- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 4 Minutes
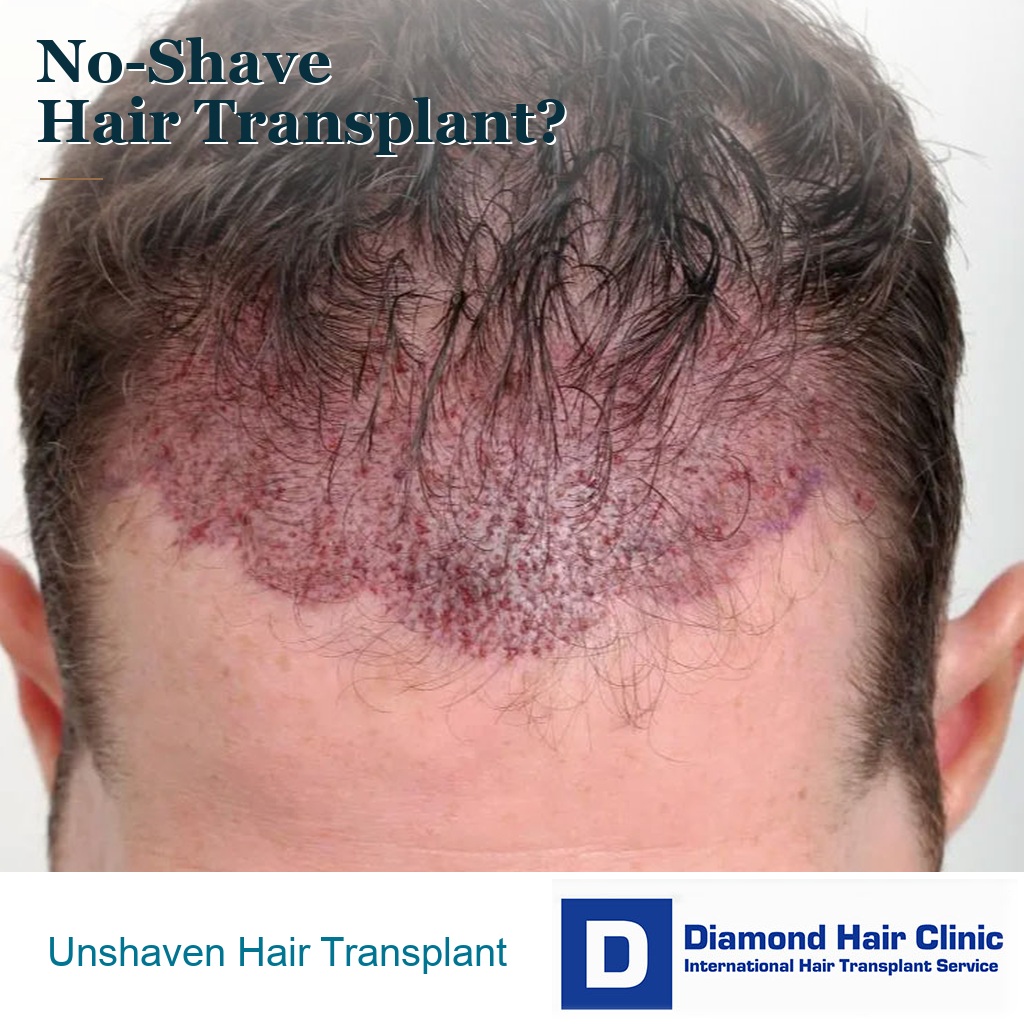
Can an Unshaven Hair Transplant Be Done Safely?
Yes, an unshaven hair transplant can be done safely in specific cases, but it is not necessarily the best or safest choice. I only consider it when the graft number is limited, the donor area can be seen clearly enough, the recipient area can be handled without fighting through long hair, and the patient understands that discretion should never come before graft survival, donor protection, or natural placement.
The main risk of unshaven surgery is not that the idea is wrong. The weaker point is that the technique is used for the wrong patient. Long hair can hide the operation from other people, but it can also hide the scalp from the surgical team. When visibility becomes weaker, extraction, angle control, density planning, washing, and early monitoring can all become more difficult.
I do not treat unshaven hair transplant as a luxury upgrade. I treat it as a technical decision. Sometimes it helps the patient socially. Sometimes it makes the operation less clean, less efficient, and less predictable. The correct answer depends on the scalp, not on the marketing name.
What is an unshaven hair transplant?
An unshaven hair transplant is a hair transplant plan where some or all of the visible hair is left long instead of shaving the entire scalp. The goal is usually privacy. Patients want to return to work, family, or public life without the obvious appearance of a shaved head.
