- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 8 Minutes
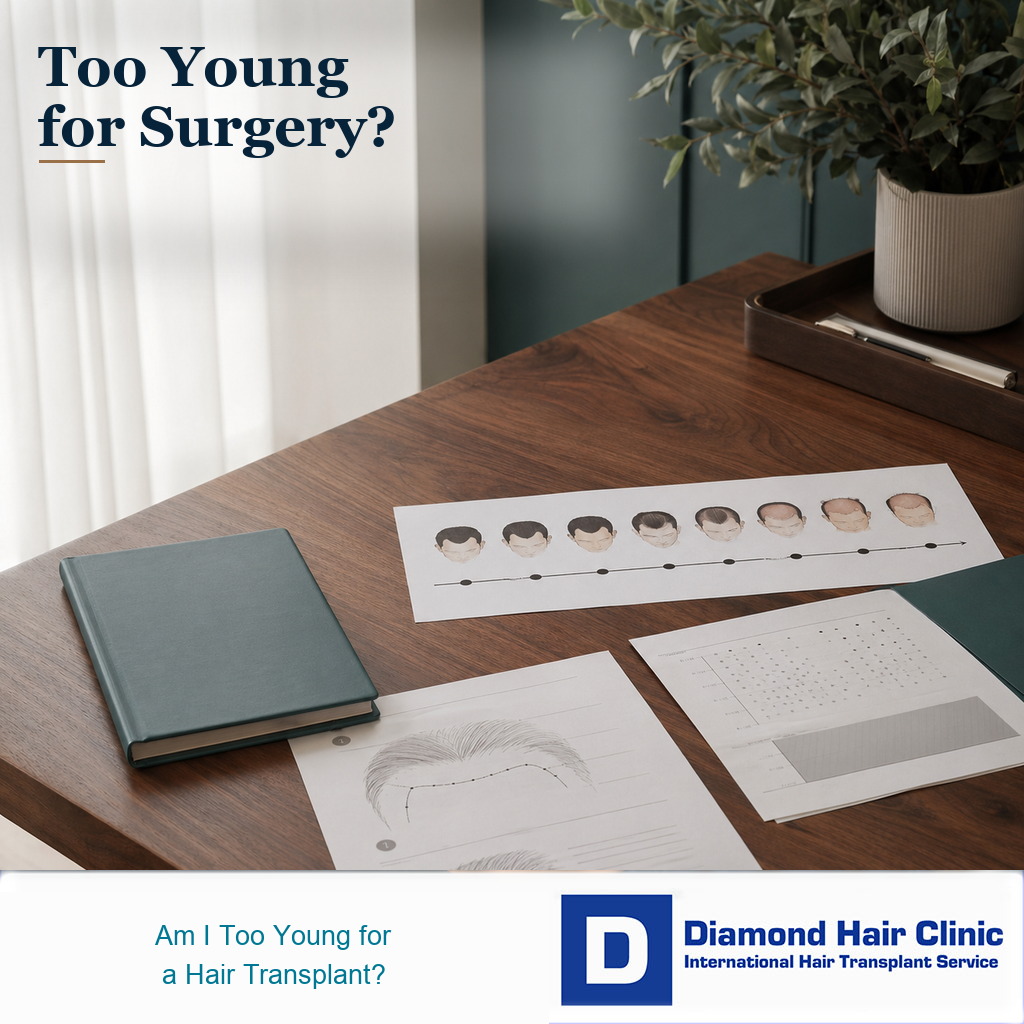
Age and Donor Planning Before FUE Surgery
You may be too young for a hair transplant if your hair loss is still changing, your donor area has not been properly assessed, or your goal is to rebuild a teenage hairline. Age alone is not the decision. I look at stability, donor capacity, family history, medication options, expectations, and whether the plan will still look natural years from today. For men who are no longer very young but still have decades of possible change ahead, hair transplant in your 30s planning needs its own future hair loss logic. family hair loss history review makes that future risk reading more precise.
When hair loss starts early, the urgency can feel very real. A young patient may feel watched by every mirror, every photo, and every comment about their hair. That emotional pressure deserves respect, but it cannot be allowed to rush a permanent surgical decision.
A young patient may need to delay a hair transplant with medication before any permanent design is chosen. Sometimes that delay protects the future result more than an early operation ever could.
The useful distinction is not age by itself. A 23 year old with stable, limited recession and a mature plan is different from a 23 year old with rapid thinning, crown changes, and a request for a very low hairline. The same birthday can carry very different surgical risk. A focused Norwood 3 transplant planning discussion helps when early temple recession is already more than a mature hairline.
Young age is not an automatic no, but it raises the burden of proof. The consultation cannot ask only whether surgery is possible. It needs to ask whether surgery now will still look wise when the patient is 30, 40, and older. I start with whether the patient is truly a good candidate for a hair transplant, not with a graft number or a package price.
The opposite age question needs the same discipline because a hair transplant in your 40s or 50s depends on donor reserve, health stability, and lifetime coverage rather than age alone.
Ages 18 to 24 need extra caution
Quite often, 18 to 24 is too young for a hair transplant. Not because the hair loss is imaginary, and not because a young patient must simply accept it. The weak point is that the future pattern is often still unclear.
