- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 10 Minutes

Repairing Hairline Advancement Scars With Transplant Surgery
A hair transplant can sometimes soften or camouflage a scar from surgical hairline advancement, forehead reduction, or a previous forehead-shortening procedure. It should not be treated like ordinary hairline lowering. The scar has to be mature, soft enough, well supplied with blood, and positioned in a way that grafts can grow in a natural direction. I usually want the scar to be reviewed after at least 9 to 12 months of healing, and sometimes longer if the tissue is still red, firm, raised, painful, or changing. Scar tissue is less predictable than normal scalp, so the plan often needs fewer grafts at first, lower density expectations, and a staged approach.
The patient usually wants to know whether the line can be hidden. The medical answer has to be more careful. A visible forehead-reduction scar may improve with transplanted hair, but the result depends on the scar itself, the surrounding hair direction, skin tension, hair caliber, donor reserve, and whether another procedure would create a better surface before grafting. If the first decision is rushed, the patient can waste valuable donor hair on tissue that was not ready to receive it.
How is this different from lowering a naturally high forehead?
A patient with a naturally high forehead usually has intact skin at the future hairline. When lowering a naturally high forehead with hair transplant, the main questions are facial proportion, age-appropriate placement, future hair loss, density, and donor management.
A hairline advancement scar is different because the front border already contains operated tissue. The surgeon is not only designing a lower hairline. The surgeon is deciding whether grafts can survive in scarred skin, whether the scar should be crossed or softened, whether the hairline should sit just in front of it, and whether the old operation changed the natural movement of the forehead skin. That makes the case closer to hair transplant into scar tissue than to a routine cosmetic lowering case.
If the patient also has male or female pattern hair loss, the decision becomes more complex. A forehead-reduction scar may be the visible problem today, but future thinning can expose a low or dense front line later. The repair should not solve one scar while creating an unnatural hairline that ages badly.
When is the scar mature enough to review?
The scar should look and feel stable before grafting is planned. A mature scar is usually flatter, paler, less tender, less itchy, and less reactive than it was in the early months. Redness, firmness, pain, thickening, or widening means the tissue is still active or under tension. A red, raised, painful, or widening scar should not be rushed into grafting just because the patient is embarrassed by it.
Nine to 12 months is a common review window, but it is not a magic permission date. Some scars settle earlier; some need longer. A patient with thick scarring, keloid tendency, repeated surgery, inflammation, or ongoing tightness may need dermatology or scar-revision input before any transplant plan is discussed. The decision should be based on the tissue, not only on the calendar.
If the patient has a history of raised scars, chest or shoulder keloids, hypertrophic scars, or unusual wound healing, that history must be reviewed before new surgical sites are created. Scar behavior changes the surgical threshold. That also matters for keloid scars and hair transplant risk.
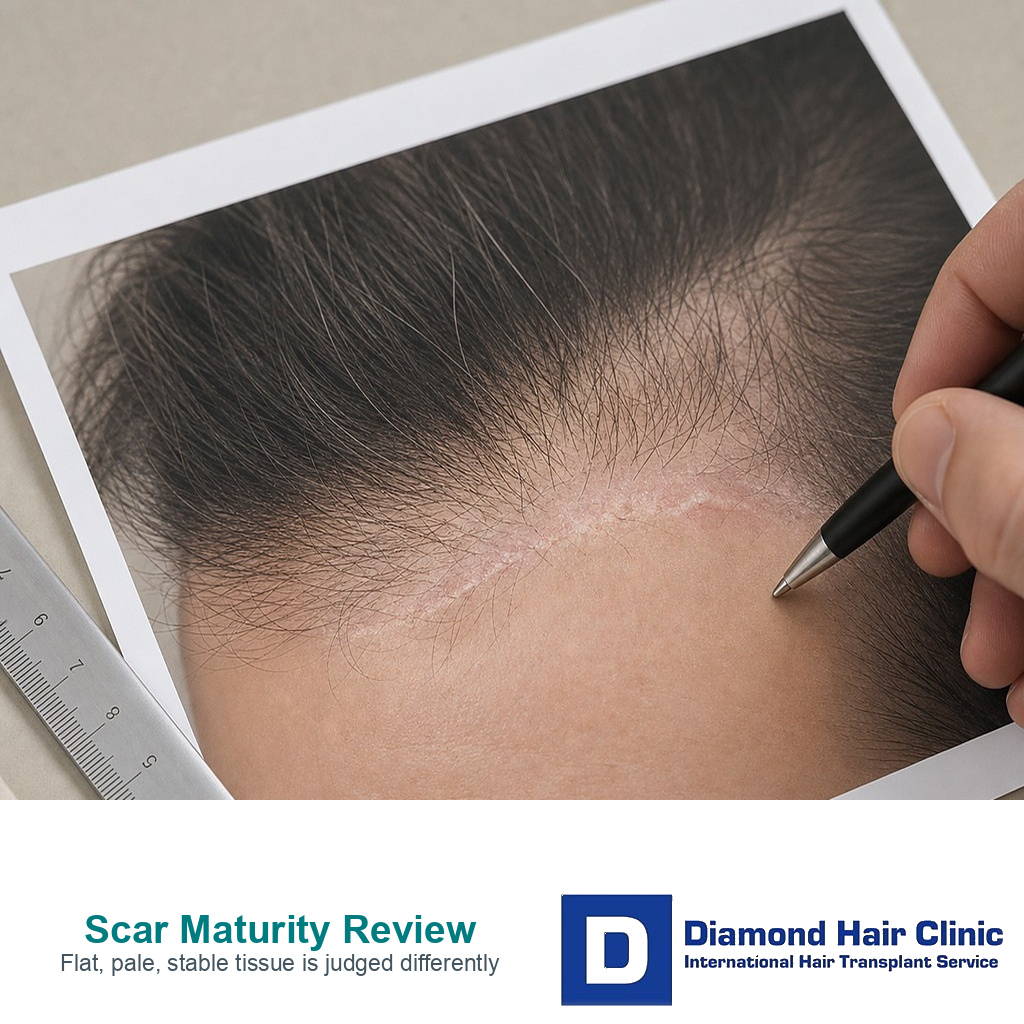
What makes grafting into scar tissue less predictable?
Normal scalp has better blood supply, softer tissue, and more predictable healing. Scar tissue can be tighter, stiffer, and less vascular. That matters because every transplanted follicle needs a good environment in the first days and weeks after placement. Dense packing that might be reasonable in normal skin may be too aggressive for a scar.