In practice, the word unshaven can mean several different things. In one patient, only a small donor window is shaved and hidden under longer surrounding hair. In another patient, the recipient area is left long while the donor area is shaved. In a smaller group, the surgeon may attempt a more complete no shave approach.
These are not the same operation. A hidden donor window is very different from trying to extract and implant grafts while almost all hair remains long. Before a patient agrees, he should know exactly what will be shaved, where it will be shaved, and how visible it may be after surgery.
The method usually still uses FUE hair transplant principles. Some clinics describe the implantation as DHI, but DHI is a way of placing grafts within the FUE family rather than a separate guarantee of better results. The tool matters less than whether the surgeon can see, protect, and place the grafts correctly.
Why do patients want no shave hair transplant surgery?
Most patients ask for no shave surgery because they want privacy. They do not want coworkers, relatives, clients, or friends to notice a sudden change in hairstyle. Women and patients with long hair often have an especially strong reason to avoid a visible shave.
I understand this concern. Hair transplantation is personal, and not every patient wants to explain surgery to the people around him. A discreet recovery can reduce stress, especially for patients in public facing work or patients who cannot take long time away from daily life.
But privacy is only one part of the decision. The operation still has to be safe. The donor area still has a limited supply. The grafts still need careful handling. The recipient area still needs correct angle, direction, spacing, and depth.
If a patient chooses no shave surgery only because he is embarrassed, without understanding the surgical compromise, the decision can become risky. I would rather have a patient feel temporarily self conscious than accept a weaker surgical field that may affect the final result.
What are the main types of unshaven hair transplant?
The most common practical option is a partial donor shave. The surgeon clips one or more small donor windows, extracts grafts from those areas, and the longer surrounding hair covers the shaved zones. This can work well when the patient has enough length and the graft number is modest.
Another option is an unshaven recipient area with a shaved donor area. This may be considered when the recipient area still has enough native hair to hide early redness or scabs, while the donor area is prepared more traditionally for extraction.
The most technically demanding option is a fully unshaven approach. In this plan, both the donor and recipient areas remain largely unshaven. I consider this only in very selected cases because it can reduce visibility, slow the operation, and increase the chance of technical compromise.
There is also long hair FUE, where grafts are extracted with longer hair shafts attached. This can sometimes give a preview of direction or coverage, but it is not a magic result. The visible shafts can still shed after surgery, and the operation remains technically demanding.
The medical literature around unshaven and long hair FUE is useful, but it needs the right interpretation. It supports the idea that these methods can work in specific cases and experienced hands. It does not prove that keeping the hair long is safer for every case. For me, the evidence supports careful selection, not routine no shave surgery for everyone.
The patient should never accept a vague promise of invisible surgery. He should ask which version is being offered, how many grafts are realistic, and what tradeoff is being made for discretion.
Why do I often prefer a partial shave instead of a fully unshaven plan?
A partial shave often gives the best balance between privacy and surgical control. The patient may keep enough surrounding hair to cover the donor area, while the surgeon still works through a clean and visible donor window.
It matters because donor extraction should be spread responsibly. If the shaved window is too small for the requested graft number, the surgeon may be tempted to take too many grafts from one limited area. That can create a patchy donor appearance even if the first week looked discreet.
A partial shave also makes the plan more reliable. The patient knows where the work will happen, the team can see the donor field clearly, and aftercare is easier than in a fully unshaven plan.
I prefer this kind of compromise when discretion is important but surgical precision should not be sacrificed. In my mind, the best hidden procedure is not the one that hides every sign at any cost. It is the one that protects the result while reducing unnecessary visibility.
Why can shaving make a hair transplant safer?
Shaving gives the surgeon a clearer surgical field. In the donor area, it helps me see exit angles, spacing, density changes, and the pattern of extraction. In the recipient area, it helps me control angle, direction, depth, and distribution.
Hair transplantation is not only placing hairs into empty skin. It is a series of small decisions repeated thousands of times. If visibility is reduced, the margin for error becomes smaller.
A shaved field also makes cleaning and early monitoring easier. After surgery, the patient and clinic can see scabs, redness, irritation, folliculitis, or unusual healing more clearly. It matters because early aftercare is not only cosmetic. It protects the grafts and the skin.
This point does not say every patient must be fully shaved. It means shaving is not a punishment or an outdated habit. Commonly, it is the safer and more precise way to perform the operation.
What risks can unshaven surgery create?
The first risk is reduced visibility. If the surgical team cannot clearly see the donor area, extraction may become less controlled. This can increase the risk of transection, uneven extraction, or unnecessary trauma to nearby follicles.
