- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 6 Minutes
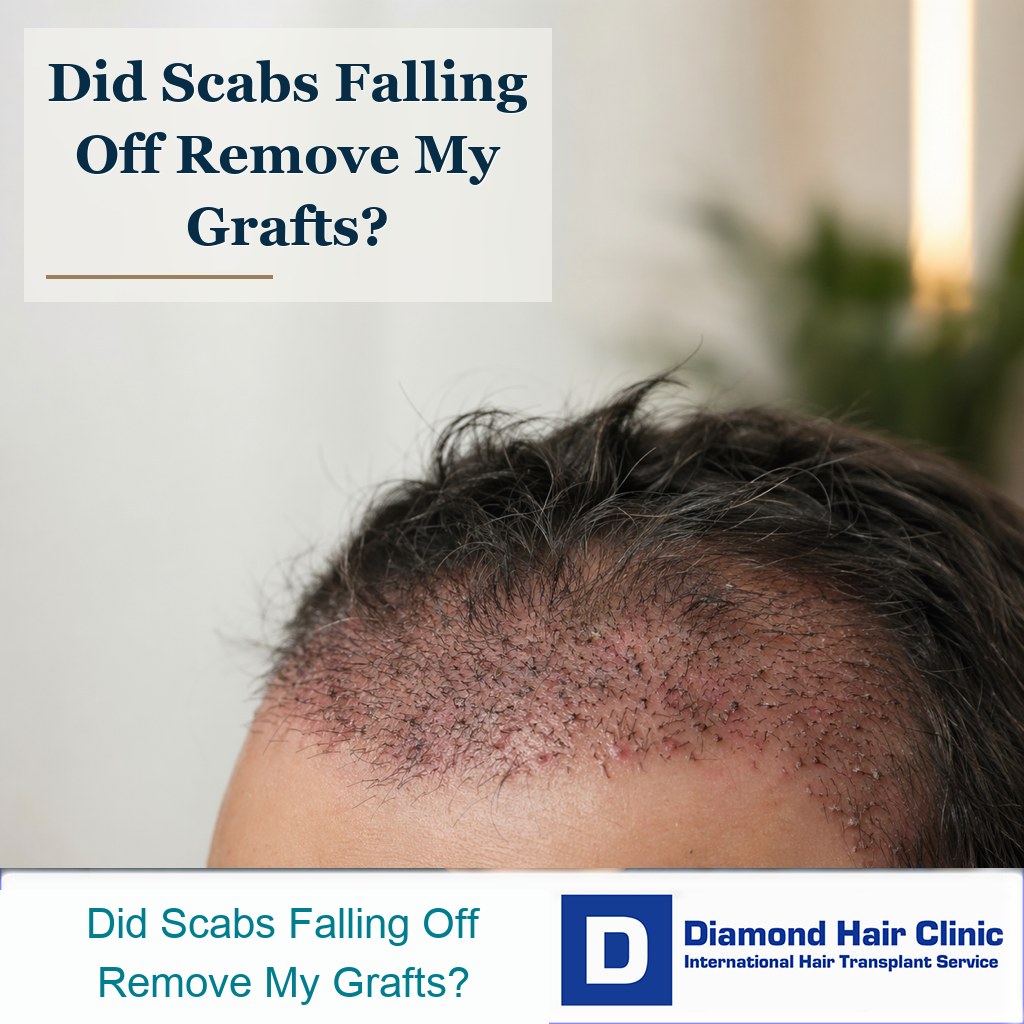
Scabs Came Off After Hair Transplant: Graft Loss or Normal Healing
In most cases, no. If a dry scab came off with a short hair inside it and there was no fresh bleeding, you probably did not lose the graft. The same distinction matters if hair comes out while you comb after the scalp has started to settle. The visible hair shaft can shed while the living follicle remains under the skin, and the recipient area can also look less dense after the first wash once scabs and shadow clear. Even the opposite pattern, no shedding after a hair transplant, can also be normal when the scalp is healing calmly.
Between days 10 and 14, this moment can frighten patients very quickly. You look at the sink, the towel, or your fingertips, and it can seem as if the surgery has come out with the scabs. But a hair shaft trapped in a dry crust is not the same as a living graft being pulled out.
Look at the event, not only the hair in the scab. Fresh bleeding, forced picking, increasing pain, and whether the skin underneath looks healthy matter more than the hair shaft itself. If the worry started after hitting or bumping the scalp, the timing and whether the spot opened also matter. The same calm judgment helps when the worry starts after sneezing or coughing.
At Diamond Hair Clinic, I treat this as part of hair transplant aftercare, because fear can make patients keep checking and touching the recipient area when the scalp mainly needs protection.
Hair in scabs often looks worse than it is
After FUE hair transplant surgery, tiny crusts form around the transplanted hairs. These crusts are made from dried serum, a little blood, and normal healing material from the skin.
As the scalp heals, those crusts loosen. The short hair shaft may be trapped inside the crust, so when the scab comes away, the hair may come with it.
Many patients think they are seeing grafts. Most of the time, they are seeing scab material and a hair shaft, not the living follicle itself.
The follicle sits deeper in the skin than the visible hair shaft. Once the graft has settled, the hair can shed while the follicle remains in place and prepares for the next growth cycle.
That separation matters because panic can lead to more touching. A patient sees one hair in a scab, checks another area, rubs a little more, then spends the whole day inspecting the scalp. That behavior can create more irritation than the scab itself. Scalp massage after a hair transplant needs to return only when crusts are ready and the clinic has allowed more pressure.
A truly lost graft usually bleeds and looks different
A truly dislodged graft is different from a dry scab with a hair attached. It usually happens earlier, when the graft has not yet anchored well, and it is often followed by fresh pinpoint bleeding from the recipient area.
If a graft is pulled out, you may see a small soft tissue piece, not just a dry flake. There is often bleeding because the graft has been removed from the small channel where it was placed.
A dry crust with a hair inside it, without fresh bleeding, is usually not a lost graft. The next step is not more rubbing or more testing. Stop, document the area once if needed, and ask the clinic if bleeding or symptoms are present.
If there is repeated bleeding, increasing pain, fluid under thick dark scabs, deep open areas, spreading redness, or skin that looks black, that is a different situation. Contact your clinic or a qualified doctor promptly.
Both sides matter. Real warning signs must not be ignored, but every fallen hair shaft must not be treated as a surgical disaster.

