- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 29 Minutes
Is Your Receding Hairline Normal or Getting Worse?
A receding hairline means the front edge of the hairline is moving backward or becoming visibly weaker, usually first at the temples. In men, the most common reason is androgenetic alopecia, also called male pattern hair loss. But I want to be clear from the beginning. Not every high forehead, temple shape, or uneven front line is true balding.
A patient with a natural widow’s peak needs this distinction because the center may be stable while the temple corners are changing.
A mature hairline, stress shedding, traction from hairstyles, inflammation, thyroid disease, low iron, and some scarring conditions can all change the way the frontal hairline looks. A naturally high forehead is also different from a hairline that is actively moving backward.
Clinically, I first separate slow pattern recession from changes that need diagnosis. If the change is slow, symmetrical, and supported by family history, it is often pattern hair loss. If the change is sudden, patchy, painful, itchy, red, scaly, or associated with heavy shedding, it needs diagnosis before anyone talks about graft numbers.
In short, a receding hairline should first be diagnosed before treatment is chosen. If the recession is early and active, medication or monitoring may be the first step. If the temples are clearly lost and the donor area is strong enough, a hair transplant may rebuild the hairline. But the safest result depends on age, future hair loss risk, donor capacity, and natural hairline design.
Many patients are not told this clearly enough. A receding hairline is not only a missing corner. It is a forecasting problem. It tells me something about what may happen behind the hairline later. If the crown is beginning to thin, if the mid-scalp is weaker than it looks, or if the donor area is limited, the hairline plan must change.
Before I talk about treatment, I want to understand whether the hairline is truly changing, why it is changing, and which treatment would still make sense if we look at the same patient five or ten years later.
What Should You Do First If Your Hairline Is Receding?
If you think your hairline is receding, the first step is not choosing a clinic or asking for a graft number. The first step is understanding whether the hairline is truly moving, why it is moving, and whether the surrounding hair is also becoming weaker.
I want to know the patient’s age, family history, speed of change, old photos, crown condition, mid-scalp density, donor quality, and whether there are symptoms such as itching, burning, redness, scaling, or sudden shedding.
A close-up temple photo can show the visible concern, but it cannot show the whole risk. A single close-up image is too narrow for safe hairline planning. A proper plan needs the front, temples, crown, donor area, hair caliber, age, family pattern, and speed of progression.
Consultations that begin with a package number are a warning sign for me. A real plan should begin with the cause of the recession, the strength of the donor area, future risk, and a design that would still look natural as the patient gets older.
When Should You Watch, Treat, or Consider Surgery?
Most patients want to know whether they should watch the hairline, treat it medically, or consider surgery. In real consultations, I separate receding hairline patients into four practical groups.

When the change is mild, the hairline edge is still strong, old photos look stable, the crown is not thinning, and there are no scalp symptoms, watching and photographing the hairline can be reasonable. Daily mirror checking usually creates noise. Consistent monthly photos, taken in the same conditions, are more useful than panic.
When the hairline change is sudden, patchy, painful, itchy, red, scaly, shiny, or associated with eyebrow thinning, heavy shedding, or female frontal recession, diagnosis should come first. These signs can point away from simple male pattern hair loss.
When miniaturized hairs are still present, the patient is young, the recession is actively changing, or the family history suggests more advanced future hair loss, stabilization may be the better first step. Treatment should protect the hair behind the hairline, not only improve the front edge today.
Hairline transplant planning becomes more reasonable when the temple loss is clear, the pattern is stable enough, the donor area is strong enough, there is no active scalp disease, and the patient accepts a natural adult hairline rather than the lowest possible line.
This framework is not a replacement for examination, but it helps patients think more clearly. A receding hairline should not immediately lead to surgery. It should lead to the correct category of decision.
Why Is a Receding Hairline a Forecasting Problem?
A receding hairline is not only about the corners today. It also tells me something about what may happen behind the hairline later.
When I assess a patient, I am not only asking whether I can close the temples. I am asking whether the crown is beginning to weaken, whether the mid-scalp is quietly thinning, whether the donor area can support future needs, and whether the proposed hairline will still look natural as the patient gets older.
A low hairline drawing can be misleading. On paper, it may look exciting. In real life, it uses permanent donor grafts. If the patient later develops crown thinning or mid-scalp loss, those grafts are no longer available for the next problem.
The safest hairline is not the lowest one. It is the one that still makes sense when the whole pattern is considered.
Can a Receding Hairline Grow Back?
Sometimes, yes. But it depends on why the hairline looks weaker.
