- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 10 Minutes
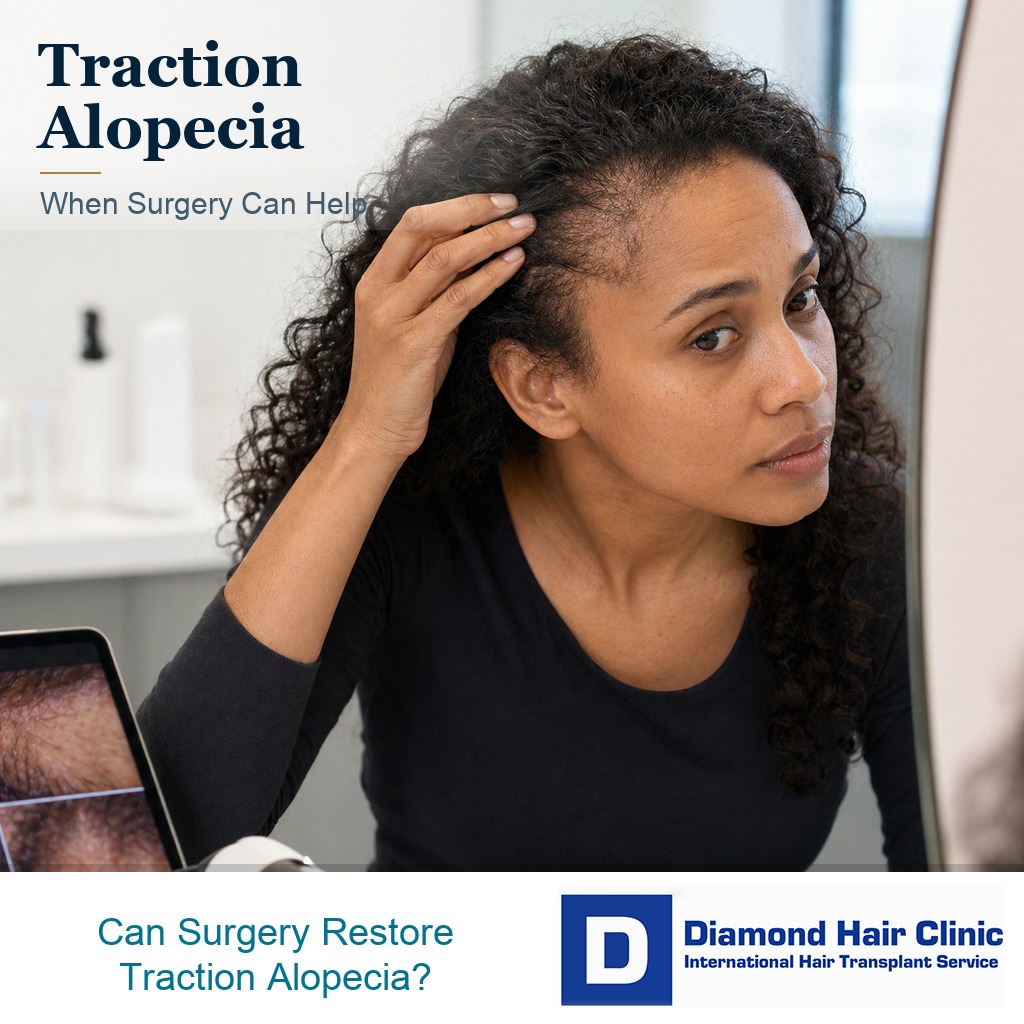
Traction Alopecia Hair Transplant Repair
Yes, a hair transplant can repair traction alopecia in carefully chosen patients, but only when the pulling has stopped and the hair loss is truly permanent. If the follicles are only weakened, the better first step is to protect natural recovery. If years of tension have destroyed the follicles, surgery may be useful, especially around the hairline, temples, sideburns, or edges.
The unsafe decision is treating every thin edge as a transplant case. Before I would consider surgery, the diagnosis should be correct, the area should be stable for at least 6 to 12 months, there should be no active inflammation, and the patient must be able to avoid returning to the same tension that caused the loss.