Grafts become more stable after the early days
The first few days are the most delicate. In this early period, the grafts must be protected from scratching, rubbing, pressure, and accidental trauma.
By the end of the first week, grafts are usually much more stable, but the scalp cannot be treated as completely normal. Healing is stronger, but the skin is still recovering.
Around day 10, many patients begin to remove crusts more actively, depending on the clinic instructions and how the scalp looks. This is also when many patients become anxious because more scabs and hairs appear to come away during washing.
There is a careful balance. Scabs must not remain so long that they irritate the scalp, but dry crusts must not be picked before they are ready.
The right timing depends on the surgery, the skin, the scab thickness, and the aftercare instructions. Do not copy another patient’s day exactly. Follow your clinic’s plan, and ask for review if the scalp does not look ready.

Rough scab removal needs calm documentation
First, stop rubbing and look calmly at what happened. If there is no fresh bleeding, no open wound, no increasing pain, and the skin looks calm, the situation is usually less serious than it feels in that moment.

If you rubbed too hard and a small area bled, send a clear photo to your clinic and explain exactly what happened. Do not keep testing the area to see whether more scabs will come off.
The mistake after rough rubbing is often the second reaction, not the first event. Patients become frightened, then they continue touching, washing again, applying extra products, or checking the area under harsh light.
If you are unsure, document the scalp once under steady light, then leave it alone while waiting for medical advice. Light fingertip movement during an instructed wash is different from dry rubbing, scratching, or repeatedly testing the same area. The plan needs to protect the healing environment, not solve fear with more handling.
Gentle washing matters when scabs are ready
Safe washing is patient and gentle. The plan needs to soften the scabs first, then allow them to loosen with controlled fingertip movement when your clinic says the time is right. If dryness is making crusts feel tight, saline spray after a hair transplant may be part of the clinic plan, but it must not lead to picking.

