- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 14 Minutes

Hat After Hair Transplant Pressure, Friction, and Timing
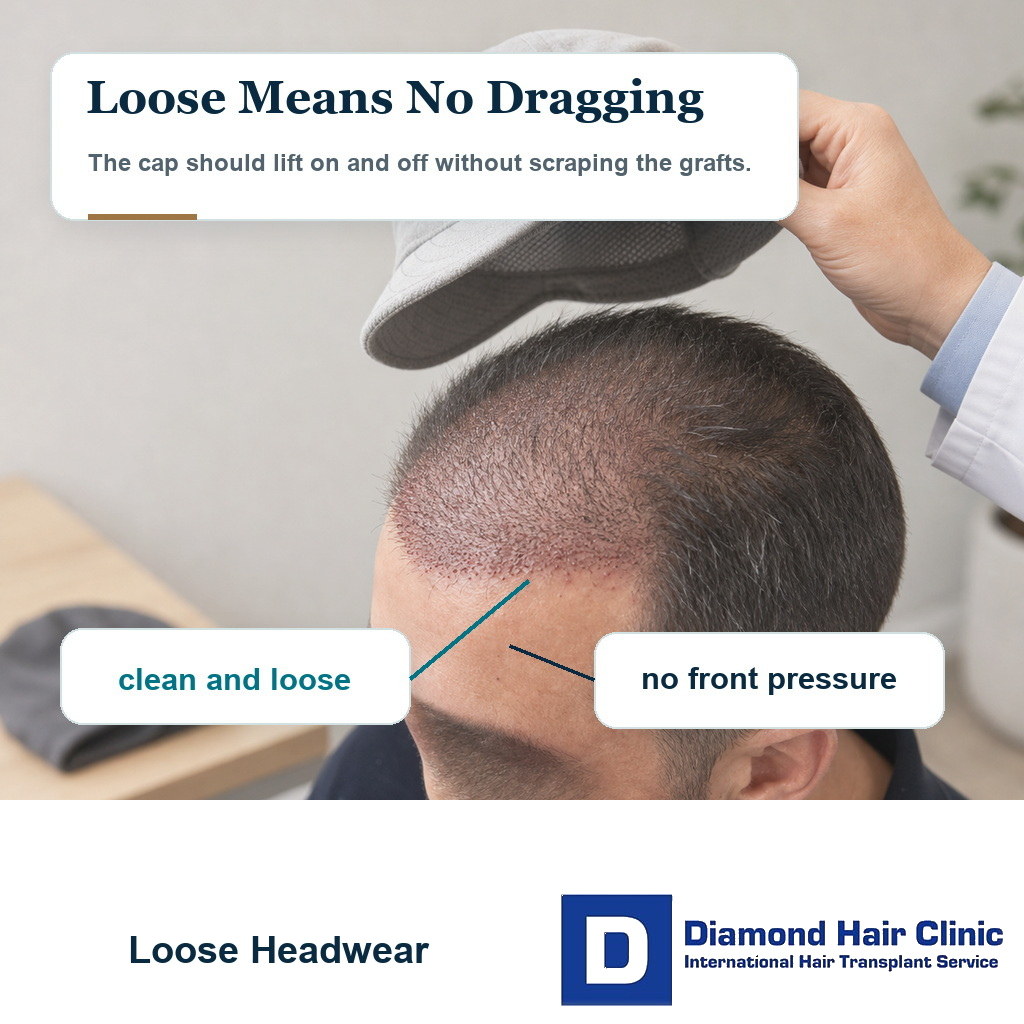
In most cases, I avoid headwear touching the recipient area during the first 10 days after a hair transplant. A loose, clean, breathable cap can often be considered between day 10 and day 14 if scabs are coming away normally, the scalp is dry, and the cap does not rub, press, or drag when you put it on or remove it. I use the same contact logic for clothing after a hair transplant. For choices such as bandanas, durags, and bucket hats, I judge soft headwear after transplant by pressure, movement, and cleanliness.