Practically, if the traction is still active, surgery should wait. If the scalp is settled, the pulling has stopped, the loss is stable, and the empty area is truly permanent, a carefully planned FUE hair transplant may be a reasonable option.
Why is it not the same as pattern hair loss?
Traction alopecia is caused by repeated pulling on the hair. Tight braids, ponytails, buns, extensions, weaves, turbans, clips, glued systems, tight wig bands, and repeated styling stress can damage follicles over time. The pattern is usually strongest where the pull has been greatest, often around the front hairline, temples, sideburns, or edges.
Pattern hair loss behaves differently. It follows a genetic process where follicles gradually miniaturize, often in a predictable hairline, crown, or diffuse pattern. The treatment strategy changes because a transplant for traction alopecia may be a localized repair, while pattern hair loss needs long-term planning for future progression.
This distinction is not only academic. If a patient thinks the weak point is traction but actually has female pattern hair loss, the transplanted area may be planned incorrectly and the surrounding hair may continue to thin. Careful female hairline hair transplant planning matters when a woman has edge or temple loss.
It is also different from repeated hair-pulling behavior, where the injury comes from pulling the hair out rather than a hairstyle placing tension on the edge. In both situations, the damaging behavior has to be controlled before donor grafts are used.
In men, the same caution applies. A young man may blame long hair, tight tying, a very tight turban, or repeated styling, while the examination also shows androgenetic recession. If I ignore the genetic pattern, I may restore one visible area but leave the patient with a result that becomes unnatural as the rest of the hair changes.
When can the lost hair grow back without surgery?
If the traction injury is early, the follicles may still be alive. In that stage, stopping tension can allow improvement over months. Surgery should not be rushed when the area still has short fine hairs, changing density, recent shedding, or visible recovery after the damaging hairstyle was stopped.
