- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 10 Minutes
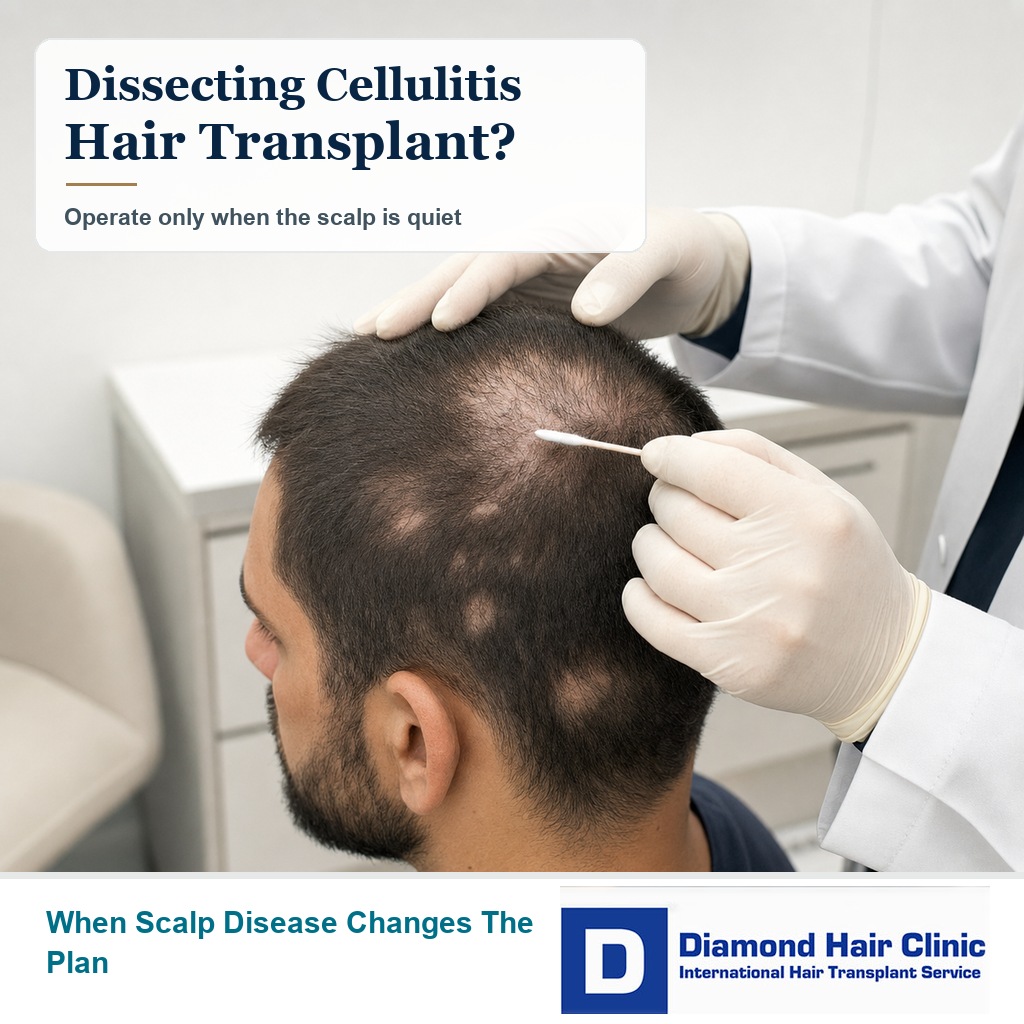
Can I Have a Hair Transplant After Dissecting Cellulitis of the Scalp?
A hair transplant after dissecting cellulitis of the scalp may be possible in carefully chosen patients, but only when the disease is quiet, the diagnosis is clear, the scarred area is stable, and the donor area is safe. If there are still painful bumps, drainage, crusting, pus, swelling, or new patches of hair loss, surgery should wait. A transplant can move healthy follicles into a suitable area, but it cannot control active dissecting cellulitis.
Active disease should be treated before donor grafts are used. The safest decision usually comes from separating two issues. First, is the scalp disease controlled? Second, is the bald area a stable scar that can accept grafts responsibly?
If either answer is uncertain, using donor grafts too early can turn a medical scalp problem into a repair problem.
Why does dissecting cellulitis change the hair transplant decision?
Dissecting cellulitis changes the decision because the scalp may not behave like normal recipient area skin. This condition can create deep inflammation around follicles, abscess-like swelling, draining tracts, scarring, and permanent patches of alopecia. A routine hair transplant plan is not enough for that kind of history.
In ordinary pattern hair loss, I mainly judge donor capacity, hairline design, hair caliber, recipient area size, and future hair loss. With dissecting cellulitis, I need to judge whether the disease is still active under the skin.
That difference matters. If the disease is active, new grafts are being placed into an unstable field. The operation may be technically possible, but it may still be a poor use of donor hair.
