- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 14 Minutes

Sleep Position and Graft Safety During Recovery
Protect your sleeping position for the first 7 to 10 nights. Many patients can sleep more normally after day 10 if the grafts are stable, the scabs are settling, and the recipient area is not rubbing against the pillow.
During the early nights, sleep on the back with the head elevated about 45 degrees. The purpose is to protect the grafts from pressure, friction, and careless contact while swelling is still active.
Do not read this as a reason to panic over every small movement in bed. The rules are there to make sleep safer, not to turn every night into a test. A light accidental touch is different from rubbing, pressing, scratching, or sleeping directly on the grafted area. If you wake up worried that you bumped the grafts while sleeping, judge the event by timing, bleeding, and whether the skin opened. The same calm check helps if you woke up after coughing or sneezing. If the real problem is barely sleeping despite following position rules, sleepless nights after FUE explains when poor rest is harmless and when it needs help.
Sleep after hair transplant surgery is about more than whether a graft can be pulled out. Swelling, donor discomfort, pillow contact, neck support, and a practical first week setup all matter. If the question is specifically the first hotel night, use the first night after hair transplant plan alongside the broader sleep rules. Room comfort matters too. If you use a fan or air conditioning after hair transplant, keep the airflow indirect so dryness does not make you rub or scratch.
Sleeping position matters
Sleeping position matters for two reasons. Elevation helps limit swelling, especially after frontal work. Avoiding pressure and friction protects the recipient area while the grafts and surrounding skin are still settling. If you use ice after a hair transplant for swelling comfort, keep it away from the grafted area and do not sleep with it on the face.
Some people think only a dramatic accident can harm the grafts. In reality, repeated small friction can matter more than one tiny touch. A pillow, blanket, shirt collar, or restless hand can irritate the recipient area if you are careless while half asleep. If you already woke up worried, use the focused guide to sleeping on grafts after hair transplant before you start touching the area.
Sleeping elevated also helps with swelling after a hair transplant. After frontal hairline work, swelling can move downward toward the forehead and eyes. Elevation helps reduce that movement, especially in the first nights.
Sleep advice belongs inside good hair transplant aftercare, not as a separate ritual. It is part of protecting the surgical work while the scalp is still vulnerable.
Do not lie awake in fear. Arrange the bed in a way that makes the safe position easier before you are already tired. Good preparation is better than trying to control every movement after midnight.
Perfect stillness is not the goal. The practical distinction is between a light accidental touch and repeated rubbing, pressure, or scratching. Rubbing, pressure, and scratching are what sleep planning is trying to prevent. Sedating cannabis use after a hair transplant can matter if it makes sleep less controlled during those early nights.
Some people ask whether the donor area or the recipient area matters more during sleep. Both matter, but for different reasons. The recipient area is where the grafts need protection from friction, while the donor area may be tender and sensitive to pressure.
A safe sleeping setup respects both areas. It supports the head and neck, keeps the grafted area away from fabric, and avoids a position that makes the donor pain worse.