The second risk is less precise recipient area work. Long native hair can fall into the field, obscure the angle of existing hair, and make it harder to create a soft natural pattern. This matters most in the frontal hairline, where even small direction mistakes can become visible after growth.
The third risk is harder cleaning. Hair can trap crusts, dried serum, and products. If the patient is afraid to separate the hair and wash properly, scabs may stay longer or irritation may increase. I connect no shave surgery with very clear washing after hair transplant instructions.
The fourth risk is false reassurance. The patient may look less operated on, but Do not read that as the surgery was easier or safer. A discreet first week is not the same thing as a better long term result.
The fifth risk is cost and time pressure. Unshaven work can take longer and may cost more. That extra time is only worthwhile if it protects the patient socially without weakening the surgical quality.
Can Sapphire FUE or DHI remove the risks of no shave surgery?
No technique name removes the need for visibility and careful planning. Sapphire FUE can be useful for recipient area work when it is selected correctly, and DHI hair transplant can help in certain implantation situations, but neither one makes every no shave case safe.
The tool does not decide the hairline. The tool does not protect the donor by itself. The tool does not know whether the patient has diffuse thinning, weak donor density, or unrealistic density expectations.
I become more careful when a clinic presents DHI or Sapphire FUE as a way to make an invisible transplant easy. These tools can be valuable in the right hands, but the surgeon still needs to control depth, angle, spacing, graft handling, and donor distribution.
For the patient, The decision is not which label sounds more advanced. The practical issue is whether the chosen method gives the surgical team enough access to do the work well.
Who may be suitable for an unshaven hair transplant?
A better candidate usually needs a smaller or moderate number of grafts, enough hair length to hide a limited donor shave, stable hair loss, and a realistic goal. The donor area should be strong enough to allow careful extraction without overusing one hidden zone.
Women and long haired patients can sometimes benefit from a partial shave plan because the surrounding hair may hide the donor window well. This can be emotionally important, especially when the patient cannot comfortably appear with a shaved head.
Patients who need a small hairline refinement may also be candidates if the recipient area can be accessed clearly. The practical detail is not only the number of grafts. The practical detail is whether the surgeon can still work with precision.
I check personality and aftercare. A patient who is extremely anxious about anyone noticing the surgery may become too afraid to wash properly or send clear photos. In those cases, the desire for privacy can interfere with recovery.
Suitability is case specific. It should be decided after examining hair length, donor density, hair caliber, recipient area needs, skin condition, and future hair loss risk.
Who should be cautious about no shave surgery?
Patients with extensive baldness, high graft needs, diffuse thinning, weak donor density, or unstable hair loss should be cautious. These cases often need maximum visibility and careful long term donor planning.
Diffuse thinning is especially important. When native hairs are spread throughout the recipient area, the surgeon must protect existing hair while placing grafts between them. Long hair can make this more difficult, and the patient may also be more vulnerable to native hair shock loss.
Patients who need major crown work should also be careful. Crown hair transplant planning already requires discipline because the crown can consume many grafts. If the unshaven approach limits visibility or graft distribution, the result may become weaker.
Patients with scalp inflammation, heavy dandruff, folliculitis, poor hygiene during recovery, or a history of difficult healing may also be better served by a clearer surgical field and easier aftercare.
If a clinic says everyone is suitable for no shave surgery, I would slow down. That is not surgical judgment. That is marketing.
Can an unshaven hair transplant still look natural?
Yes, it can look natural if the patient is suitable and the surgery is planned well. Naturalness does not come from shaving or not shaving. It comes from correct hairline design, graft selection, angle, direction, distribution, and donor management.
For the frontal hairline, I want soft irregularity, fine single hair grafts at the front edge, and a transition that does not look drawn. If long hair blocks visibility, the surgeon may lose some control over the details that make the hairline natural.
I still connect the decision to hairline design in hair transplant. A private recovery is not enough if the final hairline looks artificial.
A good no shave result is not simply hidden in the first week. It should still look natural after the hair grows, after shedding, under daylight, and with normal styling.
Does no shave surgery make recovery easier?
It can make the recovery less visible, but not always easier. These are different things.
Long hair may help cover a donor window or reduce the shock of a new appearance. Even so, it can make washing slower, make scab removal more awkward, trap products, and make it harder to see whether the skin is healing normally.
The patient may also need to be more careful with styling. Brushing, pulling, tying, clipping, or moving long hair around the grafts can create avoidable friction during the early period.