This overlaps with the broader article on hair transplant surgery with scarring alopecia, but dissecting cellulitis deserves its own discussion because the inflammation can be deeper, recurrent, and more destructive than an ordinary scar.
How do I know whether the bald patch can still recover?
The first question is whether the follicles are truly destroyed. Some patients have temporary shedding around inflammation. Some have broken hairs, inflamed follicles, or thinning that may improve when the disease is treated. Others have smooth scarred areas where the follicles have been permanently lost.
I do not judge this from one photo. I look for follicular openings, skin texture, tenderness, scale, drainage history, old photos, treatment response, and whether the area has changed over time.
A patch that has been quiet and unchanged for a long period may be a different surgical question from a patch that was swollen or draining last month. If the scalp is still moving, surgery is usually premature.
The distinction also matters because some patients confuse dissecting cellulitis with ordinary folliculitis before a hair transplant. Small surface pustules and deep tract-forming inflammation are not the same surgical problem.
I separate true scarring from hair that has simply become thin around inflammation. If short hairs are returning, if the skin still has follicular openings, or if the area improved after treatment, a medical recovery window may still exist. Surgery should not replace proper diagnosis.
When should surgery wait?
Surgery should wait when there are active painful nodules, pus, draining tunnels, wet crusts, swelling, heat, spreading redness, or new patches of hair loss. I also delay if antibiotics or isotretinoin were recently started, stopped, or changed and the scalp has not yet shown stable behavior.
A patient may feel desperate when a scarred patch remains after months of treatment. I understand that pressure, especially when the area is visible under light or after a short haircut. But the donor area is limited, and grafts should not be spent into a scalp that is still inflamed.
Waiting can feel frustrating, but it may protect the final result. If the disease flares again after surgery, the patient may blame the transplant when the real issue is ongoing scalp disease.
If the concern is an early wound after surgery, pus, odor, fever, or worsening pain after a recent procedure, the separate guide on infection after a hair transplant is more urgent. This article is about candidacy after dissecting cellulitis, not home diagnosis of an active infection.

When can a transplant be considered?
A transplant can be considered when the diagnosis is confirmed, the disease has stayed quiet, the skin is not tender or draining, and the bald area appears stable. The donor area must also be strong enough and separate from the disease process.
The plan should usually be conservative. Scarred skin may not accept density in the same way as healthy scalp. Blood supply, skin thickness, old tracts, and previous inflammation can all reduce the margin for error.
In some cases, surgery may be discussed only as a limited cosmetic improvement, not full restoration. A patient with a small stable scarred patch may have a more realistic option than a patient with widespread unstable disease across the crown and donor region.
Here, being a good candidate for a hair transplant means more than having enough bald skin. The scalp disease, donor strength, timing, and expectation all need to fit together.
How long should the scalp stay quiet before grafts are used?
Patients often want an exact waiting period. I cannot give the same number to every case, but I do not consider the scalp ready just because antibiotics dried the area for a few weeks. For dissecting cellulitis, I usually want at least 12 months of quiet behavior before cosmetic grafting is discussed. In more destructive, recurrent, or heavily scarred cases, 1 to 2 years of stability may be more responsible.
Quiet means more than the patch looking dry in a photo. I want no painful nodules, no drainage, no sinus tracts, no pus, no wet crusting, no expanding patches, no recent rescue medication, and no uncertainty from the dermatologist about whether the disease is still active.
If the disease returns every time medicine stops, the transplant discussion is too early. The surgeon should be able to explain why the chosen area is a stable scar rather than active dissecting cellulitis. That is the difference between careful reconstruction and spending donor hair into a moving disease.
What should be checked before donor grafts are used?
Before donor grafts are used, I need the medical picture to be clear. A dermatologist’s diagnosis is important, and in unclear cases trichoscopy or biopsy may be needed before surgery is even discussed. The operation should not be planned around guesswork.
Treatment history matters. Antibiotics, isotretinoin, steroid injections, biologic medication, medicated shampoo, previous drainage, and flare timing can all change the timing of surgery.
The donor area needs careful examination. If the donor area has scarring, repeated inflammation, low density, or miniaturization, the surgery may become much more limited. A large graft quote in that situation can be a warning sign.
If the donor region itself has active painful nodules, drainage, or unstable patches, I do not treat that as a simple density problem. The source of grafts may not be safe enough yet, even if the bald scar in the recipient area looks ready.
Medical screening may also matter because some patients with dissecting cellulitis have other inflammatory or follicular occlusion conditions. Blood tests before a hair transplant can clarify medical readiness before the cosmetic plan becomes the focus.

Can FUE place grafts into scarred scalp?
FUE can sometimes place grafts into scarred scalp, but scarred scalp is less forgiving than normal skin. The grafts still need blood supply, correct depth, careful spacing, and a recipient area that is not inflamed.