First night sleep position
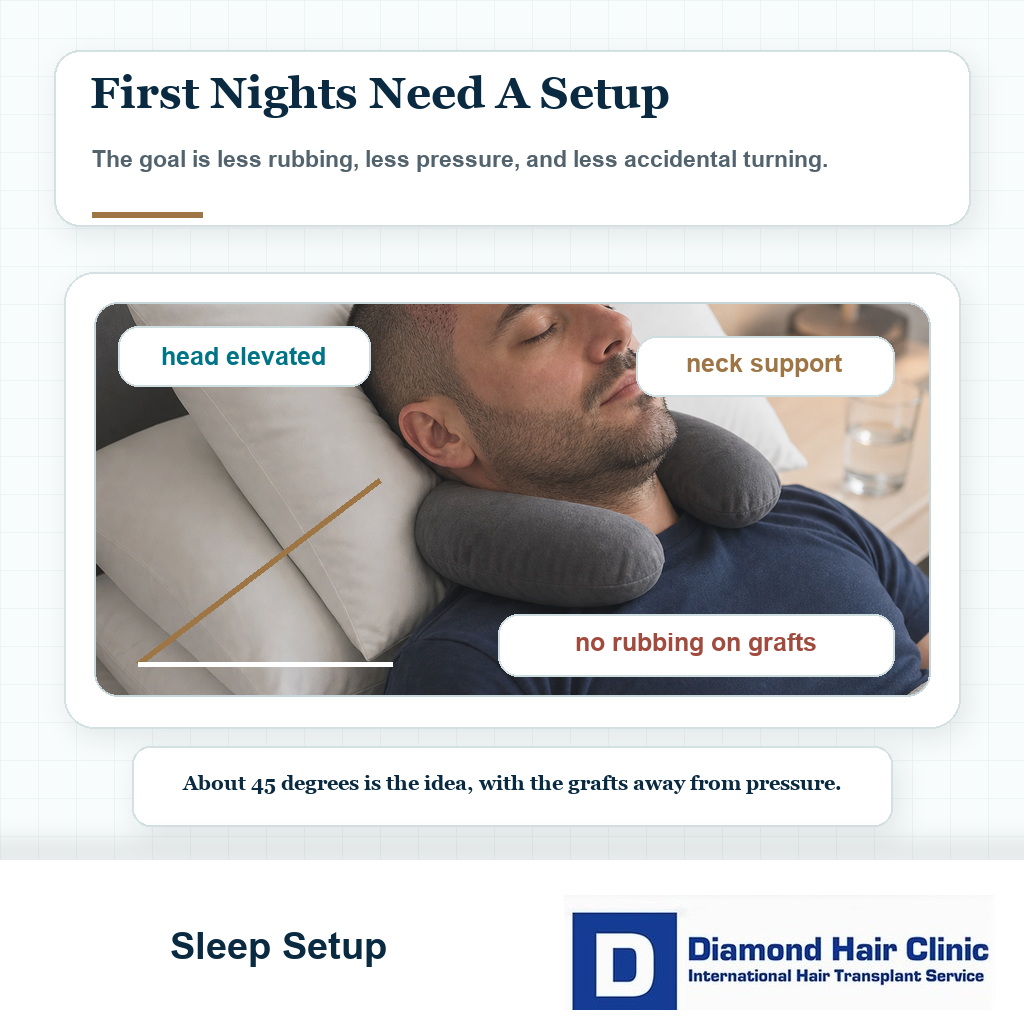
During the first night, sleep on the back with the head elevated about 45 degrees. A travel neck pillow can help keep the head stable and reduce accidental turning.
The first night is often the most awkward because you are tired, cautious, and aware of every sensation. Some donor tightness, mild discomfort, and fear of touching the grafts are common. Those sensations are not, by themselves, proof that something is wrong.
Prepare the bed before sleep. Keep the pillow arrangement simple. Avoid soft pillows that allow the head to sink and roll. Avoid sleeping face down or pressing the recipient area into the pillow.
If the transplant involved the hairline or frontal scalp, be especially careful not to let the front of the head touch bedding. If the crown was treated, the back of the scalp may also need protection from direct pressure.
I also advise against checking the scalp in the mirror all night. Anxiety after a hair transplant can make people touch, adjust, inspect, and move more. A prepared sleep setup protects the grafts better than constant checking.
If you wake up and find that your position changed slightly, do not panic immediately. Return to the safe position and examine the scalp only if there is bleeding, pain, or a clear sign of graft displacement.
Keep the first night boring. Do not experiment with new pillows, sleeping aids, or positions that you have never tried before. A simple arrangement that keeps you stable is better than a clever setup that becomes uncomfortable after one hour.
If someone is staying with you, explain the sleeping rules before bedtime. The helper does not need to watch you all night, but they need to understand that the recipient area must not be touched and that sudden adjustments can create unnecessary friction.
