- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 15 Minutes
Alopecia Areata and Hair Transplant Surgery: Why Stability Matters
For active alopecia areata, a hair transplant usually comes after diagnosis, treatment, and stability, not before them. If the hair loss is autoimmune hair loss, patchy, unpredictable, or still changing, medical control should come before surgery is even considered. A transplant moves hair. It does not switch off the immune process that caused the patchy loss in the first place.
If alopecia areata is active, unstable, or affecting the donor area, surgery is usually unwise. If the disease has been quiet for a long time and the patient also has a separate pattern of male hair loss, surgery may sometimes be discussed very carefully. The distinction between these two situations is everything. Vitiligo hair transplant planning is different, because the hair loss may be male pattern thinning while the skin stability still changes the timing.
Why is it different from male pattern hair loss?
The condition is different because the hair loss is not mainly about the usual male pattern thinning process. It is immune-related, and hair can disappear in patches and sometimes return. Male pattern hair loss behaves differently. It usually follows a more predictable pattern in the hairline, mid-scalp, and crown.
This difference matters because hair transplant surgery works best when the diagnosis is stable and the donor hair is reliable. In male pattern hair loss, the donor area is usually more resistant to the same thinning process. With immune-related patchy loss, different areas can be affected unpredictably. It may affect the recipient area. It may affect the donor area. It may also return after a quiet period.
It is one reason I avoid deciding from photos alone. A round patch, sudden shedding, side thinning, or unusual pattern may look simple in a picture, but the diagnosis may be more complicated. A separate history of hair pulling related hair loss needs a different assessment from alopecia areata. Planning a hair transplant from photos can start a conversation, but it should not finish a diagnosis.
When the diagnosis is wrong, the surgical plan becomes wrong. A patient who needs medical treatment may be sold grafts. A patient who needs time may be rushed into surgery. That is how preventable regret begins.
Patchy autoimmune hair loss can change the emotional meaning of the problem. Male pattern hair loss often feels gradual. This condition can feel sudden and unfair. A patch appears, then the patient studies the mirror every day. That emotional shock can make surgery feel like the only decisive answer, even when the disease itself has not been understood.
In surgical planning, urgency created by fear is not enough. I need the diagnosis to make sense, the pattern to make sense, and the donor area to make sense. If those pieces are unclear, the clear answer is evaluation first, not graft numbers first. I apply similar logic in PCOS hair transplant planning, because the label alone does not prove that surgery is ready.
When is surgery usually a poor idea?
Surgery is usually a poor idea when the condition is active or still poorly diagnosed. Spreading patches, donor involvement, repeated inflammation, and a clinic treating it like ordinary male pattern hair loss all make me slow down. The disease behavior matters more than the patient’s wish to fill the area quickly.
The concern is not only that the transplanted hairs may fail. The deeper issue is that the disease process may later affect the transplanted area or the donor area. A technically clean surgery can still be a poor decision if the biology is unstable.
Emotional urgency also changes the consultation. Patchy hair loss can be very distressing. It can make a patient feel exposed, embarrassed, and impatient for a permanent solution. I understand that. But surgery is not always the right answer to emotional urgency.
A patient with an active immune patch is often better served by proper diagnosis, dermatology treatment, and observation before surgery. This is part of why being a good candidate for a hair transplant requires more than wanting the empty spot filled.
Rapid improvement also needs careful interpretation. Regrowth is encouraging, but it does not always mean the condition will never return. I check how long the area has been stable, whether the patient needed treatment to maintain it, and whether new areas have appeared elsewhere.
Another poor reason for surgery is embarrassment alone. I do not dismiss embarrassment. It is real. But if surgery is used to hide active disease without treating the disease, the patient may spend money and donor grafts while the underlying condition remains capable of changing the result.
Can surgery ever be considered after it becomes stable?
In selected cases, surgery may be discussed after the disease has been quiet for a long time, the diagnosis is clear, the donor area is healthy, and the surgical goal is realistic. I use the word discussed deliberately. I do not say automatically approved.
The surgeon must understand what area is being transplanted and why. A small old patch that has been quiet for years is very different from a moving immune condition. A stable male pattern hairline problem is also different from immune-related loss affecting the same area. The risk changes with the story, not only with the size of the empty space.