Male pattern hair loss can move quickly during the late teenage years and twenties. A patient may have temple recession today, but the middle scalp, crown, or area behind the new hairline may thin later.
If surgery is done too aggressively at the beginning, the patient may look better for a short period and then face a harder problem later. The transplanted hair may remain in front while the native hair behind it continues to disappear.
This is how some young patients end up with an isolated transplanted hairline, low density behind it, and fewer donor grafts left for correction. That is not a small planning mistake. It can shape the rest of the patient’s hair restoration life.
There are exceptions. A young patient with a scar, stable traction alopecia, or a clearly limited problem can be different from a young patient with active androgenetic hair loss. Even then, the diagnosis, donor quality, and expectations must be clear before surgery is discussed seriously.
Young age is a warning light. It tells me to slow down, examine more carefully, and plan further ahead.

Surgical risk comes from pattern, stability, and expectations
The first risk is active hair loss. If the hairline is changing quickly, shedding is still strong, or miniaturization is spreading, surgery may be premature.
The second risk is treating surgery as a cure for hair loss. A hair transplant moves hair from one area to another. It does not stop the biology that caused the original hair loss.
The third risk is emotional pressure. I meet young patients who want surgery because they are tired of hiding their forehead, avoiding photos, or comparing themselves with other people. I take that seriously. It is not vanity to be concerned about your appearance.
Still, emotion must not set the surgical plan faster than the medical facts allow. A patient who feels desperate may accept a low hairline, a large graft number, or a clinic that says yes too quickly.
The fourth risk is an unrealistic target. A very low, flat, dense hairline may look exciting immediately after surgery, but it can look artificial as the patient matures.
In a young patient, the plan needs to improve the frame of the face without spending too many grafts too early. A strong result is not the youngest possible hairline. It is a hairline that fits the face now and still looks natural later.
Donor planning matters more when the future is long
The donor area is limited. It is not an endless source of hair, and I cannot treat it as if every graft can be used today without consequence.
When I examine a young patient, I think about the donor area like a lifetime reserve. Some of it may be used now, but enough must remain for possible future needs.
This makes donor area management especially important in younger patients. The younger the patient, the longer the future we must protect.
A young patient may ask for maximum density in the frontal hairline. That wish is understandable. But if that density consumes too many grafts too early, the crown or middle scalp may become difficult to manage later.
I do not calculate grafts only by looking at the empty area today. I also consider future hair loss, donor density, hair caliber, contrast between hair and skin, family history, and the patient’s long term priorities.
The way I calculate the graft number for a hair transplant is never copied from another patient’s photos. Two young patients with similar temples can need very different plans.
Medication may need discussion before surgery
Very often, yes. If the patient has androgenetic hair loss, I need to understand whether the native hair can be stabilized before committing donor grafts to surgery. That means a serious discussion about medical treatment before a hair transplant.
Medication is not a fixed rule for every young patient. Some patients cannot use certain medicines, some do not want them, and some have diagnoses where they are not relevant. But a young patient must not ignore stabilization simply because surgery feels more decisive.
Finasteride, dutasteride, minoxidil, oral minoxidil, PRP, and other options each need proper medical discussion. Benefits, limits, side effects, monitoring, and personal suitability matter. A young patient must not start, stop, or combine medication based only on fear or online comments.
If the native hair is not stable, surgery may only chase the loss. The hairline may be restored, but the surrounding hair may continue to thin. That can create a new problem around a technically surviving transplant.
For the same reason, having a hair transplant without finasteride deserves careful discussion. Some patients can still be candidates, but the plan may need to be more conservative and the expectations must be very clear.
Waiting 6 to 12 months to observe stabilization can be the smarter decision in a young patient. Waiting for the right timing and the right surgeon is sometimes the decision that protects the final result.

Steps before deciding at 18, 20, or 24
Start with diagnosis. Not every young person with thinning has the same problem. Pattern hair loss, diffuse thinning, telogen shedding, low ferritin, thyroid issues, scalp inflammation, traction, alopecia areata, and medication related shedding can look similar to a worried patient.

Document the hairline, middle scalp, crown, donor area, and family pattern with clear photos under consistent lighting. A few months of accurate comparison often teaches more than one dramatic mirror check on a bad day.
Review the speed of change. Hair loss that has changed very little for several years is different from hair loss that worsened during the last six months. Recent acceleration changes the surgical conversation.
If medication is appropriate, the patient needs to understand what it may and may not do. The purpose is not to force every young patient into medication. The purpose is to avoid using surgery while the surrounding hair is still unstable.
Then discuss a design that respects the future. The hairline needs to be attractive, but it must not spend the donor reserve as if the patient will never lose more hair.
If a clinic skips these steps and moves straight to a large graft number, slow down. A young patient needs more examination, not faster sales language.
Young hairlines need mature planning
In a young patient, the hairline cannot be designed only for the face and hair loss pattern the patient has today. It also needs to respect the face they will carry as they become older.
A natural hairline is not only low. It has the right height, shape, irregularity, density, and direction for the patient’s face and future hair loss risk.
