very clearly. Many hair mill clinics attract patients with very cheap package prices, and that low headline price is part of the marketing strategy. The patient sees the package, compares only the initial number, and thinks he has found the same surgery for much less money.
But after the operation, or sometimes even just before it, these clinics often start pushing additional treatments such as PRP, exosomes, mesotherapy, laser sessions, stem-cell-branded cocktails, or various “growth booster” packages. These are often presented dramatically, almost as if they were mandatory, essential, or capable of transforming the outcome. In reality, they are often used not only as medical add-ons but also as a way to increase the total amount charged to the patient.
What makes this even more problematic is the type of clinic that most aggressively uses this strategy. In many hair mills, the surgery itself is already performed within a volume-driven system, where donor management, graft handling, and surgeon oversight may be compromised. Then, after a patient has already been drawn in by a cheap package, those same clinics may try to compensate by selling expensive adjunctive treatments with very inflated promises.
So the patient is first attracted by the low entry price, and later pressured into buying “supportive” treatments framed almost like rescue tools, mandatory upgrades, or miracle boosters. In my opinion, this is not how honest medical counseling should work.
My view is much simpler. Treatments like PRP may sometimes play a supportive role. Treatments like exosomes remain experimental and should not be marketed as established miracle solutions. None of these treatments can compensate for poor donor management, rushed extraction, high transection, or careless surgery. If the donor area has been properly assessed, harvested carefully, and managed intelligently, some supportive treatments may add a little in selected cases. But if the donor area has been handled badly, those add-ons will not undo the fundamental problem.
Is the donor area different in women?
Yes, it can be.
Female donor assessment often requires extra caution. In some women, the donor area is less clearly defined than in typical male-pattern hair loss, especially with more diffuse thinning. That means donor planning may need to be more conservative and more selective.
So while the basic idea of the donor area is the same, the evaluation is not always identical in men and women.
Does hairstyle matter when planning the donor area?
Yes, very much.
A patient who prefers to keep the hair very short may notice donor scarring, thinning, or unevenness more easily than a patient who keeps the donor area longer. This is one of the reasons why hairstyle preference matters when choosing between FUT and FUE, and also when deciding how conservatively or aggressively the donor should be harvested.
Good planning is not only about the surgery itself. It is also about how the donor area will look in the way the patient actually wears his or her hair.
Can smoking or poor healing affect the donor area?
Yes, they can.
Anything that negatively affects healing can also affect how the donor area recovers. Smoking is not friendly to surgical healing in general, and patients with poorer healing tendencies may experience more prolonged redness, irritation, or slower settling of the donor area.
That does not mean every smoker will have a bad donor result, of course. But in general, healthier healing habits are always better for surgical recovery.
Why do I personally consider the donor area one of the most important parts of hair transplant surgery?
Because the donor area is the foundation of everything else.
If the donor is strong, carefully assessed, and responsibly managed, it becomes possible to build a much better overall result. If the donor is misjudged, overused, or damaged, even a nice-looking front result becomes much less impressive.
A hair transplant should not only look good from the front. It should also leave the patient with a donor area that still looks natural and preserved. In my opinion, a surgeon who does not respect the donor is not thinking properly about the long-term welfare of the patient.
For me, good surgery is not just about what I implant today. It is also about what I preserve for tomorrow.
So, what is the simplest way to explain the donor area?
The donor area is the limited, valuable region of the scalp that provides grafts for a hair transplant. In FUE, individual grafts are extracted from this zone. In FUT, a strip of tissue is removed from it.
But whatever name is used for the technique, FUE FUT or DHI, the donor area remains the same in one very important sense: it is the patient’s reserve. It is not unlimited. It should be respected. And once it is used badly, it cannot simply be reset.
That is why, for me, the donor area is never just the back of the head. It is one of the most valuable parts of the entire surgery.