If the difficulty is stress shedding, recent illness, rapid weight loss, traction, inflammation, or a correctable deficiency, some improvement may be possible once the trigger is controlled. If the difficulty is androgenetic alopecia and the temples have been empty for a long time, medication may protect weaker hairs, but it usually cannot recreate a full new hairline shape by itself.
That distinction matters because weak hair and lost hair do not behave the same way. Weak miniaturized hair may still respond. A bare temple that has been empty for years usually needs surgical restoration if the patient wants to rebuild the shape.
Patients sometimes lose valuable time because they hope a shampoo, oil, vitamin, or temporary treatment will bring back a hairline that has already disappeared. I understand why that hope is attractive, but it should not replace a realistic diagnosis and treatment plan. The earlier the correct diagnosis is made, the more options we usually have.
How Do You Treat a Receding Hairline?
Treatment depends on whether the hairline is actively thinning, already lost, or not truly receding. Medication can protect and thicken existing miniaturized hair, but it cannot reliably rebuild a completely empty temple. A hair transplant can rebuild shape, but it does not stop future loss. Most good plans use this distinction carefully.
I think about treatment in three steps. First, diagnose and remove any correctable cause. Second, stabilize existing hair if the pattern is active. Third, consider surgical restoration only when the lost shape cannot realistically return with medical treatment alone.
Can Minoxidil Help a Receding Hairline?
Minoxidil can help some patients slow shedding, thicken miniaturized hairs, and improve overall density. It is often more predictable in the crown than in completely bare temples, but it can still be useful when the hairline has weak hairs that are not fully lost.
In the first few weeks, I mainly look at tolerance, irritation, and whether you can use minoxidil consistently. A fair assessment of benefit needs several months, and often closer to 6 to 12 months. Early shedding can happen, irritation can happen, and the benefit is usually maintained only while treatment continues.
Minoxidil is not a hairline drawing tool. It does not create a new shape where the temples have been empty for a long time. Its best role is usually protecting and improving hairs that are still alive but weaker than before.
If you are considering minoxidil around surgery, the timing needs planning carefully. This point is part of minoxidil after hair transplant. If you are considering oral minoxidil rather than topical minoxidil, that decision should be more careful; oral minoxidil and hair transplant planning needs the same judgment.
Should You Use Finasteride or Dutasteride?
Finasteride and dutasteride reduce DHT activity and can be very useful for many men with pattern hair loss. They are not cosmetic vitamins. They are medications, and the decision should include benefits, side effects, age, fertility plans, medical history, and personal comfort with long-term use.
For some patients, medication is the main treatment. For others, it is used to protect native hair before or after surgery. A patient who wants a hair transplant but is still losing hair quickly needs a serious conversation about stabilization, because transplanted hair may survive while the surrounding native hair continues to thin.
If you are trying to understand the medication side of planning, the pages about hair transplant without finasteride, finasteride before and after hair transplant, and dutasteride vs finasteride go deeper into those decisions.
I also explain that not every patient can or wants to use these medicines. That does not by itself make surgery impossible, but it changes the risk discussion. If future hair loss is likely and no medical maintenance is used, the hairline must be planned even more carefully.
Do PRP, Laser, or Shampoos Fix a Receding Hairline?
PRP and low-level laser therapy may help specific cases with hair quality or density, especially when some miniaturized hair remains. They should not be sold as a guaranteed way to rebuild empty temples. Shampoos can help scalp inflammation, dandruff, or irritation, but they do not redesign a lost hairline.
These treatments are sometimes useful as support. They are not substitutes for diagnosis, medication when appropriate, or surgical planning when the hairline has already been lost.
When Is a Hair Transplant the Right Choice?
A hair transplant becomes more reasonable when recession is clearly visible, the cause is understood, the donor area is strong enough, and the patient wants a long-term hairline rather than the lowest possible hairline. I am not trying to erase every sign of age. I want to restore facial framing in a way that looks natural and still fits the patient as he gets older.
For a receding hairline, I pay close attention to the frontal hairline, temple corners, temple points, hair caliber, graft direction, and density transition. A natural hairline is not a wall of equal grafts. It needs softness at the front, irregularity in the right places, and single hair grafts placed with careful angle and direction.
Hairline design controls much of the operation. The drawing must respect the face, the donor area, and the likely future pattern. A low and flat hairline can look artificial even when the growth is technically good, and it can create problems if the crown or mid-scalp thins later.
What Is the Real Difference Between a Mature Hairline and a Receding Hairline?
A mature hairline usually settles. A receding hairline keeps changing.
With a mature hairline, the front may sit slightly higher than it did at seventeen or eighteen, but the edge still looks strong. The corners do not keep moving backward every year, and older photos show only a mild adult change.