Tight caps and beanies need more time because they can pull across the grafted area and trap heat. Helmets and hard hats are a stricter category. I avoid a motorcycle helmet during the first 30 days, and in practical terms I usually prefer 4 to 5 weeks or longer. If the helmet is tight, if it must be worn for many hours, or if the scalp is still sensitive, 5 to 6 weeks is a safer mindset.
A bonded hair system needs even more caution than a loose hat because tape, glue, clips, and removal can all create friction on healing skin.
This question feels urgent because you are not only asking about something to wear on the head. You are asking how to return to work, protect the grafts, hide redness, avoid awkward conversations, and feel normal again after a hair transplant without damaging the result.
The answer depends on the type of headwear, the stage of healing, the treated area, the amount of scabbing, how long it will be worn, how much heat it traps, how much pressure it creates, whether the hat is being used for sun protection, and whether it is part of a beach after a hair transplant plan. The same recovery timeline behind hair transplant aftercare is the foundation for headwear decisions.
Early hats can disturb fragile grafts
Yes, headwear can damage grafts in the first days if it rubs, catches, presses, or pulls on the recipient area. The first days are not the time to test the scalp. The grafts are settling into tiny surgical openings, and the skin is still fragile.
A light touch is not the same as destroying grafts. One accidental brush is very different from repeated rubbing, pressure, scratching, or forcing headwear on and off. That practical distinction matters because panic can make people keep checking and touching the same area.
The risk is mechanical. A tight edge can scrape the hairline. A cap can catch on scabs. A beanie can drag across grafts when removed. A helmet can press on the recipient area and the donor area at the same time.
During the first 10 days, think mechanically. Anything that touches the grafted area can become a source of friction. That includes hats, pillows after a hair transplant, towels, car ceilings, shirt collars, glasses or sunglasses after a hair transplant, headphones after a hair transplant, and even your own fingers.
For the same reason, I pay close attention to aggressive scalp checking. Anxiety can turn one careful moment into repeated lifting, adjusting, replacing, and inspecting. That repeated contact is often more risky than the first brief touch.
If scabs come away with hairs inside them, people often panic and think they pulled grafts out. A hair shaft inside a dry crust is not always a lost follicle. That also matters for lost grafts after a hair transplant. Still, do not test this by wearing something too early.
The early rule is clear. If the recipient area still has fresh scabs, wet crusts, bleeding spots, tenderness, or fragile skin, do not cover it with ordinary headwear. Protection matters more than appearance in this early window.

Accidental contact needs calm triage
If a loose hat touched the grafts briefly and there is no bleeding, no pain, no visible tissue attached to the hat, and no new open spot, do not immediately assume the transplant is ruined. Most serious problems come from pressure, rubbing, dragging, or repeated contact.

The right response is to look once, document it if needed, and then leave the area alone. Do not keep lifting the hat and checking the same spot again and again. Do not scratch, pick, or try to test whether the grafts are secure. Take clear photos if you are worried and send them to your clinic.
If there is bleeding, a clear open gap, increasing pain, discharge, or a piece of tissue that looks like a graft, the situation needs review. If the contact was brief and the scalp looks unchanged, the answer is to stop wearing the hat for now and return to careful aftercare.
One accidental touch is different from deciding to wear the wrong hat all day. The first may only create anxiety. The second can create avoidable friction, heat, and pressure.
Safer headwear after day 10 to day 14
After the first 10 to 14 days, the safest option is loose, clean, breathable, and easy to put on without dragging across the grafted area. It needs to sit lightly and must not compress the hairline, temples, crown, or donor area.
The safer choice has enough internal space so the fabric does not rub the recipient area when you move. A very soft, loose cap can be safer than a structured cap with a tight front panel. A hat that looks stylish but grips the scalp is not a good choice.
Test the movement before leaving home. Put it on slowly. Remove it slowly. Try it for a short quiet period first, not for the first time during a full workday or commute. If it catches on scabs, pulls at hairs, creates pain, leaves a pressure mark, or makes the scalp feel hot and wet, it is too early or it is the wrong choice.
Cleanliness matters. Any cap worn during commuting, gym use, outdoor sweating, or daily work can hold oil, dust, and bacteria. I avoid that sitting over healing skin. If you must wear one, use it freshly cleaned and for short periods at first. If the concern is rain after a hair transplant, an umbrella is usually safer than tight wet fabric.