If the patient wants to use hats, fibers, or styling for privacy, timing matters. A loose hat may be reasonable at the right stage, but tight pressure is not safe early. I explain this separately in my guide to wearing a hat after hair transplant. The same caution applies to hair fibers after hair transplant, which should not be used too early over healing skin.
The responsible answer is that no shave surgery may make you look less changed, but it does not remove the need for careful aftercare.
How does no shave surgery affect scabs, washing, and early checks?
Long hair can make the first days feel more private, but it can also make basic care more awkward. The patient may be afraid to separate the hair, touch the scalp correctly, or clean crusts when the time is right.
Scabs can hide under longer hair. Redness can be harder to see. Small areas of irritation may be noticed later than they would be on a shaved scalp. This is not a reason to panic, but it is a reason to receive very clear aftercare instructions.
When scabs begin to loosen, patients sometimes worry that the hairs inside the crusts are lost grafts. I explain this separately in my article about scabs coming off after hair transplant, because this fear is common even after an ordinary shaved procedure. With longer hair, the fear can be stronger because everything is harder to see clearly.
Good no shave aftercare should explain how to wash, how to dry, how to move the surrounding hair, what photos to send, and what warning signs should prompt medical review. The patient should not be left guessing because the operation was marketed as discreet.
How many grafts can be done with an unshaven plan?
There is no accurate universal number. The safe number depends on donor density, hair length, the number and size of hidden donor windows, the recipient area, the team experience, and how much visibility the surgeon is willing to sacrifice.
In general, smaller cases are more suitable. As graft numbers rise, the hidden donor area may become too large, extraction may become concentrated, and the operation may take longer than is ideal.
I am cautious when a clinic promises a very large no shave session without explaining donor distribution. A high graft number can sound impressive, but if it is taken from a limited hidden zone, the donor may become patchy or depleted.
That is the reason I slow down around giving graft numbers from hairstyle alone. A patient may have long hair that hides the donor well, but the safe donor capacity may still be limited. Another patient may have shorter hair but excellent donor strength. The visual cover is only one part of the calculation.
I keep returning to donor area management. A patient should not trade long term donor safety for a short term private recovery.
Does an unshaven hair transplant cost more?
It often costs more because it takes more time, demands more focus, and may reduce the number of grafts that can be handled efficiently in one day. But higher cost does not necessarily mean better surgery.
The patient should ask what the extra cost is paying for. Is it paying for more surgeon time, careful extraction, slower placement, and better planning? Or is it simply a marketing label attached to a standard surgery?
If cost is part of your decision, it is better to understand the broader picture of hair transplant cost in Turkey. A fair price should support enough time, proper medical responsibility, trained staff, safe tools, and clear follow up care.
I would not choose no shave surgery only because it sounds premium. I would choose it only when the surgical plan remains strong.
What should I ask before choosing no shave surgery?
Ask exactly which areas will be shaved. Ask how large the shaved donor window will be and whether your existing hair can truly cover it. Ask whether the recipient area will be left long, trimmed, or partially prepared.
Ask how many grafts are realistic with this plan and whether the surgeon would recommend a different approach if privacy were not a concern. That question often reveals whether no shave surgery is being chosen for medical reasons or emotional reasons.
Ask who evaluates the donor area, who designs the hairline, who makes the recipient area openings, and who performs extraction. Who performs hair transplant surgery matters even more in no shave work, because this should not be treated as a simple cosmetic variation.
Ask what aftercare will be different. Washing, drying, photographing, and checking the scalp may require more instruction when long hair remains around the grafts.
Finally, ask what would make the clinic refuse a no shave plan. If the clinic has no clear answer, I would be careful.
How should I judge a clinic that promises an invisible transplant?
Be careful with any promise that makes no shave surgery sound simple for every patient. A clinic should explain which area will be shaved, how many grafts are realistic, how visibility will be managed, and whether the plan changes graft handling or procedure time.
When this is mainly about discretion, cost, or speed, the discussion is incomplete. The medical discussion should cover donor management, recipient area access, expected healing, aftercare, and what the patient may still notice after surgery.
I would be especially cautious if a clinic uses invisible surgery as a way to rush the booking. A patient who is anxious about privacy can be easy to pressure. The clinic should slow the decision down, not use embarrassment as a sales tool.
If you are comparing clinics abroad, the same principles in my guide to choosing a hair transplant clinic in Turkey apply here. The clinic should explain responsibility, donor limits, graft numbers, aftercare, and who will make the surgical decisions.
My final view is conservative. An unshaven hair transplant is reasonable only when discretion does not weaken the surgery. If shaving gives a safer, cleaner, more precise operation, I would rather protect the final result than protect the hairstyle for one week.