The first treatment is not surgical. The first treatment is removing the cause. The patient must stop the tight style, avoid heavy extensions, reduce chemical stress, and give the scalp time to recover. If inflammation, itching, flaking, tenderness, bumps, or breakage is present, the scalp should be treated before surgery is discussed.
Some early cases begin to show small signs of improvement after a few months, but recovery should not be judged too early. Hair cycling is slow. A patient may stop the pulling today, but the scalp still needs time before we understand whether the follicles are recovering or whether the loss has become permanent.
Medication can sometimes support regrowth when follicles are weak but not destroyed. Here, medication before a hair transplant may matter, especially if there is also pattern hair loss, shedding, or another medical reason for thinning.
Serial photographs with the same hairstyle, lighting, and hair length are useful. A single photo does not tell me whether the area is improving, stable, or getting worse. If the edge is slowly filling in, surgery may be unnecessary or should be delayed.
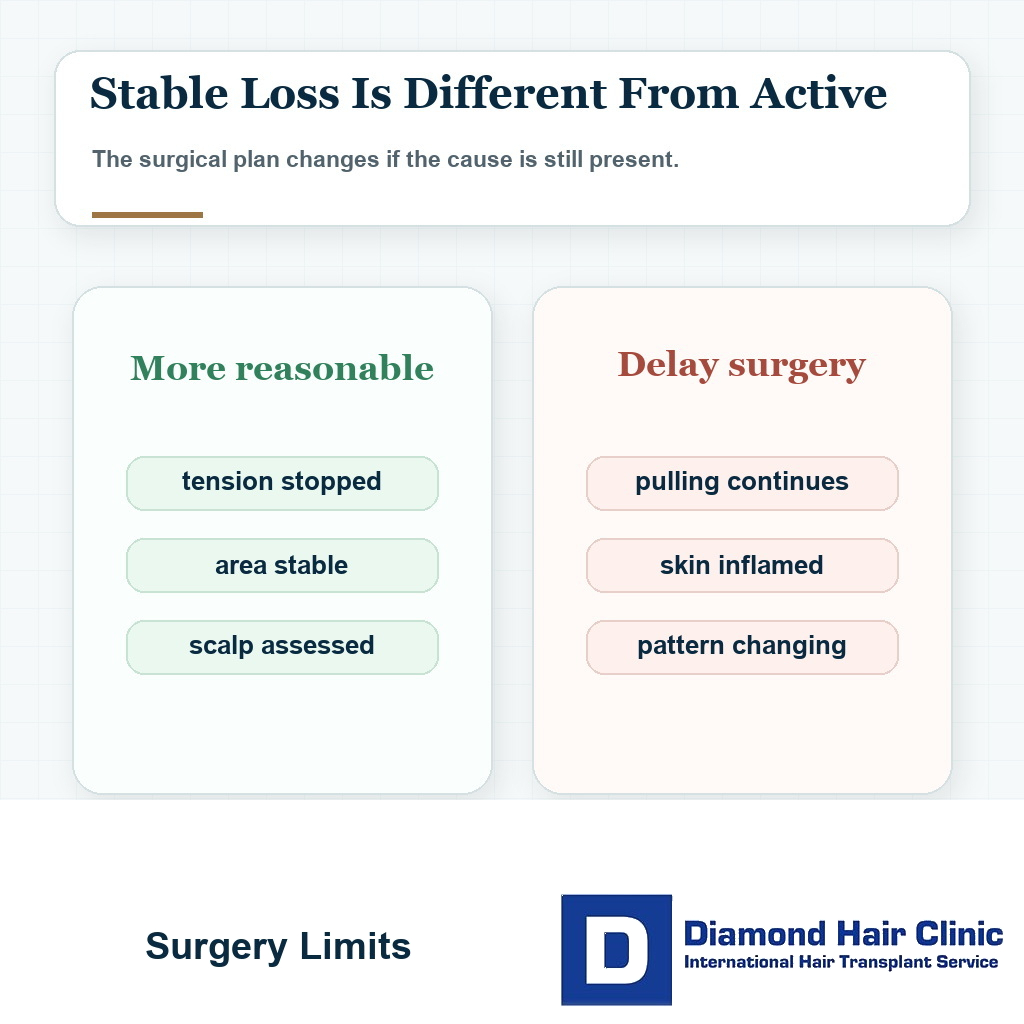
What should change before surgery is considered?
Before surgery is considered, the damaging routine has to change in a real and repeatable way. It is not enough to stop one tight hairstyle for a few weeks and then replace it with another habit that pulls on the same edge. The scalp needs a new pattern of protection that the patient can actually maintain.
The issue is not blaming a hairstyle or asking the patient to abandon every style, covering, or cultural habit. It is about changing the mechanics so the same fragile edge is no longer pulled, rubbed, glued, or loaded every day. A style can feel protective socially and still be too much mechanical stress for one damaged hairline.
The daily styling routine matters. Braids should be looser, lighter, and less frequent. Wig bands should not rub the same frontal edge every day. Clips, glue, extensions, and head coverings should not keep creating pressure on the same damaged area. If the routine still injures the edge, surgery should wait, even if the patient is emotionally ready for repair.
This step is not cosmetic advice. It is surgical protection. A transplant can move healthy follicles into a damaged area, but it cannot make those follicles immune to renewed tension. The best repair begins before the operation, with a scalp that is no longer being injured.