The angle is also less forgiving. Hair along the front hairline should not grow straight forward like a brush. It has to follow a soft, irregular direction that matches the surrounding hairs. When grafts are placed through or around a scar, the surgeon may have less flexibility because the tissue resists the incision angle. Hair direction matters as much as coverage in a visible front hairline scar.
A scar case can fail even if hair grows. The scar may be partly hidden, but if the direction is wrong, the repair can look artificial. Patients worried about this point should also understand wrong hair direction after hair transplant, because direction errors are difficult to disguise at the hairline.
Which scars are poor candidates?
A scar is a poor candidate when it is still active, thick, painful, red, unstable, very wide, infected, or under strong tension. It is also a poor candidate when the patient expects the transplanted hair to erase the scar completely. Hair can soften a line and reduce contrast, but a scar may still be visible under harsh light, wet hair, short styling, or close inspection.

Some patients have more than a surgical scar. They may have scarring alopecia, frontal fibrosing alopecia, lichen planopilaris, traction alopecia, or another inflammatory diagnosis near the hairline. If the medical diagnosis is active, transplant surgery may be unsafe or disappointing. For scarring alopecia and transplant candidacy, stability has to be proven before grafts are moved.
A poor candidate can sometimes become a better candidate later after scar treatment, waiting, scar revision, or medical control. But some scars should not be grafted. If graft survival is unlikely, donor hair should not be sacrificed for a result that cannot be responsibly promised.
How should the new hairline be designed around an old scar?
The new hairline must be designed around the face, the scar, and the future. It should not simply be drawn low enough to cover every millimeter of the old line. If the new hairline is too low, too straight, or too dense, the patient may trade a scar problem for an unnatural hairline problem.
The repair often works better when the hairline is built with irregularity, softer density at the edge, and careful direction that lets the hair fall naturally over the scar. The scar may be grafted directly in selected areas, partly crossed, or partly camouflaged by hair placed just in front of it. The plan depends on scar position and tissue quality.
Temple points also need careful planning. A forehead-reduction scar can tempt the surgeon to close the temples too aggressively, especially when the patient wants a smaller forehead. Temple work is one of the places where small design mistakes are very visible. With temple point restoration, direction, density, and age-appropriate shape matter.
Does the hairline have to be lowered again to hide the scar?
Not always. This is an important design decisions in a hairline advancement scar repair. If the scar is just behind or inside the natural front edge, a small number of grafts may be used through the scar and around it without meaningfully lowering the whole hairline. If the scar sits lower or wider, trying to cover every part of it by drawing a new line in front can make the forehead too short or the hairline too rounded.
I do not judge scar coverage only by whether the line disappears in a close photograph. I also look at facial proportion, temple shape, hair direction, future hair loss risk, and whether the new outline will still look natural years later. In some patients, the better plan is partial camouflage, scar revision first, or a staged transplant rather than a lower, denser hairline that creates a new cosmetic problem.