It helps to name the uncertainty clearly. Even if the disease has been quiet, it can still be unpredictable. No ethical surgeon should guarantee that the immune process will never return. The patient must know that a transplant cannot remove that uncertainty.
If surgery is considered, the plan should be conservative. The goal should be natural improvement, not dramatic overcorrection. A careful plan protects the donor area in case future decisions are needed.
Documentation also matters. Good photographs from different periods, dermatology notes if available, and a clear timeline can be very helpful. If the patient says the condition has been quiet for years, I need to understand what quiet really means. No patches at all. Occasional tiny spots. A large flare that recovered. These differences matter.
The patient also needs to accept that even a stable history does not create a perfect prediction. A surgeon can reduce risk by choosing the right patient and timing, but no surgeon can promise that the disease will obey the surgical plan forever. Clear consent has to include that uncertainty.
How long should the condition be quiet before surgery is discussed?
I do not use one universal number for every patient, because the pattern matters. A tiny patch that appeared once many years ago and fully regrew is not the same as repeated patches over the last year. Still, I do not consider a few quiet weeks or one reassuring photo to be enough. For me, quiet means no new patches, no enlargement of old patches, no recent donor-area involvement, and a pattern that stays stable rather than changing every few weeks. The disease can look settled before it becomes active again.
If the plan is to transplant into an old immune patch, I need more evidence than one quiet interval. I usually want a long period without activity, clear photographs over time, and dermatology input if there is any doubt. In some cases, several years of stability may still not remove the uncertainty completely.
If the patient is not asking to fill an immune patch, but has separate male pattern hair loss, the conversation is different. Even then, I still want to know whether patchy loss has recently appeared anywhere on the scalp or body. A quiet history is reassuring only when it is truly quiet.

What if I also have male pattern hair loss?
I separate this situation very carefully. A patient can still have patchy autoimmune loss and male pattern hair loss at the same time. The round patch may be immune-related, while the hairline or crown may be thinning from androgenetic hair loss. If the clinic mixes these together, the plan can become confused.
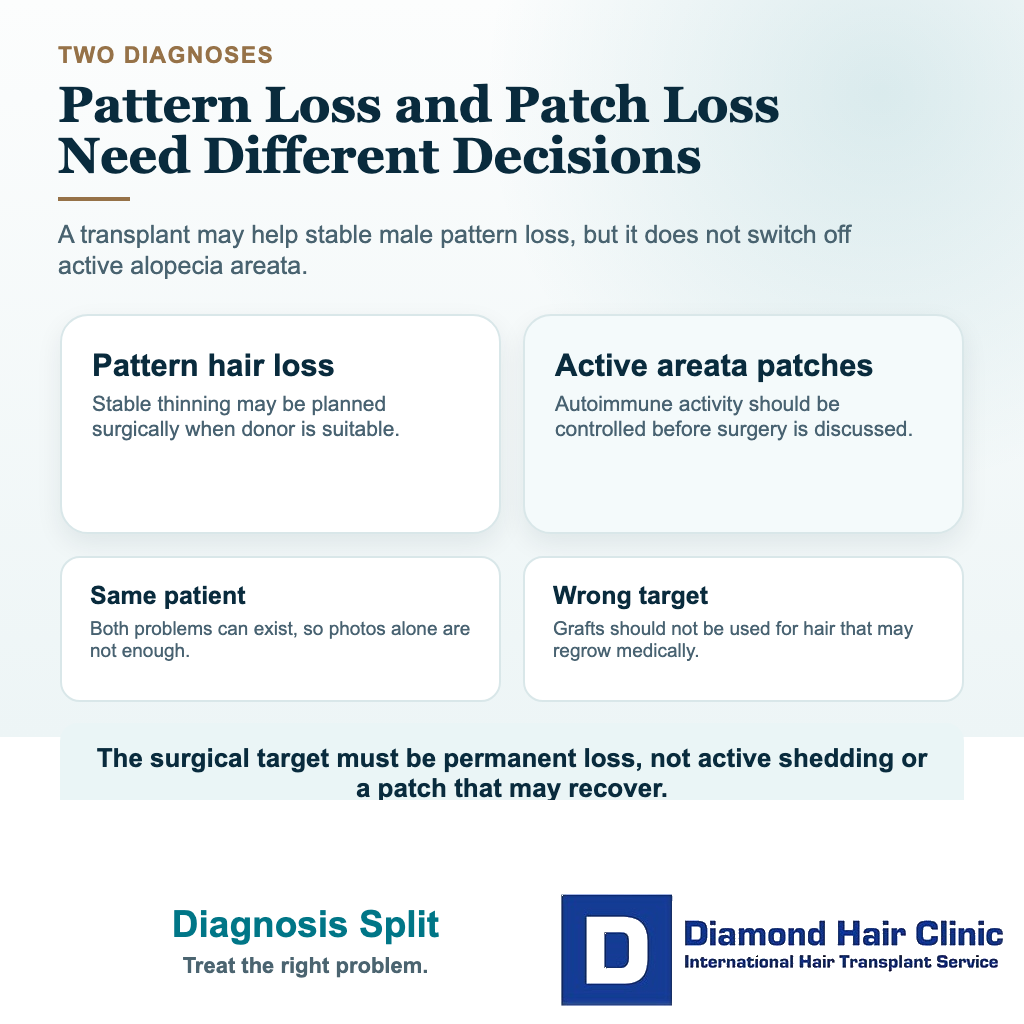
When I evaluate this kind of patient, I first ask which hair loss pattern we are treating. If the question is an active immune patch, surgery is usually not the first answer. If the question is a stable male pattern hairline while the autoimmune disease has been quiet, then surgery may be considered with caution.
Medication discussions can also be misunderstood here. Treatments used for male pattern hair loss are not the same as treatments used for immune-related patchy loss. Questions about finasteride, minoxidil, steroid injections, or newer immune treatments need separation, because these are not interchangeable tools. Medication before a hair transplant should not be improvised around surgery.