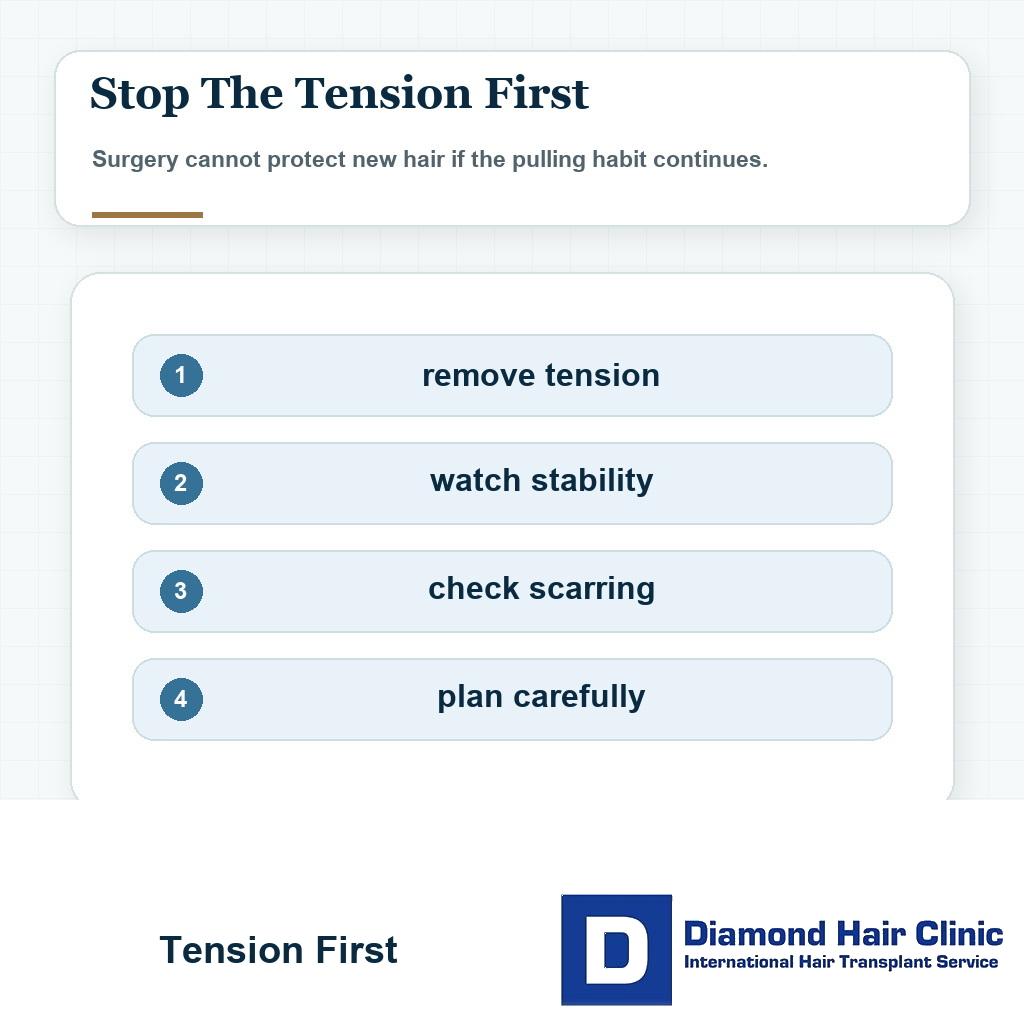
How can I tell if it is still active?
Active traction damage often gives clues before the area becomes completely empty. Pain during styling, stinging, tenderness, redness, small bumps, crusting, flaking, raised or tented skin at the hairline, broken hairs, and worsening recession after each tight style are not small details. They are warning signs that the scalp is still being injured.
What the patient feels matters as much as what I see. A hairstyle that hurts is not a protective style for that patient. A wig that grips the same edge every day is not harmless. A tight band that rubs the same frontal area may continue the problem even if the patient no longer wears braids.
If the scalp is still angry, surgery is not the first answer. A transplant placed into an unstable or inflamed environment may be a poor decision. The pulling needs to be stopped, the irritation needs to settle, and the area needs observation before donor grafts are used.
The real daily routine has to be discussed. It is easy to say that the tight style has stopped. I need to know whether the patient has replaced it with another habit that still pulls, clips, glues, or rubs the same fragile area.
When should a dermatology review come before a hair transplant?
Dermatology review should come first when the story does not behave like straightforward traction alopecia. Ongoing burning, pain, scale, pustules, spreading patches, sudden shedding, or loss beyond the pulled area can point to another diagnosis that should be treated before surgery.
The case needs extra caution when traction alopecia overlaps with female pattern hair loss, central centrifugal cicatricial alopecia, lichen planopilaris, alopecia areata, or a medical shedding problem. The patient may still have traction damage, but that may not be the whole explanation.
If the diagnosis is uncertain, confirming the scalp condition is safer than using donor grafts in an area that may still be medically active. That is not delaying for its own sake. It is how we avoid treating the wrong problem with surgery.
What does smooth shiny skin along the edges usually mean?
