- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 5 Minutes
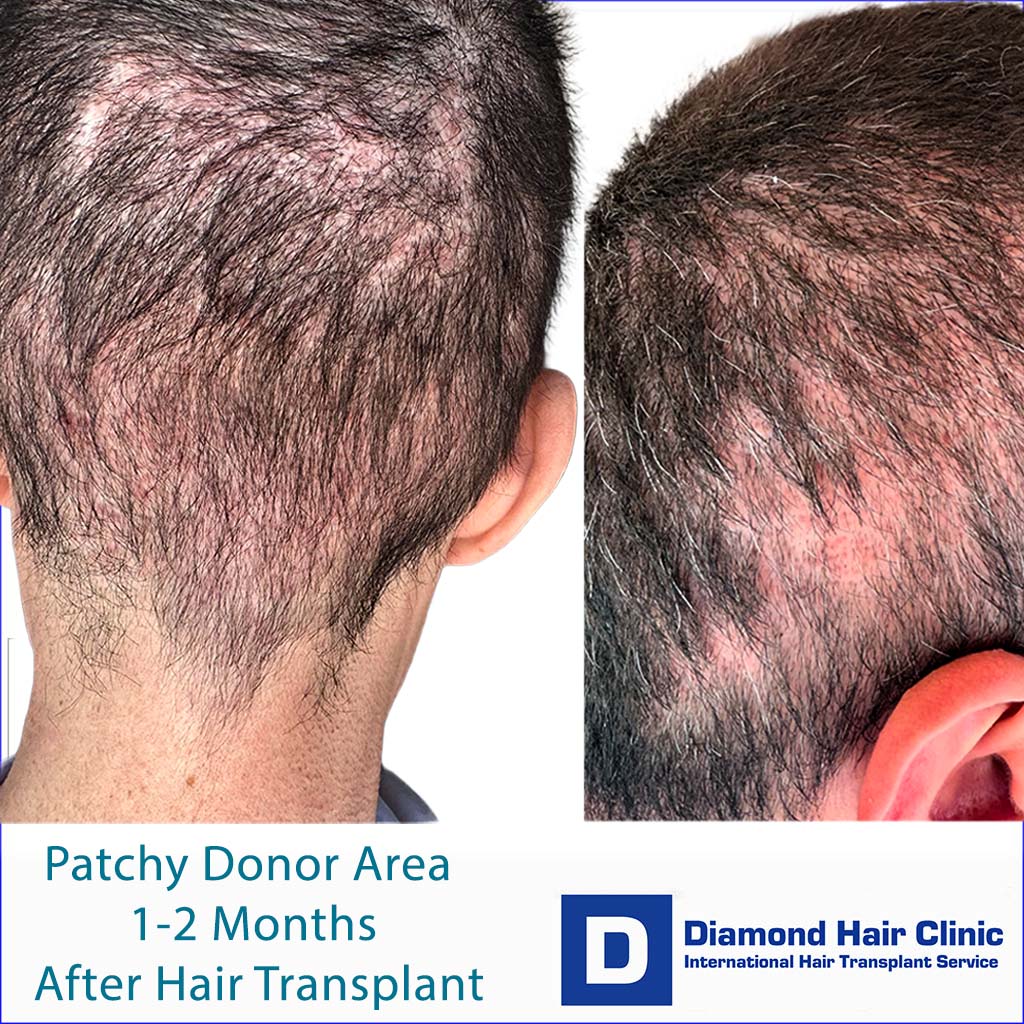
Does the Donor Area Look Normal One or Two Months After FUE?
A donor area can look patchy, red, uneven, or thinner at one or two months after FUE hair transplant and still be healing normally. I become more concerned when the pattern is sharply depleted, the symptoms are getting worse, the hair has grown but the area still looks see through, or the extraction looks concentrated in one zone instead of evenly distributed.
This is the responsible answer I give patients who send anxious donor photos. One close photo under bright bathroom light cannot diagnose the donor area by itself. But it can show whether the case deserves calmer monitoring, better photos, or direct medical review.
The donor area is not a secondary detail. It is the limited hair reserve that makes the whole surgery possible. A good result depends not only on the front hairline, but also on whether the donor area was used with judgment.
What can still look normal after one or two months?