If sleeping on your back is difficult
Some people simply do not sleep well on their back. That is understandable. But during the first 7 to 10 nights, the priority is not your favorite sleeping position. The priority is keeping the recipient area away from pressure and rubbing.

If back sleeping is difficult, make the setup more practical before the first night. A firmer back support, a travel neck pillow, side pillows beside the shoulders, or a recliner style position can reduce the feeling that you may roll without control.
A slightly imperfect but stable protected position is better than an elaborate pillow tower that collapses after one hour. Stability matters more than trying to make the bed look medically perfect.
Short daytime rests can also help if the first nights are poor. Use them to get through the protected phase without repeated contact on the grafts, not to prove that sleep must feel normal immediately after surgery.
If you truly cannot maintain any safe position, share that with the clinic before surgery. Sleep habits are part of aftercare planning, especially for restless sleepers, people with neck problems, and anyone who already uses breathing support at night.
Graft safety while sleeping
Yes, grafts can be disturbed by strong rubbing, scraping, pressure, or direct trauma in the early days. But a light accidental touch does not always mean you have lost grafts.
The difference matters. A hair on the pillow can look frightening, but it is not always a destroyed graft. Very often, what you see is a hair shaft, dried crust, or normal early shedding, not a lost follicular unit.
A truly lost graft in the early period may be associated with bleeding or a small tissue like piece, not just a hair. Even then, a clear photo and clinic review are better than scratching, picking, or inspecting aggressively.
That distinction is part of lost grafts after hair transplant scabs. It matters because panic can make you do the exact thing you should avoid, which is touching the recipient area too much.
During sleep, the main risk is not a single hair on the pillow. The main risk is friction, pressure, or scratching during the period when the grafted area needs to be left alone.
If you are a restless sleeper, use physical prevention. A neck pillow, side pillows, and a slightly elevated position can reduce rolling. Do not rely only on willpower when you are asleep.
Timing for upright sleeping can stop
Many people can begin reducing strict upright sleeping after the first 7 to 10 nights if the scalp is healing well and their clinic has not given a different instruction. Do not make this decision only by calendar. Swelling, scabbing, tenderness, and the area treated all matter.
In this part of the decision, people often mix up two different ideas. A graft may become harder to dislodge before the scalp is ready for careless pillow pressure, repeated friction, or sleeping face down. Crusts and scabs also change the risk, because pulling on attached crust can be more dangerous than seeing a loose hair shaft.
If swelling has settled, scabs are stable, and the recipient area is not being rubbed, the sleeping position can become more relaxed. But relaxed does not mean careless. Still avoid direct pressure on the grafted area until healing is secure.
Some cases need longer. If the crown was treated, if there is unusual tenderness, if scabs are heavy, or if you move aggressively in sleep, staying cautious a little longer may be better.
The same logic appears in recovery planning for work. Many people need a protected first phase before social life feels normal again, and planning time off work after hair transplant around the visible healing period often helps.
Sleep should become easier each night. If it becomes harder because pain, swelling, or anxiety is increasing, that deserves clinic review rather than silent struggle. The same is true if poor sleep comes with cold or flu symptoms after a hair transplant, because fever and scalp symptoms need judgment together.
The fastest return is not always the best return. Match the sleep position to your actual healing.

Side sleeping after FUE
Side sleeping may be possible after the early protected phase, but it depends on which areas were treated and whether the recipient area touches the pillow. If the grafts are in the hairline, side sleeping may still be safer than face down sleeping, but the head can roll and create friction.

If the temples were treated, side sleeping can place the side recipient area near the pillow. If the crown was treated, the back of the head may be more vulnerable. The advice changes with the surgical map.
In the first 7 to 10 nights, avoid sleeping freely on the side unless your surgeon has specifically allowed it. After that, side sleeping can return gradually if there is no rubbing on the grafted area.
A neck pillow can still help even when you are no longer fully upright. It can limit sudden rotation and keep the scalp from sliding against fabric.