With a receding hairline, I usually see progression. The temples open more, the front edge becomes weaker, and there are often thin, short, miniaturized hairs at the border. The detail that matters is not only where the hairline sits today. It is whether the hairline is still moving.
I do not decide this from one photograph. I compare age, family history, crown density, temple point strength, miniaturization, and the speed of change. A 22-year-old with active thinning at the temples is different from a 38-year-old whose hairline has looked the same for years.
This distinction matters because treating a normal mature hairline too aggressively can create an unnatural low and flat result. On the other side, ignoring true early recession can allow preventable loss to continue for years.
A common mistake is chasing the teenage hairline. A teenage hairline can look strange on an adult face, especially if the temple points, forehead shape, and future crown thinning are not considered. A mature but well framed hairline often looks stronger and more natural than an artificially low one.
What Does a Receding Hairline Look Like?
A receding hairline usually starts with temple recession. The corners move back, the front edge becomes less dense, and the hairline may begin to form an M shape. Some people notice the change only when the hair is wet, under strong bathroom light, or in photos taken from above.
The detail I look for is not only bare skin. I look for weaker, thinner, shorter hairs at the edge of the hairline. These miniaturized hairs can show that the hairline is still changing, even before the recession looks dramatic.
One useful habit is to take the same photo once a month. Use the same lighting, the same angle, dry hair, and hair gently pushed back. A single bad selfie can make almost anyone anxious. A six-month photo comparison tells a much clearer story.
One temple can also change before the other. That asymmetry can be part of early pattern recession, but it can also be exaggerated by lighting, hairstyle, pillow direction, or the way the hair is pulled back. I look for progression and miniaturized hairs around the edge, not only whether the two corners look perfectly equal in one photo.
If only one corner bothers you, I still design the whole hairline in my mind before considering grafts. Treating one side without understanding the other side can create a line that looks corrected in the mirror but unbalanced in real life. Sometimes the safer answer is monitoring. Sometimes both corners need subtle planning. Sometimes one side can be refined, but it should still belong to the whole face, not to one panic photo.

In men, the pattern often begins at the temples and may later involve the mid-scalp or crown. In women, the front hairline is often preserved in typical female pattern hair loss, so a clearly receding frontal line needs a careful look. Traction, frontal fibrosing alopecia, inflammation, and hormonal or medical triggers can all change the front hairline in different ways.
Hairline recession can also be misleading because styling changes the way it looks. Longer hair pushed forward can hide weak corners. Wet hair, short hair, harsh light, or a pulled back hairstyle can reveal recession that was already there. I prefer realistic photos over emotional guessing, because the treatment decision should be made from the pattern, not from a frightening moment in the mirror.
When Should You Get Checked?
You should be checked if the recession is changing quickly, if there is itching, burning, scaling, redness, eyebrow thinning, patchy loss, or sudden heavy shedding. These details can point away from simple pattern hair loss. In those cases, the right answer may be a dermatology diagnosis, blood work, scalp treatment, or medical stabilization before surgery is considered.
I am especially cautious when the hairline loss is not behaving like ordinary male pattern hair loss. Conditions such as traction alopecia, alopecia areata, frontal fibrosing alopecia, thyroid related shedding, and low ferritin can all affect the front hairline. Some can improve when treated early. Some can scar and become permanent if missed.
A transplant should not be used to hide an unclear diagnosis. If the scalp is inflamed, unstable, or affected by an active scarring process, placing grafts into that area may give poor growth and may make the situation more difficult.
Is a Receding Hairline Different in Women?
Yes. In women, I am more cautious about calling frontal recession simple pattern hair loss. Female pattern hair loss often appears as diffuse thinning or a widening part. True frontal recession can suggest traction, frontal fibrosing alopecia, inflammation, hormonal change, or another diagnosis.
Eyebrow thinning, shiny skin at the hairline, itching, burning, redness, scaling, pain, or a hairline that seems to move back in a band-like pattern should not be ignored. These details can change the entire treatment plan.
Some female patients come with a very reasonable wish. They want the front line restored because the face no longer feels framed. I understand that. But if the follicles are unstable or the diagnosis is uncertain, surgery may not be the safest first step.
I pay close attention to transplant planning for women when the diagnosis is unclear. The first priority is to understand whether the follicles are stable enough to support surgery. Only after that can we discuss whether restoration is safe, natural, and worth doing.
When Is a Receding Hairline Not a Simple Hair Transplant Case?
If the scalp is red, painful, itchy, shiny, scaly, or the eyebrows are thinning, I do not treat this as a normal hairline transplant case. First, I want to understand whether there is inflammation or scarring alopecia.
A transplant into an unstable scalp can grow poorly, and in some cases the real problem continues after surgery. That matters most in frontal hairline problems that do not follow a typical male pattern.