Smooth shiny skin along the edges can be a warning sign. It may suggest that the follicles have been damaged permanently, especially if the area has looked the same for a long time after the pulling stopped.
I do not diagnose permanence from one description alone. The scalp should be examined for follicular openings, small remaining hairs, skin quality, and comparison with older photos if possible. But when the skin looks smooth, empty, and unchanged over time, natural regrowth becomes less likely.
Here, many patients become confused. They may try oils, massages, supplements, serums, or minoxidil for months and feel frustrated when nothing changes. The key question is whether the follicle is still alive. A weak follicle can sometimes recover. A destroyed follicle cannot be stimulated back into existence.
If the skin quality is poor or scar-like, density should be more conservative. Forcing too many grafts into fragile skin can weaken the result rather than improve it. The plan should restore a natural edge while respecting blood supply, healing capacity, and donor limitations.
When does it become a surgical problem?
The condition becomes a surgical problem when the hair loss has become stable and permanent. The area may look smooth, shiny, or sparse for a long time, and the patient may no longer see meaningful regrowth after stopping the pulling. At that point, replacing lost follicles with grafts may be reasonable.
Surgery becomes more reasonable when the patient has been free from damaging tension for at least 6 to 12 months, the pattern has not expanded, the scalp is settled, and there is no sign of active inflammatory disease. In longstanding cases, I may need even more observation before using donor grafts.
Permanent traction damage can behave like a small scarred recipient area. That point does not mean surgery cannot work, but it means the density goal must be moderate and the graft placement must respect the skin quality. If the skin has reduced blood supply or scarring, aggressive dense packing can be a poor decision.
I separate mechanical traction from inflammatory scarring alopecia before hair transplant. With traction, the trigger is pulling. With inflammatory scarring alopecia, a disease may still be attacking follicles. The surgical risk is different, so the diagnosis must be exact.
What do I check before saying a patient is a candidate?
Before I call someone a candidate, I examine the recipient area, the donor area, the remaining native hair, and the habits that caused the problem. The patient also has to be able to protect the transplanted hair afterward. If the same tight style continues, surgery is not a solution. It is only a delay before another injury.
Mixed hair loss also has to be considered. Many patients have traction damage plus another problem, such as female pattern hair loss, diffuse thinning, nutritional deficiency, postpartum shedding, central centrifugal cicatricial alopecia, or androgenetic recession in men. If I miss the second diagnosis, the transplant plan becomes too narrow.
In some patients, the diagnosis is clear from the pattern and history. In others, a closer scalp examination is needed. If the signs do not fit straightforward traction damage, surgery should not be rushed. A transplant placed into an active inflammatory scalp disease can be a mistake. In selected cases, dermatologic evaluation, trichoscopy, or biopsy may be needed before surgical planning.
Candidacy is not simply about whether grafts can be inserted. A good candidate for a hair transplant has a stable problem, a safe donor area, a realistic goal, and a plan that protects the future.
Traction repair is usually a refinement operation. It can improve visible gaps, edges, or hairline shape, but it should not be sold as a way to create unlimited density or reverse every styling injury perfectly.
How should the hairline or edges be designed?
This condition often affects the most visible part of the face, so design matters deeply. The aim is not to draw a new hairline that looks impressive in a clinic photo. The plan should restore a natural frame that matches the patient’s age, facial proportions, hair type, and future styling.
For women, the edges and temples need soft irregularity. A harsh wall of grafts can look artificial, especially when hair is pulled back. For men, the surgeon must also check whether the apparent traction pattern is hiding normal recession. A low youthful line may create a problem later if genetic hair loss continues.
Natural hairline design matters for this reason. The first row should not look like a straight border. The angle, direction, density, and transition from the face into the hair must be planned with discipline.
Temple points and sideburn areas need special planning. These areas are unforgiving. If the angle is wrong, the grafts may grow outward or stand separately from the native hair. A small technical error can be very visible because the patient often wears the hair away from the face.
A natural edge also needs a gradual transition. I avoid thick multi-hair grafts placed at the very front. The visible border should be built with fine single hairs, then the density can increase behind them. These are the details that separate natural reconstruction from simply filling empty skin.
Why does hair type change the plan?