Think about the same principle I use when discussing hat after hair transplant. Anything that touches the grafted area must be judged by pressure and friction. A pillow is not different in that sense.
If side sleeping causes scabs to catch, recipient redness to worsen, or discomfort to increase, return to a safer position and ask your clinic for guidance.
Some people ask whether they can sleep slightly turned without fully lying on the side. A small angle can sometimes work after the highest risk period, as long as the grafted area does not touch the pillow. Change gradually rather than making a sudden return to old sleeping habits.
If you normally sleep face down, you need to plan for that before surgery. Face down sleeping is one of the riskiest positions in the early period because it can combine pressure, rubbing, and heat on the recipient area.
If this is your normal habit, treat the first week as a temporary medical position, not your permanent way of sleeping. The rule becomes easier when you see it as a short protected phase.
If you accidentally roll onto grafts
If you accidentally rolled onto your grafts, first stop and avoid checking with your fingers. Do not scratch, pick, or rub the area to check what happened. Sit up, look gently in good light, and ask the clinic to review it if you see bleeding, clear graft displacement, or unusual pain.
If there is no bleeding and no visible tissue displacement, a brief accidental contact may not cause harm. The scalp is delicate, but it is not made of glass. The real danger is repeated friction or a strong scrape.
Many people punish themselves emotionally after one sleeping mistake. That anxiety can become more harmful than the event because it leads to constant inspection. Report the concern clearly, then return to careful aftercare instead of checking the scalp again and again.
If there is a scab stuck to the pillow, do not pull on the scalp. Let washing instructions and clinic guidance manage scab softening. Pulling is more dangerous than the scab itself.
Healing signs can look alarming without always meaning graft loss, especially when judging redness, scabs, and pimples after hair transplant.
One accidental moment needs judgment by signs, not fear. Bleeding, pain, and clear displacement matter more than imagination.
It also helps to remember that you may not know what you saw. A hair shaft can look dramatic on a pillow because it is dark against white fabric. That does not prove that the follicle was pulled out.
If you are unsure, take one clear photo and stop touching the area. The clinic can guide you better from one steady photo than from repeated rubbing, lifting scabs, or trying to inspect every tiny spot with your fingers.

Sleeping with donor area soreness
Donor area discomfort can make sleep difficult, especially after FUE when the back of the scalp feels tight or tender. The challenge is to protect the recipient area while also avoiding too much pressure on the donor.

Elevation can help. A neck pillow can help. Taking prescribed medication exactly as instructed can also help. Do not add medications on your own without your clinic’s approval.
If donor pain is severe, worsening, on one side, burning, or associated with unusual swelling, the clinic should review it. Some discomfort is expected, but severe pain in the donor area after hair transplant belongs in a different category and should not be ignored.
For sleep, use support rather than pressure. A pillow needs to support the neck and head without pressing hard against fresh donor wounds. The position needs to feel stable, not forced.
If sleeping upright is causing neck strain, adjust the support gradually. The purpose is protected healing, not suffering through an impossible position.
Some people tolerate the first few nights better by changing support in small ways rather than abandoning the safe position completely. A slightly firmer neck pillow, a stable back pillow, or a cleaner angle can make a large difference.
Do not force yourself into severe discomfort and then sleep wildly from exhaustion. Recovery needs to be protective, but it also needs to be practical enough to follow. If you use CPAP or have sleep apnea, that practicality becomes part of the surgical plan before the first night.
Poor sleep and recovery
Poor sleep can make recovery feel harder. It can increase irritability, anxiety, pain sensitivity, and the urge to inspect the scalp repeatedly. It may not destroy grafts by itself, but it can make careful behavior harder.
Good sleep after surgery is not about luxury. It is part of practical recovery. When you sleep better, it is usually easier to follow instructions patiently and touch the scalp less.
Prepare the room before surgery if possible. Use clean pillow covers. Keep water nearby. Place the phone away from the bed if late night research makes anxiety worse. Make the safe position easy.
