- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 6 Minutes

Recently, a hair transplant patient contacted Diamond Hair Clinic via WhatsApp seeking advice about severe pain in his donor area following surgery. A few days earlier, he had undergone an FUE (Follicular Unit Extraction) procedure at another clinic in Turkey, not at our clinic. He was unhappy with the quality of the surgery and concerned that no doctor was present during the procedure. As a result, he had many doubts about both the operation and the potential results. Unfortunately, by choosing a hair mill clinic for such an important procedure, he did not make the best decision, nevertheless, we provided him with information and guidance regarding his condition.
I had fue hair transplant four days ago, since yesterday, I’ve been experiencing extremely sharp pain whenever the back of my head makes contact with anything, even something as soft as a pillow or the headrest of a chair. Donor area feels very tender and hypersensitive, almost like a nerve-pinching or electric shock sensation, and pain tends to linger for several minutes after the contact stops. There’s no visible bleeding or discharge, but the area feels tight, slightly swollen, and very sore to the touch. I’ve been trying to follow all the aftercare instructions carefully, sleeping upright at about a 45 degree angle, using a travel neck pillow to avoid direct pressure, and taking medications, but last night was especially difficult because even minor shifts in position triggered that sharp discomfort. I expected some soreness, but this level of pain feels more intense than I anticipated. Is this degree of sensitivity and sharp pain in the donor area normal at this stage of recovery?
Is This Degree of Sensitivity and Sharp Pain in Donor Area Normal After FUE?
This is actually a very good question, because many patients read online that recovery after FUE is “easy” or “mild,” and then they become alarmed when their own experience feels stronger than expected.
Some donor area pain, tenderness, burning, numbness, and pressure sensitivity can absolutely be normal after FUE. But if the pain is truly severe, I would not ignore it, and I would want the patient to update the clinic.
That does not automatically mean something is wrong. It simply means the symptom deserves proper interpretation, not guesswork. FUE complications describe early postoperative pain, altered sensation, hyperesthesia, burning discomfort, and temporary neuralgia-type symptoms as recognized issues after donor harvesting.
After an FUE hair transplant, the donor area at the back of the scalp has gone through hundreds or sometimes thousands of tiny excisions. Even though each extraction site is small, the overall donor area is still a healing surgical field. Because of that, it is completely expected for patients to feel some combination of:
- Soreness
- Tenderness
- Bruised Feeling
- Tightness
- Burning
- Numbness
- Tingling
- Increased Sensitivity
In some patients, that discomfort feels more nerve-like than wound-like. Instead of a dull ache, they describe a sharp, stinging, electric, or pinching sensation when the donor area touches a pillow or anywhere. That kind of contact triggered pain can happen because small sensory nerves and surrounding tissue are temporarily irritated during the extraction and healing process. Deeper punch penetration in the graft extraction process or nerve irritation may lead to pain, hyperesthesia, neuralgia, or burning sensation in the donor area.
So yes, in principle, a patient can have a donor area that hurts sharply when it touches the pillow and still be within the spectrum of normal early recovery.
Why Can Donor Area Hurt After Fue Hair Transplant?
There are a few possible reasons.
1) Temporary Donor Area Nerve Irritation
During FUE, the punch works around the follicular units in the donor region. Even when the surgery is performed correctly, tiny superficial sensory nerve branches can become irritated. When those nerves are irritated, patients may describe the sensation as burning, shooting, electric, stinging, or sharply painful when touched.
In other words, the scalp may not simply feel “sore.” It may feel over-sensitive.
This is why some patients can tolerate sitting, standing, or walking relatively well, but the moment the back of the head touches a pillow, the pain becomes much more intense. Complications associated with FUE include hyperesthesia, neuralgia, and burning sensations, which are recognized as potential donor area symptoms resulting from nerve irritation.
2) Ongoing Post Operative Inflammation
Even if the donor area looks acceptable on the surface, the deeper tissues are still healing. The inflammatory phase of wound healing is still active, and pressure on the area can amplify pain disproportionately. That is especially true at night, because contact is prolonged and repeated over the same region.
A patient may think, “The area does not look terrible, so why does it hurt this much?”
The answer is that pain intensity and external appearance do not always match perfectly in the first postoperative week.
3) Mechanical Pressure from Pillows, Neck pillows
This is very common.
Many patients are told to sleep elevated and use a travel pillow, which is generally good advice in the first days. But sometimes the setup is not as protective as it seems. The donor area may still be intermittently touching:
- the bed behind the neck pillow
- the edge of the travel pillow
- the sofa back
- the car seat headrest
- a hard or uneven cushion
So the pain is not necessarily happening “for no reason.” It may be that a healing donor area is being repeatedly compressed in a very sensitive zone.
4) Less Commonly, A Complication That Should Be Ruled Out
This is the part patients should not ignore.