At one or two months, the donor area may still show mild redness, tenderness, small dot marks, uneven density, temporary thinning, or a patchy look when the hair is very short. This can be frightening because patients usually inspect the area much more closely after surgery than they ever did before.

The most reassuring sign is improvement. If the redness is fading, tenderness is settling, the surrounding hair is growing, and the area looks less obvious month by month, I am usually calmer. Healing is judged by direction, not only by one day.
A donor area can also look worse than it really is when the hair is cut very short. The contrast between skin, scar dots, redness, and short dark hair can exaggerate every small difference. The timing of your first haircut after a hair transplant matters.
Normal healing does not mean the donor area must already look perfect. It means the appearance makes sense for the time point and is moving in the right direction.
Why can the donor area look patchy during healing?
Patchiness can come from several different causes. Short hair length is one. Redness is another. Temporary shock loss around the extraction points can also make the donor look thinner than it will later look.
There is also a natural difference in density between the back and the sides of the scalp. When grafts are taken, those differences become easier to see, especially in harsh light. A patient with pale skin and dark hair may see more contrast than a patient whose hair and skin color are closer together.
But patchiness can also come from poor extraction. If grafts are taken too close together, if one zone is emptied while other areas are barely touched, or if extraction moves outside the reliable safe donor area, the problem may be more than temporary healing. I do not judge only the word patchy. I judge the pattern.
How can I tell shock loss from overharvesting?
Shock loss after a hair transplant means nearby hairs weaken or shed temporarily after surgical stress. It can happen around the recipient area, and it can also affect the donor region. If the follicles are not permanently damaged, the area may improve as the scalp calms and the hair cycle recovers.
Overharvesting is different. In true donor area overharvesting, too much hair has been removed from the donor reserve or extracted in a poor pattern. Removed follicular units do not grow back in the donor as if nothing happened.
The distinction is not always obvious at one month. Shock loss can mimic damage. Short hair can exaggerate extraction marks. Redness can make the scalp look more exposed. I usually compare standardized photos over time before calling a donor area permanently damaged.
Still, the clinic should not hide every concern behind the word shock loss. If the extraction map looks obviously concentrated, if the donor looks carved out, or if the graft number was pushed beyond what the donor could safely support, the patient deserves a more serious answer.
Which warning signs should be checked quickly?
Some signs are not only cosmetic. Increasing pain, spreading hot redness, pus, bad smell, worsening swelling, bleeding, fever, or skin that is turning dark, grey, or unusually wet should be checked quickly. These signs can suggest infection, irritation, poor healing, or another medical problem.
If you have severe donor area pain after a hair transplant, do not treat it as a normal photo concern. Pain that is sharp, increasing, or disturbing sleep needs different attention from simple patchiness in a photo.
The same is true when redness, scabs, or pimples are getting worse instead of settling. Mild surface changes can be normal, but spreading inflammation deserves careful follow up. The redness, scabs, and pimples after hair transplant page explains those warning signs in more detail.
How does extraction pattern change the answer?
Extraction pattern is an important details. A well planned FUE extraction should be distributed carefully across the safe donor area. It should not create obvious empty corridors or take too much from one region just to reach an impressive graft number.
When I look at a donor area, I ask whether the harvesting looks balanced. I compare the back and sides. I look at whether the lower neck or unstable areas were used too aggressively. I also consider the number of grafts and the original density of the patient.
Graft numbers must never be separated from donor planning. A plan that sounds attractive in the recipient area can be harmful if the donor cannot safely support it. How a surgeon calculates graft numbers explains this relationship more fully.
Good donor management is not simply taking fewer grafts. It is taking the right grafts from the right zones in a pattern that preserves future options.
Why does hair length and lighting matter so much?
Hair length changes the donor appearance dramatically. A donor area seen at a few millimeters can look much more open than the same area seen with longer hair. This should be understood more narrowly the patient is imagining the concern. It means the visual test is very unforgiving.
Lighting also matters. Flash, bathroom mirrors, wet hair, close phone angles, and overhead light can make the donor look emptier than it appears in daily life. Clinic result photos are often taken with controlled light and a flattering hair length, so comparing them with a panic photo at home is not fair.
I prefer responsible photography. Dry hair, normal room light, the same distance, the same angles, and monthly comparison. A useful photo should help the decision. It should not create more confusion.
When should I send photos to the clinic?