If the patient has diffuse thinning as well, the case becomes even more delicate. Diffuse thinning and hair transplant surgery require careful diagnosis because transplanting into unstable weak native hair can create disappointment.
When male pattern hair loss is clearly present, the hairline still has to be designed with long-term logic. A patient with this history may want a dramatic change because the hair loss has already taken so much from them emotionally. I understand that feeling, but the design must still be natural, age-appropriate, and responsible with donor supply. Natural hairline design in hair transplant surgery should not be drawn only from emotion.
In combined cases, I separate the problems in my mind. The male pattern component may be surgical. The immune patchy component may be medical. If both are treated as one problem, the patient may receive the wrong solution for at least part of the hair loss.
This is the point patients should not miss when they point to one area and say, “Just fill this.” The surgeon must ask why that area is empty, whether it may still regrow, and whether grafts are truly the right answer. Empty because of stable male pattern recession is one story. Empty because of an active immune patch is another story. They may look similar to the patient, but they are not the same surgical problem.
What if the patch might regrow without surgery?
This question matters because an immune patch can sometimes regrow with treatment or time. An empty-looking patch is not necessarily a dead patch. Alopecia areata is usually non-scarring, so the follicles may still be present but temporarily suppressed by immune activity. Moving donor hair into that area too early can waste grafts and confuse the later picture.
A transplant should not be used to replace patience when the biology is still active or recoverable. If the follicles are not destroyed, the problem may be immune activity rather than missing hair follicles. That is very different from scar tissue, burns, or permanent pattern hair loss, where the missing hair is less likely to return on its own.
Before I consider grafts, I assess what treatments have been tried, whether the patch is shrinking, whether fine regrowth is visible, and whether the dermatologist thinks the area is still medically active. Surgery should come after the diagnosis and treatment path are clear, not before.
Can surgery trigger or worsen the condition?
A patient with this history should understand that surgery is a form of controlled trauma to the scalp. In some people with inflammatory or immune-related skin and hair conditions, trauma and stress can be part of the story. I cannot responsibly tell every patient that surgery will trigger the disease. I also cannot promise that it will not.
This uncertainty is one reason I am conservative. If the disease has been quiet, the risk may be lower than during an active flare. But the patient still needs to know that surgery does not cure the condition. It only places hair into skin that may still have the tendency to react in the future.