Patients sometimes think the solution is simply to place grafts into the empty area. But if the underlying disease is still active, the new grafts may be placed into a scalp that is not ready to support them. That skips diagnosis instead of practicing careful surgery.
In doubtful cases, the safer path is to identify and control the underlying condition first. Surgery can be discussed later only if the scalp becomes stable and the expected growth is realistic.
What Photos Help Diagnose a Receding Hairline?
The best photos are not the most flattering photos. They are the most consistent ones. I like to see the hair dry, brushed back, photographed from the front, both temples, top, crown, and donor area. If possible, old photos from two, five, and ten years earlier are very useful.
Many patients send only a close-up of the temples. That helps, but it can mislead the decision if the crown or mid-scalp is also thinning. I need to see the whole pattern, because a hairline transplant planned without the rest of the scalp can become a poor long-term decision.
Wet hair photos can also be useful, not because the patient normally walks around like that, but because wet hair reveals density and miniaturization more. Strong light is uncomfortable, but it shows what the result must survive in real life.
When patients send photos for consultation, I prefer simple photos rather than edited or filtered images. The hair should not be covered with fibers, styling powder, concealer, or strong product. A good plan depends on seeing the real condition. I explain this limitation more deeply in my article on whether a hair transplant plan can be trusted from photos alone.
What Causes a Receding Hairline?
The most common cause is genetic pattern hair loss. Genetically sensitive follicles respond to androgens over time by producing thinner, shorter hairs. The hairline can look less solid before the area becomes completely empty.
Family history helps, but it is not perfect. Some men follow their father’s pattern, some follow the mother’s side, and some do not match either side neatly. I use family history as one clue, not as the whole diagnosis.
Can Stress or Illness Make the Hairline Look Worse?
Stress, fever, surgery, rapid weight loss, and major illness can trigger shedding. This is often called telogen effluvium. It usually affects the scalp more diffusely, but if the frontal hairline is already weak, the shedding can make recession look suddenly worse.
Timing matters because hair that sheds after a trigger may recover, while hair miniaturized by pattern hair loss usually needs a different plan.
What If the Hairline Is Receding Because of Traction?
If the hairline is being pulled every day, surgery is not the first answer. The first answer is to stop the repeated stress on the follicles. Tight hairstyles, extensions, repeated pulling, harsh chemical treatment, and heat can slowly damage the front and temples.
When I suspect traction, I first want to remove the ongoing force from the hairline. If the same habit continues after surgery, the transplanted area is being asked to survive in the same environment that damaged the original hair.
In early traction, the hairline may improve when the cause is removed. In long-standing traction, the loss can become permanent and may need surgical planning later. That surgical question is part of traction alopecia hair transplant.
Can Medical Problems or Deficiencies Affect the Hairline?
They can. Thyroid disease, low iron or ferritin, inflammatory scalp disease, some medications, and hormonal changes can contribute to hair loss. A full blood panel is not always necessary for every patient. The history and scalp findings should guide the workup.
For example, if a patient has heavy shedding, fatigue, menstrual changes, thyroid symptoms, or sudden diffuse thinning, the plan should not jump straight to hair transplant surgery. The underlying reason needs to be understood first.
Why Does Diagnosis Come Before Graft Numbers?
Because the same visible hairline can have different causes. A stable mature hairline, active male pattern hair loss, traction alopecia, and scarring alopecia should not be treated with the same plan. The wrong diagnosis can lead to wasted grafts, poor growth, or a hairline that looks worse as the surrounding hair continues to thin.
Consultations that begin and end with a graft quote leave too much unanswered. The hairline is only one part of the decision. The donor area, crown, mid-scalp, medication tolerance, age, family pattern, and future hair loss risk all matter.
What Should a Good Hairline Assessment Include?
A good assessment should look at the whole head, not only the first centimeter of the hairline. I want to see the donor area, crown, mid-scalp, frontal density, temple points, scalp skin, hair caliber, and older photos if the patient has them. I also have to understand how fast the change has happened.
A consultation should answer whether this is true hair loss or a naturally high or mature hairline, whether the loss is stable or active, and whether the donor area can support the design without creating problems later if surgery is considered.
When these questions are skipped, the plan often becomes too simple. The patient is told a graft number, a low line is drawn, and nobody explains what happens if the crown thins in five years. I prefer to have that conversation before surgery, not after the donor area has already been used.
I assess the emotional pressure around the decision. Some patients are ready and realistic. Some are panicking after a haircut, a harsh photo, or a comment from someone else. A decision made during panic can lead to hair transplant regret after surgery, even if the technical work is acceptable. The decision should feel clear, not rushed.
