- Written by Dr.Mehmet Demircioglu
- Estimated Reading Time 11 Minutes

Thin Hair Transplant at 7 Months: Growth Timeline and Next Steps
At 7 months after a hair transplant, a thin result can still be normal, especially if the crown was treated, the hair is fine, or the new hairs are still short and soft. It is not the final result yet.
But month 7 is late enough that the pattern deserves a proper look. I judge whether there is steady change, whether the scalp is healthy, whether the transplanted zone matches the original plan, and whether native hair loss is making the result look thinner than expected.
The mistake is to decide from one harsh light photo or one bad mirror day. The other mistake is to accept vague reassurance when nothing is changing at all. A month 7 review should be structured, photographic, and clinical. A careful comb-through video can be useful, but it should be compared with month-by-month progress rather than used as a single verdict.
If there is visible progress, fine new hairs, and a settled scalp, waiting is usually reasonable. If there is no visible progress, increasing patchiness, pain, redness, crusting, or a pattern that looks wrong compared with the surgical plan, a proper review is needed.
What does a thin result at 7 months usually mean?
A thin result at 7 months often means the transplant is still maturing, but it can also reveal an underpowered plan, slow growth, crown delay, ongoing native hair loss, or poor graft survival. The month number alone does not diagnose the case.
At this stage, I separate three things. First, are transplanted hairs actually growing but still fine and see through? Second, is the area improving compared with month 4, month 5, and month 6? Third, is the thin look coming from the transplanted zone, the surrounding native hair, or the crown where growth can be slower? The six-month density check is the record that makes that comparison cleaner.
A month five hair growth check can make that comparison cleaner before month seven, especially when the worry is slow but visible movement rather than a completely silent area.
A month 7 result should not be judged only by density. I compare it with the original graft placement, the hairline design, the crown plan, donor capacity, hair caliber, and the patient’s photos over time. A result that looks thin but is steadily improving is different from a result that has shown almost no change for several months. If the worry is no longer only thinness but whether the front looks natural, a month eight hairline check gives the review a clearer structure.
For patients who check too often, learning to track hair transplant growth without panicking is usually more useful than daily mirror checks.
Why can month 7 still be too early to judge the final result?
Month 7 is not the final result because transplanted hair does not only appear. It also changes caliber, length, texture, and visual coverage over time. A patient may see growth, but the hairs can still be fine, wiry, uneven, or too short to create the final illusion of density. A later one-year FUE result review should then separate normal maturation from a real density or design problem.
The front is often easier to judge earlier than the crown. Even then, I usually need to see how the hair behaves closer to 9 to 12 months before making a strong judgment about density. In slower cases, and especially in the crown, the more mature picture may take closer to 15 to 18 months.
Some poor results will not become good simply because the patient waits. Month 7 should be interpreted with evidence. I look for direction of change. More small hairs, better coverage in similar lighting, and improving texture are good signs. No change at all, worsening scalp symptoms, or a clear mismatch between the implanted area and the plan needs review.
The wider density issue is why some hair transplant results look thin. Month 7 is one specific point inside that bigger judgment.
What signs are reassuring at month 7?
The most reassuring sign at month 7 is not perfect density. It is clear movement in the right direction. I look for new hairs breaking through, older new hairs getting darker or thicker, and the treated area looking better in the same lighting than it did at month 4 or month 5.
Fine, soft hairs in the same thin area are different from a smooth-looking gap where I cannot see new shafts at all. Both can worry a patient, but they do not mean the same thing clinically.
A settled scalp is also reassuring. Mild sensitivity can still happen, but the recipient area should not look angry, crusted, infected, or persistently inflamed. A healthy scalp with slow improvement is usually a different situation from a thin result with redness, pain, repeated pimples, or crusting.
Hair length matters more than patients realize. A new hair that is only a few centimeters long cannot cover the scalp the same way a mature, longer hair can. If the hair is short, soft, and still changing, I usually avoid making a final density judgment too early.
How is month 7 different from month 4?
Month 4 is often too early for density judgment. Some patients are only beginning to see growth. At month 7, I still allow room for maturation, but I expect the case to give me more information than it did at month 4.
If a patient was very thin at month 4 but now has many new fine hairs, the direction is encouraging. If month 4, month 5, month 6, and month 7 all look almost identical, that is not proof of failure, but the details deserve a more careful review.
The location matters as well. A frontal hairline that has almost no visible growth at 7 months is a different concern from a crown that is slowly thickening but still see through. Hair characteristics matter too. Fine straight hair can look weaker under light than thicker, wavier hair with the same graft count.
A low-density month 4 picture carries a different meaning than a month 7 picture. I explain that earlier stage separately in low density 4 months after a hair transplant. Month 7 deserves a firmer review, but still not a rushed verdict.
Why does the crown often look thin for longer?
The crown can look thin for longer because it is a difficult area to cover. Hair direction rotates, the scalp is viewed from above, and light reflects directly onto the area. Even a technically good crown transplant can look less dense than the patient hoped at month 7.