Do not use your nails. Do not scrape. Do not pick at one stubborn scab just because the surrounding scabs have already come off.
If a crust is ready, it usually loosens without force. If it stays attached, it may need more softening and another wash rather than more pressure.
Detailed washing advice matters here. The guide to washing after a hair transplant explains the difference between protecting the grafts early and gradually cleaning the scalp when the time is right.
Surgical planning also matters, but it does not replace aftercare. Precise recipient area work during Sapphire FUE hair transplant can support controlled healing, but even good surgery still needs careful washing afterward.
Scabs after day 10 or 14 need the right response
Some patients expect every scab to disappear on one exact day. Healing is not always that neat. A few remaining crusts can happen, especially if they are small, dry, and gradually loosening.
What concerns me is thick, hard, persistent scabbing that never softens, especially if it comes with redness, pain, discharge, or a bad smell. That needs proper review.
If scabs remain after the usual period, do not pick them out aggressively. Ask your clinic whether the scalp needs more soaking, a different washing rhythm, or direct assessment. The answer depends on how the skin looks.
Scabs that last longer can also make patients keep delaying proper cleaning. That can irritate the scalp. The scalp needs to become clean, but cleaning must not become a fight with the skin.
Hairs in scabs can be early shedding
Yes, sometimes the visible hair shaft begins to shed early, and this can happen while scabs are coming away. Do not read this as the follicle under the skin has failed.
Patients often imagine the transplanted hair as one solid object. In reality, the visible shaft and the living follicle are not the same thing. The shaft can detach and fall while the deeper part of the graft remains in the scalp.
Early shedding can look alarming and still be normal. A patient may see short hairs in the scabs, then see fewer visible hairs in the recipient area, and assume the transplant is disappearing. Quite often, the scalp is simply moving into the shedding phase.
The timing is not identical for every patient. Some keep more shafts for a while. Some shed earlier. Some scabs come off with tiny hairs attached. None of these patterns alone proves failure.
The stronger clues are bleeding, pain, unhealthy skin, or a clear traumatic event. Without those, hair in a scab is usually a reason to continue careful aftercare, not a reason to declare the transplant ruined.
Warning signs after scab removal need prompt review
Mild redness, tightness, and small crusts can be normal in the early healing period. A little sensitivity is also expected, especially when the scalp is dry.

What concerns me is a pattern that worsens instead of improving. Thick scabs that do not soften, yellow discharge, bad smell, expanding redness, strong pain, fever, or dark tissue that looks unhealthy need serious attention.
Deep holes, wet scabs, or increasing inflammation need medical assessment. Do not wait silently for weeks if the skin looks unhealthy.
If black scabbing, severe pain, spreading dark tissue, or open wounds appear, that is no longer a routine scab question. The concern shifts to urgent warning signs, including the problems explained in black scabbing after a hair transplant.
Here, surgeon involvement matters. A normal healing question and a real complication can look similar to a frightened patient, but they must not be managed with the same casual answer.
Clinic quality matters during early healing
The early healing period reveals a lot about the quality of the surgery and the quality of the follow-up. Patients need clear instructions, but they also need someone clinically responsible enough to judge when something is not normal.
In large volume clinics, patients may receive a standard message instead of a real medical review. The red flags of hair mill clinics matter even more when a patient needs someone to judge bleeding, scabs, pain, or unhealthy skin.
Hair transplantation is not only graft extraction and implantation. It is planning, tissue handling, recipient area creation, donor protection, post-operative instructions, and long-term responsibility.
A surgeon-led hair transplant clinic model matters here because small clinical decisions can affect both healing and final naturalness.
A patient who asks whether scabs came off safely deserves a precise answer. They must not receive a rushed message that ignores bleeding, timing, symptoms, washing routine, and the appearance of the skin.
Useful photos make review easier
If you are worried, send useful photos, not only the most frightening close-up. A single close photo can make every crust look dramatic and can hide the overall pattern.
Send one clear front photo, both oblique angles, the top if the area was treated, both sides, and a close photo of the exact area that worries you. The photo needs steady light, a dry scalp if possible, and no filters.
Also send the surgery date, the current day after surgery, what wash you performed, whether there was bleeding, whether there is pain, whether you used nails or strong rubbing, and whether the area is improving or worsening.
This information helps the clinic separate ordinary scab shedding from a true problem. It also prevents vague reassurance. A structured message once is more useful than twenty anxious photos without context.
If the clinic answers without looking carefully, ask again more clearly. A useful answer needs to address timing, bleeding, skin appearance, symptoms, and the washing routine.
Protect the result without obsessing over every hair
Follow your clinic instructions closely, especially for washing, sleeping, sun exposure, exercise, and touching the recipient area. Good aftercare does not mean constant inspection. It means controlled handling.
Then stop judging the result too early. Scab removal is not the final result, and early shedding is not failure. This recovery distinction is explained in more detail in hair shedding or permanent graft loss.
After that, look beyond the day 10 photo. A hair transplant needs to be based on donor supply, age, hair loss pattern, hair characteristics, and realistic expectations, not only on what the scalp looks like in one anxious close-up.
The question over the longer term is whether the patient is a good candidate for a hair transplant and how the donor area needs to be managed for the future.
If scabs came off with hairs but there was no fresh bleeding and the skin underneath looks calm, take a breath. In most cases, you have not ruined your transplant.
If there is bleeding, worsening pain, pus, deep wounds, or dark unhealthy skin, do not guess. Send clear photos to your clinic and ask for a proper medical review.
Protect the grafts carefully, but do not let every fallen hair become a crisis. A properly guided recovery is part of a stable long-term result.