Can Lifestyle Stop a Receding Hairline?
Lifestyle can support scalp and general health, but it usually does not reverse genetic pattern hair loss by itself. Good sleep, enough protein, correction of deficiency, stopping harsh traction, treating dandruff or inflammation, and avoiding smoking are all sensible. They are not the same as treating androgen sensitivity when that is the main cause.
Patients can lose time here. They try shampoos, oils, supplements, and scalp massages for years while the hairline quietly miniaturizes. If there is a deficiency or scalp disease, treat it. If there is pattern hair loss, be clear about that too.
I do not dismiss lifestyle, but I do not let it replace real treatment. If a patient has low ferritin, uncontrolled thyroid disease, severe dandruff, or traction from tight hairstyles, those should be addressed. If the pattern is clearly androgenetic, lifestyle alone is usually not enough to hold the hairline.
What Are the Stages of a Receding Hairline?
People often use stages because they want a clear label. In real life, recession is more of a spectrum. Some patients only have temple recession. Some have front and crown thinning together. Some have a naturally high hairline that has not truly changed.
The Norwood scale can be useful for male pattern hair loss, but it should not replace clinical judgment. I use it as a map, not as a treatment plan.
What Is Early Recession?
Early recession usually means mild temple movement, a slightly weaker front edge, or the first signs of miniaturized hair. At this stage, medication, monitoring, and good diagnosis can make the biggest difference. A transplant may be too early if the pattern is still unclear or the hairline is only minimally changed.
In this stage, I prefer not to rush. Sometimes the correct plan is photo tracking, scalp examination, medication discussion, and reassessment. That may feel slower, but it protects the patient from an operation that may not yet be needed.
What Is Moderate Recession?
Moderate recession is easier to see. The temples are more open, the M shape is clearer, and styling may become harder. At this point I look closely at the crown and mid-scalp, because a patient who only worries about the hairline may miss thinning behind it.
At this stage, hairline design becomes very important. A mature, slightly conservative hairline can look natural for decades. A very low, straight line may look tempting in a drawing, but it can age badly and consume too much donor hair.
Moderate recession is also the stage where many patients become vulnerable to overpromising. They are not bald, so the donor area looks strong, and a clinic can make a low hairline drawing look exciting. What may be missing is whether that same design will still make sense if the mid-scalp or crown continues to thin.
What Is Advanced Recession?
Advanced recession may involve the front, temples, mid-scalp, and crown. Planning moves beyond simply rebuilding the hairline. It becomes a question of how to distribute a limited donor supply so the result still makes sense from the front, top, sides, and future.
In advanced cases, I usually explain the donor area very directly. There may be enough donor hair to improve framing and frontal density, but not enough to restore every thin area at teenage density. Clear planning is much better than an impressive graft number that the donor area cannot safely support.
How Do I Read the Norwood Scale?
Norwood 1 and Norwood 2 patterns can be normal or early. Norwood 3 usually means more definite recession. Higher Norwood patterns often include broader front, mid-scalp, and crown involvement. Still, the number alone does not decide treatment.
A Norwood 3 patient with strong donor hair, stable loss, and realistic expectations may be a good candidate. A younger patient with diffuse thinning and rapid progression may need stabilization first, even if the visible recession looks smaller.
The Norwood scale does not show donor quality, hair caliber, scalp contrast, miniaturization, medical tolerance, or emotional readiness. Those details often matter more than the label.

Who Should Wait Before Hairline Surgery?
Some patients are better served by waiting. This includes patients with very early or uncertain recession, rapid ongoing loss, diffuse thinning behind the hairline, unstable medical causes, active scalp inflammation, weak donor area, or expectations that no surgery can satisfy safely.
Waiting does not mean doing nothing. It may mean tracking the pattern, treating inflammation, correcting a deficiency, using medication if appropriate, and reassessing with better information. Surgery is strongest when the diagnosis and long-term plan are clear.
I know waiting can be frustrating, especially when the hairline is the first thing a patient sees in every photo. But sometimes waiting 6 to 12 months gives a much safer answer. It can show whether medication is helping, whether shedding recovers, and whether the recession is truly progressing.
There is also an emotional side. If the decision is driven by panic, comparison, or pressure after seeing aggressive transformations online, more time is often the safer choice. A hair transplant should be a clear decision, not a reaction to anxiety.
How Does Age Change the Hairline Plan?
Age changes the risk. A patient in the early twenties with temple recession may still be at the beginning of a much larger pattern. If I rebuild a low hairline too early and the crown later opens, the patient can be left with an isolated front and not enough donor reserve to manage the rest well.
What If You Are in Your Twenties?