The crown also consumes many grafts if the patient expects complete coverage. A surgeon has to think about the future, not only the photograph at one stage of recovery. If the patient still has progressive hair loss, filling the crown aggressively too early can spend donor grafts that may be needed later for more visible areas.
When I review a crown at month 7, I look at the whorl direction, graft distribution, hair caliber, the untreated surrounding crown, and whether the patient had enough grafts for the area treated. Sometimes the transplant is still maturing. Sometimes the original crown plan was too ambitious for the donor budget.
Patients with crown anxiety should understand the limits of crown hair transplant planning, because the crown is one of the easiest areas for clinics to oversimplify.
Could native hair loss make the transplant look worse at 7 months?
Yes. A transplant can be growing while the surrounding native hair is thinning. When that happens, the patient may feel that the transplant failed, but the real issue is a mixed picture. Some implanted hairs are maturing, while native hair around them is losing density.
This is common in patients who had surgery while their hair loss was still active. It can also happen if medication was stopped, changed, or never used in a patient with ongoing androgenetic hair loss. The transplanted area and the native hair do not always behave the same way.
Shock loss can also confuse the picture earlier in recovery. Temporary native hair shedding usually appears earlier than month 7, but if native hair has not recovered as expected, the result may still look thin. The separate discussion on native hair shock loss after a hair transplant is useful when the thinning seems to involve existing hair, not only grafts.
The long-term issue is that hair loss can continue after a hair transplant. At month 7, that distinction can protect a patient from blaming the wrong cause.
Does no shedding change how I judge a month 7 result?
No shedding by itself does not tell me that the result will be better or worse. Some patients shed most transplanted hairs in the early weeks. Some shed gradually. Some appear to keep many short hairs and still go through a quiet growth phase afterward.
At month 7, I focus less on whether the patient remembers a classic shedding phase and more on what the scalp is doing now. Are new hairs visible? Is the density improving? Are the hairs gaining length and caliber? Is the scalp healthy? These questions matter more than the exact shedding story.
Patients sometimes panic because their recovery did not match the timeline they saw online. Recovery can vary, so I look for medically plausible progress rather than one exact timeline.
If shedding was unusual or barely happened, no shedding after a hair transplant still does not decide graft survival by itself.
When does thinness at 7 months deserve a review?
Thinness at 7 months deserves a review when there is almost no visible progress from earlier months, when the transplanted zone has clear empty areas, when one side behaves very differently from the other without a good reason, or when scalp symptoms continue.
I also review the case if the patient has pain, persistent redness, pimples, crusting, infection concern, or irritation that does not fit the normal healing stage. A settled scalp with slow improvement is one situation. An unhealthy scalp with no progress is another.
The review should include the original plan, graft count by area, implantation pattern, pre-surgery photos, day one photos if available, month-by-month photos, donor assessment, medical treatment history, and current scalp condition. Without those details, reassurance has little value.
Medication changes, stopping minoxidil or finasteride, a new shedding trigger, scalp inflammation, illness, or strong stress during recovery all matter. These details do not excuse a weak surgical result, but they can explain why the visual picture is confusing.
A proper month 7 review is not only about saying wait longer. It is about deciding whether the pattern is still within a normal maturation window.
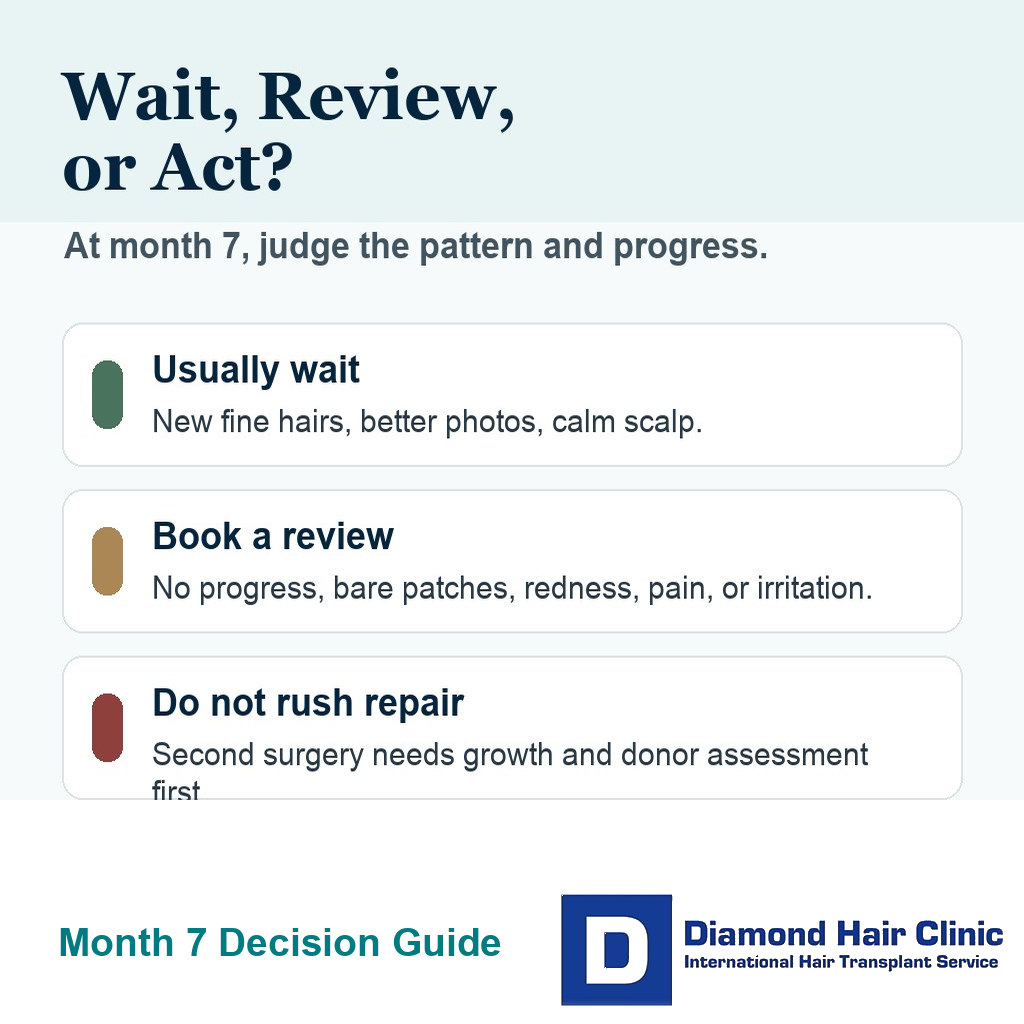
What should I avoid doing too quickly?