You should send photos if the donor area is getting worse, if pain or redness is increasing, if the pattern looks sharply depleted, or if your anxiety is strong enough that you cannot judge the situation calmly. Asking for review is reasonable. Guessing alone is not helpful.

Send photos from the back, both sides, and slight angles. Keep the hair dry. Use consistent lighting. Do not press the camera against the scalp. Add the surgery date, graft number if you know it, medications, symptoms, and whether the appearance is improving or worsening.
Good follow up depends on good information. A clinic cannot responsibly judge the donor from one unclear close photo. But with proper photos and timing, the surgeon can usually separate a normal healing concern from a case that needs closer attention.
How long should I wait before judging the final donor area?
I usually avoid final donor judgment at one or two months unless there is an obvious medical problem or a very abnormal extraction pattern. Many temporary donor changes are easier to interpret between three and six months, and the cosmetic impression can continue changing as the hair grows longer.
At three months, redness is often calmer and some shock related thinning may begin to recover. At six months, the picture is usually more meaningful. Even then, hairstyle, hair caliber, skin contrast, and the amount of extracted grafts still affect the final look.
If the donor remains visibly see through after the hair has grown, the conversation becomes more serious. At that point I would review the extraction pattern, preoperative donor density, graft number, punch size, scarring, and whether the patient had naturally weak donor hair before surgery.
Can minoxidil or supplements repair the donor area?
Minoxidil, supplements, and supportive treatments should not be presented as a guaranteed repair for donor damage. If the issue is temporary shedding or inflammation, time and proper scalp management may already bring improvement. If the issue is true overharvesting, no tablet or topical product can replace follicles that were removed.
Sometimes medical support may help surrounding native hair look stronger, especially if the patient has diffuse thinning or miniaturization. But this is different from repairing a depleted donor zone.
I prefer to be clear with patients. Support can help the scalp and existing hair in selected cases, but donor protection must happen during the first surgery. Prevention is much stronger than rescue.
What should I avoid while the donor area is healing?
Avoid aggressive scratching, harsh brushing, early close shaving, strong chemical products, and daily inspection under harsh light. These habits usually increase anxiety and can irritate the scalp.
Follow the clinic instructions for washing and normal hair transplant aftercare. If the scalp is itchy or tender, do not start random products because someone online suggested them. Irritation from products can confuse the healing picture and make a normal donor look worse.
If you are worried about ingredients, the safer approach is to keep products simple and follow medical instructions. Harmful ingredients in hair products explains why the early healing scalp should not be treated like normal skin.
What if the donor area was truly overharvested?
If the donor area was truly overharvested, the discussion must be responsible. The goal is usually camouflage, blending, or damage limitation, not a perfect return to the original donor.
Options may include growing the hair longer, changing the haircut, scalp micropigmentation in selected cases, medical support for surrounding hair, or very careful grafting into visible depleted zones in rare situations. Each option has limits. A damaged donor is difficult to repair because the donor itself is the resource normally used for repair.
I am strict about donor management. Overharvested donor area repair can sometimes improve the look, but it is not a reason to accept careless harvesting in the first place.
How do I judge whether the original clinic protected my donor area?
Ask whether the clinic measured your donor capacity, explained the safe donor area, documented the graft number, distributed extraction evenly, and planned for future hair loss. A clinic that only talks about how many grafts it can take may be missing the more important question.
High volume clinic models can create donor problems when the surgery is treated like production work rather than patient specific planning. The danger is not only a weak result in the recipient area. The danger is losing donor reserve that may be needed later.
If you are comparing clinics for a future procedure, look carefully at how they speak about the donor area. The consultation should explain limits, not only promise density. This is part of how to choose a hair transplant clinic in Turkey.
What is the safest practical next step?
If your donor area looks uneven at one or two months, do not jump immediately to the worst conclusion. Take standardized photos, watch the trend, avoid irritating the scalp, and ask your clinic for a calm review.
If the area is improving, time may be the correct medicine. If the pain, redness, swelling, or discharge is worsening, get medical review quickly. If the extraction pattern looks clearly abnormal, ask for a proper explanation instead of accepting a vague reassurance.
The donor area is your long term hair reserve. It deserves the same seriousness as the transplanted hairline. A normal healing donor should keep improving. A damaged donor should be recognized early enough for the patient to make safer decisions from that point forward.