In the twenties, I am cautious. My conclusion is not that every young patient is refused. It means the diagnosis, family history, donor area, medication plan, and expectations must be taken seriously. If the loss is active and the future pattern is unclear, monitoring and medical treatment may be safer than surgery.
In young patients, the weaker point is not only doing surgery too early. The bigger mistake is designing the hairline as if the final hair loss pattern is already known. At 22 or 24, the front may be the only visible problem, while the crown and mid-scalp may declare themselves later. I prefer a plan that can survive future thinning, not a plan that only looks exciting on the day of the drawing.
What If You Are in Your Thirties?
In the thirties, the pattern is often clearer. A transplant may be more reasonable if recession is stable enough and the donor area is good. But I still do not design a hairline as if the patient will never lose more hair. The crown and mid-scalp must be checked carefully.
Many patients in this age group are good candidates, but the plan still has to be realistic. A natural adult hairline usually ages better than an aggressive one.
What If You Are Over Forty?
After forty, the pattern is often easier to read, but donor management still matters. Some patients have strong donor hair and mainly frontal recession. Others have wider thinning and need a more conservative plan. A good design frames the face naturally without pretending the donor area is unlimited.
How Does the Plan Change in Real Patients?
Two patients can have similar looking temples and need very different plans.
A 22-year-old with active temple recession, miniaturized hairs behind the hairline, and a strong family history of advanced baldness should not be treated like a finished pattern. In this patient, I usually think first about diagnosis, stabilization, and time. If surgery is done too aggressively, the result may look good for a short period and then become difficult to manage as the surrounding hair continues to thin.
A 38-year-old with stable temple recession, strong donor hair, no major crown thinning, and realistic expectations may be a very different case. If the hairline design is mature and the graft number is calculated carefully, hairline restoration may be more reasonable.
I do not believe in one hairline formula. The correct plan depends on the patient in front of me, not only the shape of the corners.
Should You Treat the Hairline or Crown First?
This depends on what bothers the patient and what the donor area can support. The hairline usually gives the biggest visual change because it frames the face. The crown can require many grafts and still look less dense because of the spiral pattern and wider surface area.
When both the hairline and crown are involved, I discuss the tradeoff before choosing the surgery order. Some patients should prioritize the front first. Some should wait until the pattern is more stable. Some need a staged plan. Whether to treat the hairline or crown first is a donor supply decision, not just a cosmetic preference.
The risky decision is trying to solve everything in one session when the donor area cannot truly support it. That can make the result look thin everywhere. A focused frontal plan may create a stronger visible change than spreading grafts too widely.
How Many Grafts Does a Receding Hairline Usually Need?
Patients often ask for one number, but a receding hairline does not have one fixed graft count. A small temple corner correction may be around 1,000 to 1,800 grafts. A moderate frontal hairline reconstruction may be around 1,800 to 2,500 grafts. A larger frontal third restoration may require 2,500 to 3,500 grafts or more.
These numbers are not promises. They are only a practical way to understand scale. In my planning, I first decide whether the proposed hairline belongs to the face and whether the donor area can safely support it. Only after that do I calculate the graft number.
The opposite approach is risky. A clinic chooses an impressive number first, lowers the hairline too much, and then spends donor hair without thinking about the next ten or twenty years. For a receding hairline, the right number is the number that supports a natural design without damaging the future plan.
Why Does the Transition Zone Matter in Hairline Design?
The front edge should not look like a wall. In natural hairlines, there is a soft transition before the denser hair begins. I use finer single hair grafts at the very front and avoid placing the same density and thickness everywhere.
A hairline that is too equal can look artificial even if many grafts grow. The eye catches regularity, rows, and thick grafts at the very front. The patient may not know exactly why the result looks wrong, but he feels that the hairline does not belong to the face.
A natural result depends on design, graft selection, density transition, direction, angle, and incision distribution. A good hairline cannot be judged only by the number of grafts used. This point is part of what makes a good hair transplant result.
Why Does Donor Management Matter?
The donor area is limited. Once grafts are removed, they are no longer available for future surgery. I do not plan a hairline as if the patient has unlimited donor supply.
In a young patient with early recession, the better answer may be to wait, stabilize, or choose a modest design. In a patient with advanced loss, the better answer may be to prioritize the front and accept that crown coverage has limits. Good donor management is how a result stays natural over time.
Overharvesting the donor area to chase density at the front can create a second problem. The front may look better for a while, but the back and sides can look thinned, patchy, or depleted. A good hairline result should not come at the cost of an obviously damaged donor area.
If a donor area is weak, the responsible answer may be a smaller plan, a staged plan, or no surgery. For weak donor area and hair transplant, donor quality can change the entire treatment strategy.