Hair type changes the surgical plan because curl, caliber, contrast, and styling habits all affect coverage. Curly and coiled hair can create excellent visual coverage when placed correctly, but the grafts may be harder to extract and the angle must be respected carefully.
Patients with Afro-textured or very curly hair often ask about edge loss because tight protective styles, braids, extensions, weaves, and wigs may have contributed to the problem. The answer is not to blame the hairstyle. The answer is to understand the mechanical history and then plan surgery around the hair’s natural curl and direction.
Afro curly hair transplant planning is relevant when traction affects the edges. Curved follicles, curl direction, and hair exit angle matter. The surgeon cannot treat every hair type with the same extraction and placement strategy.
With Afro-textured or very curly hair, the challenge is not only extraction. It is also the direction of growth at the edge. A technically correct graft can still look wrong if the exit angle does not follow the natural curl and facial frame. I avoid using a generic hairline template for this kind of repair.
Fine hair creates a different problem. It may require more careful expectation setting because each graft gives less visual coverage. In that case, fine hair and hair transplant planning becomes relevant, especially if the patient wants strong coverage along a visible edge.
Can wigs, extensions, hair systems, or tight coverings damage the result?
Yes, they can damage the result if they continue to pull, rub, clip, bond, or place repeated pressure on the same fragile area. A wig, extension, hair system, scarf, cap, or covering is not always harmful. The weaker point is the mechanical stress it creates on the scalp.
Many patients stop one damaging habit but continue another. They may stop tight braids but use wig combs in the same temple area. They may stop extensions but use glue near the frontal edge. They may avoid ponytails but wear a tight band every day. From the scalp’s perspective, the label does not matter. The repeated stress matters.
After a transplant, the threshold should be even stricter. New grafts need a healthy scalp environment. If a bonded system, tight wig, strong adhesive, or repeated clip pressure sits over the treated area too early or too aggressively, it can interfere with healing and may create new trauma.
The same principle applies to a hair system after a hair transplant. Surgery can restore follicles, but it cannot make the scalp immune to the same mechanical injury that caused the original loss.
A patient cannot repair the area surgically and then return to the same pulling pattern. The operation and the future hairstyle must work together. Otherwise, the transplant may improve the area for a while but the underlying behavior remains unchanged.
How many grafts are usually needed?
There is no responsible graft number without examination. Some repairs need a small number of grafts because the loss is limited to the temples or side edges. Other cases need more because the frontal border, sideburns, and temple areas are involved.
In a small temple or edge repair, the number may sometimes be in the several hundred graft range. If the frontal border, both temples, and sideburn areas are involved, the number can move much higher. In larger cases, it may enter the 1,000 to 2,500 graft range or more. But the number is never the starting point.
The starting point is the size of the permanent loss, the skin quality, the hair caliber, the curl pattern, the density behind the edge, and the donor area. I avoid giving a number from photos alone when the skin quality is uncertain. Scarred or thin skin may not accept the same density as normal scalp.
If a clinic promises a high number without discussing skin condition, donor quality, and long-term hairstyle habits, that is a warning sign. Graft numbers can sound impressive, but they do not guarantee naturalness, survival, or long-term safety.
The donor area is still a limited resource, even when the patient’s hair loss is caused by traction. Donor area planning matters because every graft used at the hairline is a graft that cannot be used later. A small visible repair can be worthwhile, but it should still respect the lifetime safe donor supply.
The best plan is usually not the biggest plan. In this condition, a moderate density that blends naturally is often safer than trying to recreate childhood density. The improvement should be visible without the surgeon overloading fragile skin.
Can minoxidil or PRP replace surgery?
Minoxidil, PRP, and other supportive treatments may help when follicles are miniaturized, inflamed, or recovering, but they cannot bring back follicles that have been permanently destroyed. This is the main distinction I explain to patients. Treatment can support weak follicles, but it cannot create new follicles in a scarred empty area.
If there are small hairs, recent shedding, or partial recovery after stopping traction, medical support and observation may be better before surgery. In carefully chosen patients, oral minoxidil before hair transplant may be part of a broader plan, but it must be chosen carefully and medically supervised.