Not all strong pain means infection or another complication. But severe pain can sometimes be a warning sign, especially if it is worsening rather than improving.
General wound infection guidance consistently lists these warning signs:
- increasing pain
- redness
- heat
- swelling
- yellow or green discharge
- bad smell
- wound opening
- fever or feeling unwell
A hematoma at the donor site may cause pain and swelling, and although infection is uncommon, it remains a known postoperative risk. If the pain in the donor area becomes severe and is accompanied by redness, warmth, worsening swelling, drainage, or fever, it should not be considered typical postoperative discomfort.
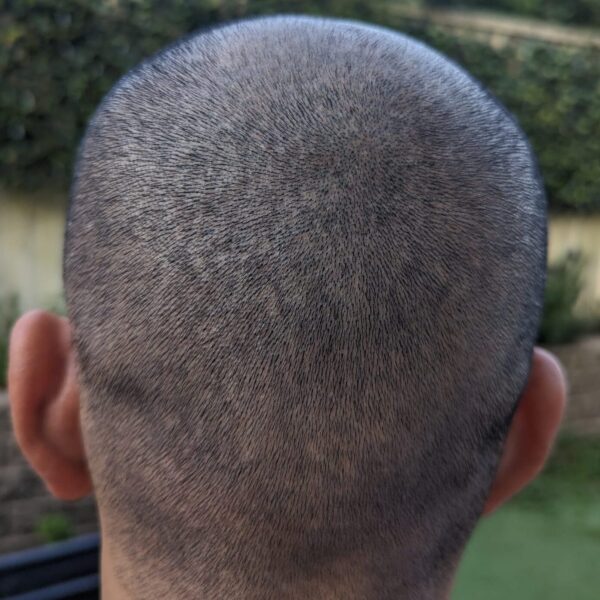
Is Severe Donor Area Pain Normal?
It can still be part of normal recovery, but it is not what I would call typical or average.
That distinction matters.
If a patient tells me:
- the pain happens mainly when the back of the head touches something
- there is no fever
- there is no pus
- there is no foul smell
- there is no obvious spreading redness
- there is no rapidly increasing swelling
- and otherwise the patient feels okay
Then my first thought is usually donor hypersensitivity / nerve irritation, not necessarily infection.
That is the reassuring side.
But if the pain is:
- getting worse each day
- becoming constant even without touch
- accompanied by visible inflammation
- associated with discharge or fever
- or severe enough to feel completely out of proportion
It deserves attention, context, and follow-up.
What should a patient do in the meantime?
Inform the clinic
This is the first step.
In practical terms, I would usually ask the patient to send:
- a clear photo of the donor area from behind
- one photo from each side
- whether pain medication is helping
- whether there is any redness, swelling, discharge, or fever
Avoid direct pressure on the donor area
This sounds obvious, but many patients are still accidentally leaning onto the donor region.
Sometimes small adjustments make a big difference:
- keep the head centered
- avoid slumping backward
- make sure the donor area is not pressing into the pillow edge
- avoid hard chair backs and headrests
- do not rest the scalp against firm surfaces for long periods
Continue the prescribed postoperative medications exactly as instructed
If the surgeon prescribed analgesics, antibiotics, or anti-inflammatory medication, they should be taken exactly as directed. A patient should not start adding or changing post-op medication casually without checking with the clinic first.
Continue gentle aftercare
The donor area should be washed exactly as instructed by the clinic. Patients should not rub, scratch, pick crusts, or apply random creams or oils to the area unless specifically advised.
Watch for signs that change the photo.
Some symptoms are much more reassuring than others.
A tender donor area that looks clean and gradually improves is one thing.
A donor area that becomes more painful, red, hot, swollen, or starts oozing is another.
When should the patient seek prompt medical review?
I would advise prompt contact with the clinic if any of the following are present:
- pain is worsening rather than easing
- the donor area becomes increasingly red
- the skin feels hot to the touch
- swelling is becoming more noticeable
- there is yellow or green discharge
- there is an unpleasant smell
- the patient has fever, chills, or feels generally unwell
- the pain becomes severe even without pressure on the area
Those are reasonable red flags, not overreactions.
A word about hair transplant forums
This is something I often tell patients.
Online discussions can be useful, but they can also be misleading. One patient may say, “I had no pain at all.” Another may say, “I couldn’t sleep for a week.” Both stories may be true.
Pain after FUE is not experienced equally by everyone.
It can vary depending on:
- individual pain sensitivity
- how many grafts were extracted
- donor density
- scalp characteristics
- exact donor zone used
- postoperative swelling and inflammation
- how much pressure is being placed on the area during sleep
So it is not wise to panic just because your recovery does not look identical to someone else’s.
At the same time, it is also not wise to ignore a symptom just because somebody online said they had the same thing.