The first thing to avoid is planning repair surgery too early. A second procedure before the first result has matured can waste donor grafts, disturb a developing result, and create a plan based on anxiety rather than evidence.

Avoid changing several treatments at once without medical guidance. If a patient starts, stops, or changes minoxidil, finasteride, dutasteride, supplements, PRP, or other treatments all at the same time, it becomes harder to understand what helped, what irritated the scalp, and what caused shedding.
Gentle handling, consistent photos, and proper communication with the surgical team are more useful than panic decisions. If medication is part of the long-term plan, the timing and consistency around minoxidil after a hair transplant should be discussed instead of changed in panic.
If a second operation is being discussed, first ask whether a second hair transplant is worth it from donor safety, timing, and the original plan. A repair or second session should not be planned from frustration alone.
What clinic promises should I question at this stage?
At month 7, be careful with any promise that sounds too certain before the case has been examined. A clinic cannot responsibly diagnose a thin result from one photo, one message, or one phrase such as “normal, wait.” It also cannot responsibly promise that repair will fix everything without checking donor capacity and the original plan.
Be especially careful with clinics that use month 7 anxiety to sell a second surgery quickly. A patient who is worried can be easy to pressure. The better review is slower. It should explain what is still maturing, what may be underperforming, what can be improved later, and what should not be touched yet.
The graft number from the first surgery also needs context. A 4,000 graft operation spread across a large area may look thinner than the same number used in a smaller frontal zone. A crown focused plan may need more patience. A case with ongoing native loss may need medical stabilization before any new surgery is considered.
When I judge whether a patient was suitable for the original operation, I return to candidacy. Grafts alone never define a safe plan. Keep that in mind with good candidate for a hair transplant.
How should I compare my photos without panicking?
Use the same room, same light, same hair length, same camera distance, and the same angles once a month. Wet hair, harsh bathroom light, overhead flash, and different styling can make the scalp look much thinner than it looks in normal life.
The most useful comparison sets show the front, both temples, mid-scalp, crown, donor area, and normal social distance. Close detail photos are useful for detail, but they can exaggerate scalp visibility. A patient also needs to know how the result looks to another person, not only under a phone camera five centimeters from the scalp.
Do not compare your month 7 result with another patient’s final result, different graft count, different hair caliber, different hair loss class, or different lighting. That comparison creates anxiety but not medical judgment.
Wet hair, hair pushed apart with fingers, fibers, concealers, and direct overhead light can all make a developing transplant look different from normal life. Clear photos still matter, but the harshest possible photo should not become the only truth.
Your own case matters more than another patient’s timeline. Month-by-month progress in the same conditions gives a better answer than scrolling through other people’s best photos.
How do I judge a month 7 result in consultation?
I start with the original problem. Was the surgery for a small frontal zone, a broad frontal and mid-scalp area, or the crown? Then I compare the graft number with the size of the treated area, the donor strength, hair caliber, hair direction, and future hair loss risk.
Then I look at progress, not only density. If there are maturing hairs, a settled scalp, and gradual improvement, the result usually deserves more time. If the treated area has poor growth, unhealthy skin, or a pattern that does not match the original plan, I investigate instead of giving generic reassurance.
I also ask whether the patient is judging the result from daily anxiety or from consistent photos. Many month 7 results look disappointing in harsh light but improve clearly by 9 to 12 months. Some crown and slow cases continue maturing beyond that.
At month 7, the safest judgment is balanced. Do not declare failure too early, but do not ignore a result that shows no progress or does not fit the surgical plan.
A good review should leave the patient clearer about three things. Whether waiting is reasonable, whether medical or scalp factors need attention, and whether repair should even be discussed later. That is the difference between patience and passive reassurance.