Breathability also matters. A thick cap that traps heat can make the scalp sweat. Sweat itself does not always destroy grafts, but heat, moisture, itching, and friction together can make you scratch. That is the pattern to avoid.
Do not reduce this to whether headwear looks normal with smart clothing. The decision depends on whether it behaves gently on healing tissue. It can look professional and still be wrong for the scalp.
If you had a crown hair transplant, caps that touch the top and back of the head need special planning. If the frontal hairline was treated, the front edge matters. If temple work was done, side pressure matters more than many people realize.
Bonded hair systems create a different risk
A bonded hair system is not in the same category as a loose hat. A loose hat may be used briefly in specific cases after enough early healing, but glue, tape, adhesive, clips, solvents, and repeated removal create a different level of risk.

With a loose hat, the main concern is pressure and friction. With a bonded hair system, I also worry about adhesive irritation, trapped sweat, poor ventilation, cleaning products, scalp pulling during removal, and the tendency to keep the scalp covered for long periods.
A hair system after a hair transplant needs much more caution than a simple loose cap. A loose cap can be removed without glue and without pulling on the scalp. A bonded system often involves repeated attachment and removal, which can irritate healing skin.
If direct scalp attachment is involved, think in terms of at least 90 days, and often longer if the scalp is red, sensitive, itchy, irritated, or not completely settled. Do not treat the hair system timeline as if it were the same as the loose cap timeline.
Allowed after a certain point does not always mean ideal for the best possible result. The aim goes beyond protecting grafts from being pulled out. The scalp also needs to stay healthy during the months when the transplanted follicles are recovering and preparing for growth.
Office return needs a practical social plan
If you need to return to an office, plan the social part of recovery before you book a hair transplant, not after. For many people, being away from in person work for 10 to 12 days is more comfortable if it is possible. That timing matches the period when scabs, swelling, washing, and visibility are most obvious.
Some people can work from home after 2 or 3 days because they are not meeting people and they can rest between tasks. That is very different from commuting, sitting under bright lights, wearing headwear all day, and feeling watched. Safety and social comfort are not the same question.
My guide on time off work after a hair transplant goes into this in more detail, because many people underestimate the emotional side of returning too quickly. They may feel physically fine but socially exposed.
If you ask me what to wear with formal clothing, I first ask whether headwear will actually reduce attention. In some offices, a cap is more noticeable than a shaved scalp. People may ask about the cap simply because you never wore one before.
A shorter leave, remote work, a simple explanation, or accepting a temporary buzzed look may be safer than forcing headwear too early. It is not worth risking grafts just to avoid one awkward week.
Another practical issue is repeated adjustment. If you return too early and spend all day lifting, tightening, and checking a cap, you may become more anxious, not less. A healing scalp needs quiet behavior. Constant hiding often creates the opposite.
For office return, the rule is practical. If the office allows a very loose clean cap after day 10 to day 14, the scalp is dry, scabs are mostly clear, and the cap does not touch the recipient area aggressively, it may be acceptable for short periods. Wearing that same cap for 8 or 10 hours is a different decision because heat, pressure, and repeated adjustment build up over time.
Beanies and tight caps need more time
A tight beanie or tight cap is often a poor choice in the early recovery period. The difficulty is pressure while it is on and rubbing when it is pulled over the scalp and removed.
A beanie can drag across the recipient area, especially if the fabric is elastic. It can also make the scalp warmer and more humid. Warmth and friction can increase itching, and itching makes people touch the grafts more often.
Many people want a beanie during the ugly duckling phase because it hides shedding, redness, and uneven growth after a hair transplant. That feeling is understandable. The ugly duckling phase can be emotionally uncomfortable, even when healing is normal.
The issue is timing. By month 2 or month 3, the concern is less about pulling grafts out and more about irritation, appearance, and anxiety. At that stage, the grafts are not sitting loosely on the surface, but the skin can still be sensitive, and you may still be judging every change too harshly.
The headwear question often connects with the way people handle the ugly duckling phase after hair transplant. A cover can help emotionally, but it should not become a reason to ignore healing signals.