What About Temple Points and a Low Hairline?
The temple points can change how the whole hairline is read. If the front hairline is lowered too much while the temple points remain weak or receded, the result can look disconnected. In other patients, rebuilding the temple points too aggressively can look sharp, artificial, or too youthful for the face.
I plan the front hairline and temples together. Temple point hair transplant is part of that balance, and low and flat hairlines show why a lower line is not necessarily a better line.
Some patients want the corners closed completely because they believe that any visible temple recession is a defect. I do not agree with that approach. A slight adult recession can look natural. A forced square frame can look operated.
What Makes a Hairline Transplant Look Unnatural?
An unnatural hairline is usually not caused by one single mistake. It can come from a line that is too low, too straight, too dense at the very front, too regular, or placed with the wrong angles. It can also happen when thick multi hair grafts are used at the front edge instead of fine single hair grafts.
The result has to survive real life. It should look natural when the hair is wet, when the patient is under bright light, when the hair is short, and when the patient ages. Small design decisions matter because patients live with the result in ordinary light, not only in after photos.
Repairing a bad hairline is harder than doing it correctly the first time. A pluggy or overly straight front may need graft removal, redistribution, camouflage, or staged repair. That costs time, donor hair, and emotional energy. The better decision is to avoid the mistake at the first surgery.
A thin looking result can also come from poor planning even when a large number of grafts was used. If the design is too wide, the density is spread too thin, the donor is overused, or the hairline is lowered beyond what the donor can support, the patient may end up with a result that is technically grown but visually disappointing. The same problem from the density side belongs in why some hair transplant results look thin.
Which Technique Is Best for a Receding Hairline?
Technique matters, but it should not be used as a marketing shortcut. FUE and DHI are methods of handling and placing follicular units. Neither automatically guarantees a natural hairline. The design, graft selection, recipient area incisions, density planning, and surgical judgment matter more than the label.
For the front edge, I want fine single hair grafts, natural direction, careful angle, and a soft transition. The clinic page comparing DHI and FUE explains the technique difference, but you should not choose a clinic only because one method sounds more modern.
Modern FUE hair transplant can be an excellent method for frontal restoration when the diagnosis, donor management, extraction pattern, and recipient area planning are done properly. At Diamond Hair Clinic, I use Sapphire FUE because I value controlled recipient area incision creation, natural angle, and careful distribution. But the blade or method is not a magic answer. The surgical judgment behind it matters more than the label.
How Much Does Treating a Receding Hairline Cost?
Cost depends on the diagnosis and the plan. Early medical treatment is different from a transplant. A small temple refinement is different from rebuilding a full frontal third. What concerns me is choosing graft numbers from a package before the hairline has been designed properly.
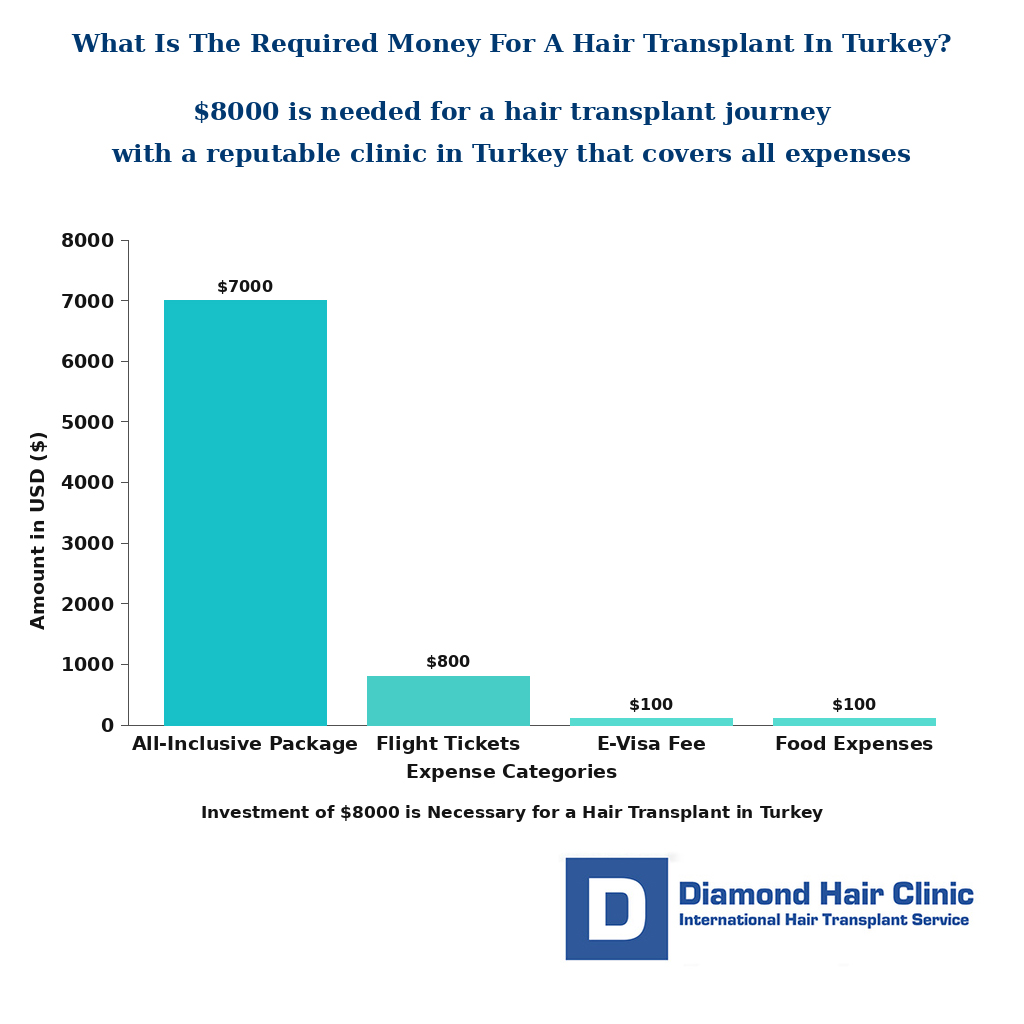
For surgery, graft number should follow the design, not the other way around. A careful 1,800 graft hairline can be much better than a careless 3,500 graft promise. The right number depends on the size of the recipient area, hair caliber, donor strength, density goal, and how much reserve must be protected for the future.