Avoid alcohol during early recovery if your clinic has advised against it, and do not use sleeping medication unless it has been approved. Being too sedated can increase careless movement or reduce awareness if you bump the scalp.
People often focus on products and forget behavior. In the first days, behavior matters. Controlled washing, careful sleep, avoiding friction, and not touching the recipient area are small but powerful parts of healing.
If poor sleep continues beyond the first week because of pain, swelling, or panic, share that with the clinic. Recovery should become progressively easier, not more chaotic.
To avoid before sleep
Before going to sleep, avoid anything that increases sweating, friction, bleeding risk, or careless movement. The night routine should be quiet and predictable. The more stimulated and uncomfortable you are, the harder it becomes to stay in a protected position.
Avoid heavy exercise after a hair transplant before bed in the early recovery period. Exercise can increase sweating and make the scalp feel more irritated. If you are unsure when to return to training, use the exercise article for activity timing and follow the wider aftercare rules from your clinic.
Avoid turning the night into a stimulant problem. One ordinary coffee earlier in the day is different from late caffeine, several espresso shots, energy drinks, or pre workout products that make you restless. The broader timing question is covered on the page about coffee after a hair transplant.
Avoid sexual activity in the very early period if it creates sweating, pressure, or accidental contact with the scalp. This is not moral advice. I am trying to protect the recipient area from friction and heat, which follows the same pressure and friction rule that applies to sex after hair transplant.
Avoid hot rooms when possible. Heat can increase sweating, swelling, and discomfort. If the weather is very warm, plan the room carefully and keep the bedding light, because a sweaty pillow can tempt you to rub or adjust the scalp repeatedly.
Season also matters for recovery comfort. Heat, sweating, sun exposure, and travel plans can change the practical experience after surgery, especially when judging hair transplant in summer or winter.
Avoid sleeping with pets or small children near the head in the first nights if there is any chance of accidental contact. This is practical, not dramatic. The first week is not the time to test your reflexes.
Avoid complicated pillow arrangements that collapse during the night. Two stable supports are usually better than five soft pillows that shift and make the neck uncomfortable.
Finally, avoid late night panic searching. The temptation is real, but it often makes you more anxious and less able to rest. If you have a real concern, take a clear photo in good light and ask the clinic to review the concern instead of reading frightening stories until morning.
Sleeping with less worry
Most people can sleep with much less worry after day 10, provided the recipient area is healing well, the scabs are controlled, and there has been no trauma. Do not read this as permission to scratch, rub, or sleep face down aggressively. It means the highest risk period has usually passed.
By this stage, you may feel more comfortable socially as well. The early swelling and fear begin to settle. The scalp still needs attention, but the recovery starts to feel more normal.
Caution can gradually soften as healing becomes stable. If you remain terrified every night after the first 10 days despite normal healing, speak with your clinic. Sometimes reassurance is part of good aftercare.
Do not confuse careful recovery with obsession. Obsession makes you inspect every hair and every scab. Careful recovery follows instructions and lets the body heal.
If you are using cosmetic products later to feel more confident, remember that timing matters. Early product use and friction should be handled cautiously, especially when judging hair fibers after hair transplant.
For most patients, the plan is clear. Protect your sleep position for the first 7 to 10 nights, avoid rubbing the recipient area, and return to normal sleep gradually when healing supports it.
After the first 10 days, still use common sense. If the scalp is irritated, if scabs remain unusually firm, or if the clinic has given specific instructions because of the case, follow those instructions instead of forcing the calendar.
Sleeping normally needs to feel like a gradual return, not a celebration that makes you careless. The best recovery is quiet. Nothing dramatic happens because you protect the scalp early and then slowly return to normal habits.
If you are unsure, ask your clinic with a clear photo rather than guessing. A clear question is always better than a nervous mistake made at midnight. Good sleep should support healing, not become another source of fear. That balance matters more than perfect stillness.