Does Afro-textured or very curly hair change the plan?
Yes. Curly hair can give helpful visual coverage, but extraction and placement are technically more demanding because the follicle may curve under the skin. Around a hairline scar, the surgeon also has to respect curl direction, hair exit angle, and the way the hair will sit when it grows long enough to cover the line.
A scar after hairline advancement in a patient with Afro-textured or very curly hair should not be treated as a fast high-density case. The donor extraction must be conservative, the punch angle must respect the hidden curl, and the hairline should not be packed so tightly that graft survival or natural flow is weakened. A smaller, controlled first session can be more protective than an aggressive repair that spends too much donor hair before the scar response is known.
Patients with this hair type can read more about Afro-textured and very curly hair transplant challenges. The same technical caution becomes even more important when the recipient area is scarred.
Should scar coverage be done in one session?
Sometimes a small scar can be treated in one careful session. A longer, wider, tight, or less vascular scar may be safer as a staged plan. The first session can test the tissue response, establish a soft front edge, and show how the grafts grow before more donor hair is committed.
A staged first session can protect the donor area. This is especially true when the patient has already had another operation, has limited donor reserve, or wants a dense cosmetic change at the front. If the first stage grows well, a second stage may refine the density. If the first stage grows poorly, the surgeon has learned something important without spending too much donor hair.
This differs from a routine hair transplant touch-up. A touch-up usually adjusts a small weak area after an otherwise reasonable transplant. Scar coverage has a tissue-quality problem built into the case, so the density target must be more conservative.
What records and photos should be prepared?
Before consultation, prepare clear photos from the front, both oblique angles, both sides, close hairline views, top scalp, and donor area. Use dry hair, similar lighting, and no hair fibers or heavy styling product. If the old scar is hard to see in soft lighting, include one plain harsh-light photo too. A surgeon needs to see both the cosmetic concern and the real tissue surface.
If you have the operative report from the hairline advancement or forehead reduction, bring it. The incision position, scar history, healing problems, revision attempts, steroid injections, laser treatments, and timing all matter. If the case involves a prior hair transplant as well, graft counts, photos, and donor records become even more important.
Photo-only planning has limits in scar cases. It can help decide whether a case is worth examining, but it cannot fully judge scar texture, mobility, thickness, or blood supply. With hair transplant planning from photos, some decisions need in-person assessment.
When is scar revision, SMP, or waiting better than grafting?
Grafting is not the only option. If the scar is wide, raised, very tight, or badly positioned, scar revision may be considered before or instead of transplantation. Scar revision and grafting are not the same decision. Revision tries to improve the surface or position of the scar; grafting tries to camouflage the line with hair. If the scar is flat but contrast is the main problem, scalp micropigmentation may help some patients, especially when the hair is kept short. If the scar is still changing, waiting may be the more protective medical decision.

There are also cases where another repair creates more risk than benefit. A patient with a low artificial hairline, weak donor area, active inflammation, or unrealistic density expectations may need a different plan. If the old procedure produced an unnatural result, the broader repair logic overlaps with bad hair transplant repair, but scar coverage still has its own tissue problem.
The decision should compare the cosmetic gain against the donor cost. If a few hundred grafts can soften a mature scar and improve styling freedom, the plan may be reasonable. If thousands of grafts are needed to hide a scar and rebuild a low hairline, the patient must understand what that means for future hair loss and later repair options.
What should a patient ask before accepting the repair plan?
Ask what the surgeon sees in the scar, not only how many grafts are being offered. The answer should mention tissue maturity, width, color, softness, surrounding hair direction, donor limits, expected density, and whether a staged approach is advised. Ask whether the surgeon plans to graft directly into the scar, in front of it, behind it, or in a combination pattern.
Also ask what would make the surgeon delay or refuse the case. A thoughtful answer protects you. It means the clinic is treating the scar as living tissue, not as an empty space to fill. If the surgeon cannot explain why the scar is suitable, how density will be limited, or what happens if the first session grows less than expected, the patient should pause and seek another opinion.
A second opinion before more surgery is especially useful when the scar came from a previous cosmetic operation, when the first clinic promised easy coverage, or when the patient is emotionally tired from trying to hide the line. The aim is not to collect more opinions until one clinic says yes. The aim is to understand whether grafting the scar is a medically sound use of the remaining donor hair.
Repairing a hairline advancement scar can be possible when the tissue, donor supply, and hairline design support the plan, but the promise should be modest and specific. The scar may become softer in appearance, the hairline may frame the face more naturally, and styling may become easier. It should still be planned as scar surgery, not routine hairline lowering. The result is more reliable when the tissue is respected first and the hair is designed around it.