I factor in the donor area. If patchy loss has affected the donor zone before, I become more cautious. The donor area is the resource we depend on for the transplant. If that area is not reliable, the foundation of the procedure becomes weaker.
Transplanted hairs are not protected from future immune activity simply because they were moved. If alopecia areata becomes active in that skin again, the visible result can change even when the operation itself was technically clean.
Guarantee language needs caution here. A hair transplant is never a guarantee, and immune-related hair loss adds another layer of uncertainty. A hair transplant guarantee can mislead patients when uncertainty is hidden.
A flare after surgery would not always mean the surgeon placed grafts badly. It may mean the disease has become active again. This distinction matters because patients often blame the wrong thing when hair changes. A surgical mistake and disease recurrence are not the same problem, and they require different responses.
Follow-up and documentation matter. If the scalp changes after surgery, clear photos and clinical review help separate normal shedding, shock loss, disease activity, and technical problems. Without that baseline, the patient may enter months of anxiety without a clear explanation.

What should I do before asking for graft numbers?
Before asking for graft numbers, the patient should confirm the diagnosis. If there is any doubt between immune-related patchy loss, male pattern hair loss, diffuse thinning, scarring alopecia, traction hair loss, or another scalp condition, surgery should wait until the diagnosis is clearer.
Graft numbers are tempting because they sound concrete. A patient feels lost, then a clinic offers a number and the uncertainty seems to disappear. But a graft number without diagnosis is not a plan. It is a sales shortcut.
Medical checks may also be appropriate depending on the story. A patient with sudden patchy loss, other autoimmune conditions, scalp inflammation, or unusual shedding should be assessed properly before a cosmetic surgery plan is made. Blood tests before a hair transplant are one part of medical readiness when health details may affect timing or safety.
The timeline often tells me more than the first graft estimate. I assess when the patches began, whether they are growing, whether they regrew before, whether treatment helped, and whether the donor area has ever been affected.
I check whether the patient has had eyebrow, beard, or body hair involvement. The disease can appear outside the scalp. If the condition is more widespread, that changes my level of caution. A small old patch is different from a disease pattern that keeps appearing in different places.
If the patient has already had a transplant elsewhere and is now losing hair in patches, I avoid jumping to conclusions. It may be normal shedding, poor growth, shock loss, male pattern progression, or immune disease activity. Thin hair transplant results can have more than one cause.
What if eyebrows, beard, nails, or body hair are involved?
The condition can sometimes affect more than one area. Eyebrow loss, beard patches, body hair changes, nail changes, or repeated patches in different places tell me that it may be more active or more widespread than a single scalp spot suggests.
That history does not by itself make surgery impossible, but it raises the level of caution. If the immune pattern is moving around the body, I try not to pretend that the scalp is separate from that biology. Hair transplant surgery depends on predictable donor and recipient area behavior.
If the history is closer to alopecia totalis or alopecia universalis, I become much more cautious. That pattern is not the same as one small patch that appeared years ago and fully recovered. The wider the immune pattern is, the less willing I am to use donor grafts before the disease has been understood medically.
In these cases, dermatology review becomes even more useful. It helps to know whether the disease is localized, recurring, expanding, or part of a broader autoimmune pattern before donor grafts are used.
How should the donor area be judged if patches have affected it?
The donor area must be judged very carefully if the disease has affected it. In ordinary male pattern hair loss, we rely on the donor area because it is usually more stable. With patchy autoimmune loss, that assumption may not hold if patches have appeared there.

If the donor area has a history of patchy loss, the surgeon must ask whether extracted grafts are coming from a reliable source. Even if the patch has regrown, the history still matters. A visually normal donor area today may not be the same as a permanently safe donor area.
I treat the donor area as a lifetime budget. Donor area management in hair transplant surgery becomes even more serious when the diagnosis is not straightforward. Wasting grafts in an unstable disease can remove options the patient may need later.
This history can also make the patient more anxious after surgery. If shedding occurs, the patient may not know whether it is normal shock loss, normal transplant shedding, male pattern progression, or disease activity. The diagnosis and baseline documentation must be clear before the operation.
When I assess donor safety, I do not only look at density. I look at the history of the donor area, how long it has been stable, whether previous patches fully recovered, and whether there is any diffuse weakness in the sides or back. A donor that looks acceptable at first glance may still need a cautious interpretation.