Topical treatment may also be discussed in early traction cases, especially when the skin still has visible hairs and the plan is to support recovery. Patients should not think of minoxidil as a magic test. Some weak follicles may respond. A smooth permanent area may not.
PRP treatment for hair loss can be discussed for scalp quality or weak native hair in selected cases, but it should not be presented as a guarantee. Add-on treatments should not distract from the main question. Are the follicles still alive, or is the area permanently empty?
If the area is truly permanent, surgery may become the direct solution. If the area is still recovering, surgery may be premature. The skill is knowing which situation is in front of us.
How do clinic promises mislead patients with edge loss?
A rushed clinic may oversimplify edge loss by saying the area only needs grafts. That answer is too fast. The surgeon should first ask whether the diagnosis is correct, whether the pulling has stopped, whether there is scarring, whether there is another hair loss condition, and whether the patient’s future styling will protect the result.
It worries me when the consultation focuses only on graft numbers or before-and-after photos. A visible edge repair can look dramatic, but the long-term result depends on the diagnosis, the design, and whether the patient stops the damaging traction. If those questions are ignored, the transplant may solve the photo and fail the patient.
Patients should also be careful when comparing clinics only by price. Edge repair is not a basic filling job. The area is visible, the angle is unforgiving, and the density must be planned around skin quality. Choosing only by the cheapest offer can be risky, especially if the consultation does not explain diagnosis, design, donor limits, and follow-up.
Patients researching surgery in Istanbul or Turkey can read more about red flags of hair transplant clinics and hair transplant cost in Turkey. Price matters, but it should not be the only deciding factor in this kind of repair.
This also matters when the patient asks about lowering a naturally high forehead. Hairline lowering and traction repair are not the same operation. One changes facial framing in a stable normal scalp. The other repairs damage from tension and may involve fragile or scar-like skin.
A good consultation should leave the patient clearer, not rushed. A surgeon-led plan should explain what surgery can improve, what it cannot fix, and what habits must change before grafts are placed.
How should I protect transplanted hair afterward?
After surgery, protection is not only about the first few days. The early healing phase matters, but the long-term hairstyle routine matters too. A patient who has repaired the edges surgically must learn how to protect those edges afterward.

During early recovery, proper hair transplant aftercare matters. The patient needs to avoid friction, avoid pressure, and avoid anything that touches or pulls the recipient area before the grafts are safe. In the first 10 to 14 days, the skin is still healing and the new grafts should not be tested.
But the first year also matters. Tight braids, heavy extensions, strong pulling, glued systems over the treated area, or repeated tension on the new frontal edge should be avoided. The transplanted hairs need time to grow, mature, and blend with the native hair. The scalp also needs a healthy environment.
The styling plan also needs realism. Very tight ponytails, sleek pulled back styles, heavy weaves, and repeated edge manipulation may be exactly what created the problem. After surgery, those habits should not return in the same way.
The transplant can restore follicles, but it cannot change the rules of biology. If the same mechanical stress continues for years, even a good surgical result can be placed under unnecessary risk.
What should be clear before you choose surgery?
This can be one of the more satisfying hair transplant indications when the diagnosis is correct and the loss is stable. A localized edge or hairline repair can make a real difference to the way a patient feels when the hair is tied back or styled away from the face.
I do not treat this concern as vanity. Edge loss can change how a patient styles the hair, covers it, and feels in public. That emotional weight is real, but it should not push the surgery ahead of diagnosis and stability.
There is no benefit in rushing. If the area is still changing, if the pulling has not stopped, if there is inflammation, or if another hair loss condition is present, surgery should wait. A transplant should not be used to hide an active problem.
The safest repair is not the one with the highest graft number. It is the one done after the cause has stopped, the diagnosis is clear, the donor area is protected, and the design is conservative enough to age naturally.
The central point is this. Surgery can restore lost hair, but it cannot protect the result from the same tension that caused the loss. The real treatment is surgery plus a long-term change in how the hair is handled.
That is the standard I would use for my own patient. First stop the damage. Then confirm the diagnosis. Then observe stability. Only after that should we decide whether surgery truly makes sense.