A scar from old trauma, a surgical scar, and a scar created by dissecting cellulitis do not behave exactly the same. A DCS scar may sit in skin that previously had deep inflammation, tracts, abscesses, and repeated tissue damage. I judge that history before making the decision how dense the placement can be.
The general principles of hair transplant into scar tissue still apply. The difference is that the disease must be quiet first. Treating a scar is one thing. Transplanting into a scalp that may flare again is another.
If FUE is used, I plan the work in a measured way instead of packing grafts aggressively into questionable tissue. A staged approach may be safer when the skin quality is uncertain.
What graft number and density are realistic?
The graft number depends on the size of the stable scarred area, the strength of the donor area, the blood supply of the recipient skin, and how much coverage the patient expects. A serious number should not come from a few phone photos.
Scarred skin often needs more conservative density planning. Trying to force normal density coverage into scarred or previously inflamed tissue can weaken graft survival and create a harsher repair later.
The donor area also has to be protected. A patient who has already lost hair from inflammation may need donor grafts for future repair, crown thinning, or pattern hair loss later. The broader page on the donor area explains why donor hair should be treated as a lifetime reserve, not an unlimited supply.
If the bald patch is large, a patient may need to accept partial improvement rather than a dense natural-looking scalp. In scarred or medically complex skin, a modest plan that heals well is better than an ambitious plan that fails.
How do medications change the timing?
Medication changes can affect timing because they tell us whether the disease is still being controlled. If a patient has just finished antibiotics and the scalp flares again, that is not a stable surgical window. If isotretinoin or another treatment has recently started, I need to see how the scalp behaves before planning surgery.
Patients should not stop dermatology medication by themselves to become eligible for a transplant. The priority is disease control. A cosmetic operation should fit around medical stability, not compete with it.
Medication planning also matters around the operation itself. Antibiotic use, stomach tolerance, allergy history, retinoid timing, anti-inflammatory treatment, and other prescriptions should be reviewed before surgery. The article on antibiotics after a hair transplant explains why medication decisions should be individualized rather than copied from another patient.
If another doctor is managing the skin disease, the hair transplant plan should respect that treatment plan. Poor communication between doctors can create unnecessary risk.
What should make a clinic promise feel unsafe?
A clinic promise feels unsafe when the disease history is ignored. If nobody asks about drainage, abscesses, active bumps, biopsy, dermatology treatment, medication, remission length, donor quality, or scar stability, the transplant quote is not complete.
Be especially careful when the answer is only a high graft number. In a dissecting cellulitis case, the graft quote should come after the scalp has been judged, not before. A number offered before diagnosis and stability have been reviewed is not a medical plan.
I become concerned when a clinic treats the scar as ordinary empty skin. The scalp may look quiet in one photo, but old tracts, fragile skin, and disease recurrence risk can change the plan.
If the patient already had a poor operation or rushed plan elsewhere, bad hair transplant repair becomes a harder discussion. Repair after a rushed decision is usually harder than making the first surgical decision slowly.
How should I think about future flares after surgery?
A future flare is part of the risk discussion. Even if the scalp is quiet before surgery, dissecting cellulitis can be recurrent in some patients. That risk needs review before grafts are used.
The patient should understand what to do if new painful bumps, drainage, or swelling appears after surgery. Early dermatology review is safer than squeezing lesions, applying random products, or waiting until scarring increases.
Aftercare should also be more careful in a patient with this history. Clean washing, avoiding scratching, avoiding dirty hats or pressure, and direct follow-up matter. The broader hair transplant aftercare guide is useful, but a patient with previous DCS may need more individualized follow-up than a routine case.
I also document the scalp before surgery with clear photos. Later, if a symptom appears, comparison is easier. A patient should not be left guessing whether a new bump is ordinary healing, folliculitis, or recurrence of the original disease.
Follow up should be practical. If a new painful lump appears, the patient should know who to contact, what photos to send, and when local medical review is needed. Vague reassurance is not enough when the history includes deep inflammation and scarring.
What is the right next step if I have this condition?
If you have active dissecting cellulitis, the next step is medical control, not a transplant date. See a dermatologist, treat the inflammation, document the diagnosis, and wait until the scalp proves that it is quiet.
If your disease has been quiet and you are left with stable bald scarred patches, then a hair transplant consultation can be reasonable. The consultation should include donor assessment, recipient skin assessment, discussion of density limits, and a realistic explanation of what surgery can and cannot improve.
Do not let embarrassment or frustration push you into a fast package. Dissecting cellulitis can leave visible scars, but donor grafts are precious. They should be used only when the scalp gives them a fair chance.
My approach is careful and staged when needed. First control the disease. Then confirm stability. Then decide whether the scarred area, donor area, and patient expectation make surgery responsible.
When the answer is yes, the plan should be conservative enough to heal and natural enough to look like hair, not a repair attempt that creates a new problem.