Rushed remote approval can miss the detail that changes the whole case. A few photos may hide a donor history that changes the whole plan. If a clinic approves a patient without asking whether the disease has affected the donor area, the assessment is incomplete.
How do clinic promises become misleading?
Clinic promises become misleading when they simplify the disease into a bald spot that can simply be filled. That may sound logical to a patient, but it ignores the disease behavior. The spot is not always the main problem. The immune tendency may be the main problem.
Some clinics say, “We can transplant into any bald area,” without asking why the area became bald. Others promise a high graft count to make the patient feel that the disease has been solved. This is not careful medical judgment.
I advise patients to prefer clinics that are comfortable with slower, harder medical judgment. Confirming the diagnosis, checking disease activity, reviewing donor involvement, and separating male pattern hair loss from immune-related patches are not delays for their own sake. They are how we protect the patient.
When comparing clinics, do not look only at price or dramatic results. Choosing a hair transplant clinic in Turkey should include judging whether the clinic understands when surgery is not the first answer.
Before and after photos can also mislead with this diagnosis. A photo may show improvement, but it may not tell whether the disease stayed quiet, whether medical treatment was used, whether the donor area was ever affected, or whether the patient was selected very carefully. The result image alone does not explain the risk.
The clinic should be comfortable saying that dermatology treatment comes first. It should also be comfortable telling the patient that transplant surgery is not a cure for the disease. If every discussion is turned into a package, a price, and a date, the patient should be careful.
How should I decide before asking for surgery?
Before moving toward surgery, the conversation should return to the diagnosis. With immune-related patchy loss, the first question is not how many grafts can be placed. The first question is whether surgery is the right treatment at all.
I need to know whether a dermatologist has confirmed the diagnosis, whether the condition is active or quiet, whether new patches have appeared recently, and whether the donor area has ever been affected. I also separate any male pattern hair loss from the immune condition, because those two problems may need different plans.
Medical treatment options need review before surgery is treated as the main solution. The clinic should also explain uncertainty. If waiting could change the diagnosis, reduce risk, or make the surgical plan safer, then waiting deserves respect.
If these details cannot be answered, the patient is not ready for graft numbers yet. Evaluation may be appropriate, but evaluation is not the same as surgery.
I am not trying to discourage the patient. I am trying to prevent the wrong operation. The most damaging hair transplant decisions often happen when the patient is asking for certainty and the clinic is too eager to provide it.
If the decision still feels uncertain after proper evaluation, I do not conclude that the answer is hopeless. It may mean the next step is diagnosis and stabilization. I prefer to help a patient take the right next step rather than push him into the wrong surgery.
There are cases where the most responsible advice is not surgical at all. That can be disappointing, but it can also protect the patient from losing donor grafts, money, and trust. A useful consultation explains what surgery can do, and also what surgery should not be asked to do.
When is it better to treat first and wait?
It is better to treat first and wait when the disease is active, when patches are spreading, when the diagnosis is uncertain, when the donor area has been involved, or when the patient is asking surgery to solve an immune condition that has not yet been controlled.
Waiting can be emotionally hard. Patchy hair loss can feel unfair because it appears suddenly and visibly. A patient may want the solution that sounds fastest and most permanent. But the fastest sounding solution is not always medically sound.
If the disease becomes stable, the diagnosis is clear, and the patient has a separate surgical problem such as male pattern hairline recession, then a careful conversation may become possible. The plan should still be conservative, realistic, and based on long-term safety.
When waiting is chosen, the patient should not feel abandoned. There should be a plan. Dermatology review, photographs, treatment response, observation period, and later reassessment can all be part of the path. The plan should make the final decision stronger, not feel like delay for its own sake.
I also tell patients that not every patch needs to be transplanted. Some patches may regrow. Some may respond to treatment. Some may remain risky. The fact that a bald area exists does not always mean the best answer is graft placement.
I am direct about this. Alopecia areata should usually be treated and stabilized before hair transplant surgery is considered. Surgery may be possible only in selected, stable situations where the diagnosis, donor area, and patient expectations are clear. A surgeon should know when to operate, and also when not to operate.