Package-style graft promises concern me for this reason. A large number may sound attractive, but if the hairline is too low, too dense in the wrong place, or planned without future loss in mind, the patient may pay later with donor depletion or repair surgery.
If you are comparing clinics in Turkey, hair transplant cost in Turkey needs judgment together with surgeon involvement, donor management, and the real quality of planning.
What Happens If You Do Nothing?
Doing nothing may be reasonable if the hairline is mature, stable, and not bothering the patient. It may be risky if the hairline is actively miniaturizing and the patient wants to preserve as much native hair as possible. The pattern decides how much waiting costs.
If it is genetic pattern hair loss and no treatment is used, progression may continue. The speed is different for each patient. Some lose slowly over decades. Some change quickly in a few years. Photo tracking and follow-up matter because the pattern becomes clearer over time.
I do not push treatment on every patient. The point is to understand what waiting means in that specific case. Waiting with a plan is different from ignoring the problem because the decision feels uncomfortable.
What Questions Should You Ask Before Treatment?
Before medication, ask what the expected benefit is, how long it takes to judge, what side effects matter, and what happens if you stop. Before surgery, ask why the proposed hairline height is right for your face, how the donor area was assessed, what happens if future hair loss continues, and whether the clinic is planning only the front or the whole scalp.
After a proper consultation, you should feel clearer, not only excited, and understand the reason behind the plan. If the only explanation is a large graft number or a discounted package, the conversation is incomplete.
I warn patients about red flags of hair mills for exactly this reason. A low price, a large graft number, and a very low hairline drawing can feel convincing at the beginning. But the detail that matters is whether the plan protects the donor area and still looks natural in the future.
If you are not sure whether you are a safe surgical candidate yet, whether you are really a good candidate for a hair transplant can help you think through the decision more carefully.
What Is My Approach at Diamond Hair Clinic?
At Diamond Hair Clinic, I do not look at a receding hairline as an isolated line on the forehead. I look at the whole scalp, the donor area, the crown, the mid-scalp, the temple points, the patient’s age, family history, and long-term risk.
Some patients are good candidates for hairline restoration. Some need medication or monitoring first. Some should not have surgery yet. I prefer to say this clearly before surgery, because a hairline transplant uses permanent donor hair and the decision cannot be treated casually.
If surgery is the right choice, I am not trying to create the lowest possible hairline. The better goal is a hairline that frames the face naturally, uses grafts intelligently, and still makes sense as the patient gets older.
The one patient per day model matters here because rebuilding a receding hairline may look like a small operation from outside, but the design controls the whole result. The angle, direction, density transition, temple balance, and donor planning all decide whether the patient looks natural or operated on.
A good hairline should belong to the patient’s face and protect his future options.
If you are unsure whether your hairline is maturing, receding, or ready for treatment, you can contact Diamond Hair Clinic and share clear photos. A proper consultation is not just about whether a transplant is possible. It is about whether it is the right decision for your hairline now and for the years ahead.