Natural and age appropriate hairline design needs so much attention. A natural hairline does not announce that surgery was done.
A very low hairline can use too many grafts and create an unnatural frame. In young patients, this mistake is often driven by impatience, aggressive marketing, or the wish to recreate teenage hair.
A hair transplant must not try to freeze the face at 17. It needs to create a mature improvement that still makes sense years later.
Low and flat hairlines need extra caution in young patients. They can look impressive at first, but the future cost can be high if the patient continues to lose hair behind them.
Waiting can protect the final result
Waiting can protect the result when the diagnosis is unclear, the hair loss is still active, the donor area needs more evaluation, or the patient is making the decision under strong emotional pressure.
Waiting can also protect the result when medication has just started. A patient who begins treatment and books surgery immediately may never learn whether the native hair was about to improve, stabilize, or continue thinning.
A structured waiting period is not wasted time. It can be used for monthly photos, medical evaluation, stabilization, family pattern review, and a more realistic design conversation.
There is another benefit. Waiting often separates medical planning from sales pressure. A proper consultation can explain what information is needed before surgery. A sales driven clinic usually pushes the patient to choose a date before the difficult questions are answered.
Some young patients fear that waiting means losing their chance. In reality, premature surgery can remove choices from the future. Donor grafts used too early cannot be put back. This is the same donor protection logic behind being declined for hair transplant when the timing is unsafe.
Emotional distress deserves respect, not rushed surgery
The emotional side of early hair loss must not be dismissed. A young patient may avoid dating, photos, swimming, bright lighting, or social events because of their hair. These feelings can be heavy.

But a painful emotion does not always make surgery the safest first step. Sometimes the kindest answer is to stabilize, observe, and plan rather than operate immediately.
If the distress is severe, the consultation needs to separate two questions. What can be improved now, and what needs to be protected for the future?
For some patients, medical treatment, hairstyle changes, fibers, or understanding the real pattern can reduce panic enough to make a better decision. For others, a small and conservative surgery may eventually be reasonable.
The decision must never come from shame, pressure, discounts, or a clinic telling the patient that delay means failure. A young patient deserves protection from regret, not only a fast operation.
Clinic behavior that should slow a young patient down
A young patient needs caution if the clinic immediately gives a large graft number without explaining diagnosis, donor limits, future loss, and hairline strategy.
They also need caution if the first conversation is mainly with a salesperson, not with a doctor who is responsible for the surgical plan.
A clinic that says yes too quickly to a young patient may not be protecting that patient. Sometimes the ethical answer is not now, not this hairline, or not this many grafts.
Large volume clinics can be especially risky when they treat young patients as easy cases. A young patient with anxiety can be persuaded by discounts, urgency, package language, and dramatic before and after photos.
Young patients need to know the red flags of hair transplant clinics before choosing where to have surgery.
Price also matters, but not in the way many patients think. The cheapest option may become very expensive if the donor area is damaged, the hairline is unnatural, or the patient needs repair surgery later.
When comparing hair transplant cost in Turkey, look beyond the number and ask what kind of medical responsibility is included in the price.
Questions to ask before surgery as a young patient
Ask what diagnosis the clinic is treating. Ask whether the hair loss appears stable or active. Ask whether the donor area is strong enough not only for this surgery, but for possible future needs.
Ask who designs the hairline, who makes the recipient area openings, who performs extraction, who places grafts, and who decides if the plan must change on the day of surgery. If responsibility is unclear, the patient is not being protected.
Ask how many grafts are planned for the hairline, middle scalp, and crown. A total number alone is not enough. Distribution shows the thinking behind the surgery.
Ask what would make the surgeon say no. A clinic that never refuses young patients, never recommends waiting, and never adjusts the plan downward is not showing medical judgment.
Also ask what happens if hair loss continues after the transplant. A young patient needs to understand that native hair may keep changing, because hair loss can continue after a hair transplant.
These questions are not meant to make the patient afraid. They are meant to make the decision adult, clear, and safer.
When surgery may be reasonable for a young patient
I may consider surgery in a young patient when the diagnosis is clear, the hair loss is stable enough, the donor area is suitable, and the patient understands that future planning matters more than instant transformation.
The patient needs to know the limits of surgery. A good transplant can improve the hairline and density, but it cannot promise that future hair loss will stop.
If surgery is appropriate, I choose a conservative and strategic plan. The number of grafts needs to be enough to create a meaningful improvement, but not so high that it sacrifices the future.
The technique also matters, but technique is only one part of the result. Whether I use Sapphire FUE or another suitable approach, the most important question is whether the plan is correct for that patient.
At Diamond Hair Clinic, my priority is careful planning over volume. Protecting a young patient from premature surgery is better than performing an operation that looks attractive today and creates problems tomorrow.
If you are 18, 22, or 24 and thinking about a hair transplant, do not ask only whether surgery can be done. Ask whether the timing is right, whether your donor area is protected, whether your hair loss is understood, and whether the surgeon is planning for your future self.
A young patient does not always need to wait forever. But they do need a careful plan, an ethical surgeon, and enough patience to avoid a mistake that cannot easily be undone.