If you use a beanie later in recovery, keep it loose, clean, soft, and careful. Do not pull it tightly over the frontal hairline. Do not let it create sweating. Do not wear it all day if the scalp becomes irritated.
Short, careful use after the grafts are secure and the scalp has settled is very different from a tight beanie during the first week. The first week is the wrong time to experiment.
Helmets and hard hats are stricter
A helmet or hard hat is not the same as a loose cap. I give more time before returning to anything that creates pressure, repeated contact, heat, sweat, or vibration.
For a motorcycle helmet, I avoid use during the first 30 days. In real life, 4 to 5 weeks is a safer minimum, and if the helmet is tight or prolonged wear is expected, closer to 5 to 6 weeks is more sensible.
A construction hard hat may sometimes be more forgiving than a motorcycle helmet if it has internal space and does not press directly on the recipient area. But still do not rush hard hat use too early, especially if the work environment is hot, dusty, physically demanding, or involves sweating.
This matters for construction workers, motorcyclists, cyclists, police officers, military personnel, warehouse workers, and anyone whose job requires protective headgear. A helmet can press on the recipient area, rub the donor area, and create heat during long use.
If your job legally requires a hard hat, do not solve that problem by wearing it too early and hoping nothing happens. Plan time away from that duty before surgery, or arrange modified work if possible. This is part of responsible surgical planning.
Clarify this before surgery if you must wear a helmet or hard hat at work. It may affect the surgery date, the recovery plan, the amount of time off, and sometimes whether surgery needs to be delayed until you can protect the result properly.
A motorcycle helmet is more demanding because it is tight by design. It moves with the head, creates pressure, and may rub when removed. I avoid that over a freshly grafted scalp.
The donor area also matters. If the donor area is tender, swollen, painful, numb, or irritated, a helmet can make recovery more uncomfortable. If donor discomfort is stronger than expected, compare your symptoms with the guidance I give about donor area pain after hair transplant and speak with your own surgeon if symptoms are increasing.
If pressure, heat, pain, rubbing, bleeding, discharge, or increasing redness appears after wearing headwear, stop and ask for clinic review.
For helmets and hard hats, keep the rule strict. If protective headgear is required, do not rely on a general internet answer. Ask your surgeon to review your scalp first. The wrong pressure at the wrong time is not worth the convenience of returning a few days earlier.

Heat, sweat, and dirty fabric can irritate healing skin
A hat can increase sweating, pimples, irritation, or infection risk if it is dirty, tight, hot, or worn too long over healing skin. This is not meant to frighten you. The scalp after surgery is not ordinary skin for the first stage of recovery.

The recipient area has thousands of tiny openings. The donor area has extraction points. The skin barrier is healing. In this stage, anything that adds heat, moisture, and friction can make the scalp more reactive.
Small pimples can happen after hair transplant surgery. Mild redness and itching can also happen. But a tight unwashed cap worn all day can turn heat and itch into a preventable problem.
My guide to redness, scabs, and pimples after a hair transplant explains warning signs more fully. For headwear, keep the rule practical. Do not trap a healing scalp under heat and pressure if it is already irritated.
If the scalp becomes more red after wearing headwear, stop wearing it and observe the trend. If there is increasing pain, warmth, discharge, bad smell, spreading redness, fever, or thick painful crusting, contact your clinic or a qualified doctor. Do not try to hide those signs under a cap.
Some people use fibers, sprays, powders, or concealers under headwear. That combination needs extra caution in the early period. The scalp is already healing. It does not need cosmetic products, sweat, pressure, and repeated washing all competing with the recovery process.
A cleaner routine is usually better. Let the scalp breathe when you can. Use a loose clean cap only when needed. Remove it gently. Follow the washing protocol your clinic gave you. Do not scratch.
Use headwear for cover only when it is safe
Yes, later in recovery, headwear can help hide shedding and redness when used carefully. But it cannot become your main recovery strategy. If you plan your whole emotional comfort around hiding, the process can become harder than it needs to be.
Shedding is expected after many hair transplants. The visible hairs may fall, while the follicles remain under the skin and later produce new growth. This can make the transplant feel as if it is disappearing, even when the biology is moving normally.
Redness can also last longer than expected. Skin type, density, healing speed, sun exposure after a hair transplant, inflammation, and previous scalp sensitivity all play a role. Some patients look socially normal sooner. Others remain pink for weeks or longer.
A cap may help you get through a social event, a short errand, or a commute. But if you are using it because you are panicking about shedding, reassurance and clinical guidance may help more than cover.
People sometimes also confuse shedding of transplanted hairs with thinning of surrounding native hair. If the native hair looks weaker after surgery, the issue may be shock loss after a hair transplant, ongoing miniaturization, or lighting, not simply the headwear.
Balance matters here. Use headwear when it is safe and useful, but do not judge your result by how much you feel you need to hide at month 1, month 2, or month 3. Those months are often emotionally noisy.
Hiding must never create more risk than the problem it is trying to solve. If it is making you sweat, scratch, or obsess, it is not helping.
Sun protection should start with shade
Sun protection matters after a hair transplant, but early sun protection cannot mean pressing a tight covering onto the grafts. If the plan involves sunbeds after FUE rather than shade, the UV decision needs separate caution. In the first phase, the best protection is avoiding direct sun, choosing shade, limiting outdoor exposure, and planning the day intelligently.
Freshly treated scalp can be more sensitive to sun. Redness can become more visible. Heat can increase sweating. Sweating can increase itching. Itching can lead to touching, and touching is the behavior to avoid in the early phase.
If you had surgery during a hot season, this planning becomes even more necessary. Heat, travel, sweating, and seasonal timing can change the practical recovery experience, which is why the timing question matters in hair transplant in summer or winter.
During the first 10 days, it is better to avoid situations that require headwear instead of forcing a hat to solve the problem. Do not schedule long walks under strong sun. Do not sit outdoors for hours. Do not test sunscreen or cosmetic products on a fresh recipient area unless your surgeon has approved it.
After day 10 to day 14, if healing is clean and the cap is loose, short periods of careful use may be reasonable. But sun protection still means moderation. A loose cap is not permission to spend hours in heat while the scalp is still settling.
If you are traveling, think about airports and security after a hair transplant, queues, hotel transfers, and outdoor sightseeing. A hair transplant trip is not a normal holiday. Do not treat the scalp like a finished cosmetic result during the first days.
If you want to visit Istanbul after surgery, quiet indoor plans, shade, and low stress movement are better. The grafts deserve quiet healing more than photographs, tours, or proving that everything is already normal.
Surgeon review before normal headwear
Before normal headwear, I assess whether the recipient area is dry, whether scabs have cleared appropriately, whether there is active redness or discharge, whether the donor area is comfortable, and whether the planned headwear creates pressure. Photos can help, but sometimes direct examination is better.
The exact type of headwear matters. A loose cap for a short walk is not the same as a tight motorcycle helmet for daily commuting. A soft surgical cap is not the same as a wool beanie. A hard hat at work is not the same as a clean loose hat at home.
Surgeon led follow up matters here. Headwear advice cannot be a generic line handed to everyone. It needs to reflect the treated area, graft count, skin condition, donor tenderness, job requirements, and healing speed.
If a clinic cannot answer who is responsible for aftercare decisions, that is a problem. The same person who understands the surgical plan also needs to understand why one person can return to loose headwear sooner while another needs more time. That responsibility is part of who actually performs your hair transplant.
The practical guidance is clear. Avoid headwear touching the recipient area for the first 10 days. Consider only a loose, clean, breathable cap between day 10 and day 14 if healing is settled. Delay tight caps and beanies until the scalp is clearly stronger. Treat helmets and hard hats more strictly, especially motorcycle helmets, which I avoid during the first 30 days and prefer after 4 to 5 weeks or longer.
If wearing headwear creates pressure, heat, pain, rubbing, bleeding, discharge, or repeated anxiety, that is a sign the headwear is not right yet. Stop, let the scalp heal, and ask your surgeon.
The surgical result is created in the operating room, but it is protected by small decisions afterward. Headwear is one of those decisions. Handle it patiently, and the first weeks become safer.


